Virtual Reality Oculokinetic Perimetry Test Reproducibility and Relationship to Conventional Perimetry and OCT
- PMID: 36276927
- PMCID: PMC9562375
- DOI: 10.1016/j.xops.2021.100105
Virtual Reality Oculokinetic Perimetry Test Reproducibility and Relationship to Conventional Perimetry and OCT
Abstract
Purpose: Vivid Vision Perimetry (VVP; Vivid Vision, Inc) is a novel method for performing in-office and home-based visual field assessment using a virtual reality platform and oculokinetic perimetry. Here we examine the reproducibility of VVP Swift and compare results with conventional standard automated perimetry (SAP) and spectral-domain (SD) OCT.
Design: Cross-sectional study.
Participants: Fourteen eyes of 7 patients with open-angle glaucoma (OAG) (average age, 64.6 years; 29% women) and 10 eyes of 5 patients with suspected glaucoma (average age, 61.8 years; 40% women) were enrolled.
Methods: Patients with OAG and suspected glaucoma were enrolled prospectively and underwent 2 VVP Swift examinations. Results were compared with 1 conventional SAP examination (Humphrey Visual Field [HVF]; Zeiss) and 1 SD OCT examination.
Main outcome measures: Mean sensitivity (in decibels) obtained for each eye in 2 VVP Swift test sessions and a conventional SAP examination, thickness of the retinal nerve fiber layer (RNFL) and ganglion cell complex (GCC) for the SD OCT examination, and mean test durations of the VVP Swift and SAP examinations.
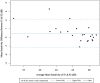
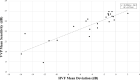
Results: The mean test duration of VVP Swift in both eyes (8.5 minutes) was significantly shorter (P < 0.001) than SAP (12.2 minutes). The average absolute difference of the mean sensitivity between the 2 VVP Swift sessions was found to be 0.73 dB (95% confidence interval [CI], 0.40-1.06). A statistically significant association was found between average mean sensitivity measurements from the VVP and mean deviation (MD) measurements obtained by the HVF with a Pearson correlation coefficient of 0.86 (95% CI, 0.70-0.94; P < 0.001). Mean visual sensitivity measurements from the VVP Swift test were significantly associated with average RNFL thickness (r = 0.66; P = 0.014) and GCC thickness (r = 0.63; P = 0.02), whereas the correlation coefficients between HVF MD and RNFL and GCC were 0.86 (P < 0.001) and 0.83 (P < 0.001), respectively.
Conclusions: Our results demonstrated that the VVP Swift test can generate reproducible results and is comparable with conventional SAP. This suggests that the device can be used by clinicians to assess visual function in glaucoma.
Keywords: CI, confidence interval; GCC, ganglion cell complex; Glaucoma; HVF, Humphrey Visual Field; MD, mean deviation; OAG, open-angle glaucoma; OCT; Oculokinetic perimetry; Perimetry; RNFL, retinal nerve fiber layer; SAP; SAP, standard automated perimetry; SD, spectral-domain; Tele-ophthalmology; VVP, Vivid Vision Perimetry; Virtual reality; Visual field.
© 2021 by the American Academy of Ophthalmology.
Figures

References
-
- Hudson C., Wild J.M., O’Neill E.C. Fatigue effects during a single session of automated static threshold perimetry. Invest Ophthalmol Vis Sci. 1994;35(1):268–280. - PubMed
-
- Schimiti R.B., Avelino R.R., Newton K.J., Costa V.P., et al. Full-threshold versus Swedish Interactive Threshold Algorithm (SITA) in normal individuals undergoing automated perimetry for the first time. Ophthalmology. 2002;109(11):2084–2092. discussion 2092. - PubMed
-
- Wu Z., Saunders L.J., Daga F.B., et al. Frequency of testing to detect visual field progression derived using a longitudinal cohort of glaucoma patients. Ophthalmology. 2017;124(6):786–792. - PubMed
Grants and funding
LinkOut - more resources
Full Text Sources
Miscellaneous

