Screening and characterization of vaginal fluid donations for vaginal microbiota transplantation
- PMID: 36289360
- PMCID: PMC9606370
- DOI: 10.1038/s41598-022-22873-y
Screening and characterization of vaginal fluid donations for vaginal microbiota transplantation
Abstract
Bacterial vaginosis (BV), the overgrowth of diverse anaerobic bacteria in the vagina, is the most common cause of vaginal symptoms worldwide. BV frequently recurs after antibiotic therapy, and the best probiotic treatments only result in transient changes from BV-associated states to "optimal" communities dominated by a single species of Lactobacillus. Therefore, additional treatment strategies are needed to durably alter vaginal microbiota composition for patients with BV. Vaginal microbiota transplantation (VMT), the transfer of vaginal fluid from a healthy person with an optimal vaginal microbiota to a recipient with BV, has been proposed as one such alternative. However, VMT carries potential risks, necessitating strict safety precautions. Here, we present an FDA-approved donor screening protocol and detailed methodology for donation collection, storage, screening, and analysis of VMT material. We find that Lactobacillus viability is maintained for over six months in donated material stored at - 80 °C without glycerol or other cryoprotectants. We further show that species-specific quantitative PCR for L. crispatus and L. iners can be used as a rapid initial screening strategy to identify potential donors with optimal vaginal microbiomes. Together, this work lays the foundation for designing safe, reproducible trials of VMT as a treatment for BV.
© 2022. The Author(s).
Conflict of interest statement
The authors declare no competing interests.
Figures


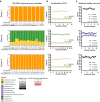
References
Publication types
MeSH terms
Substances
Grants and funding
LinkOut - more resources
Full Text Sources

