Long-Term Psychosocial Consequences of Whole-Body Magnetic Resonance Imaging and Reporting of Incidental Findings in a Population-Based Cohort Study
- PMID: 36292045
- PMCID: PMC9600583
- DOI: 10.3390/diagnostics12102356
Long-Term Psychosocial Consequences of Whole-Body Magnetic Resonance Imaging and Reporting of Incidental Findings in a Population-Based Cohort Study
Abstract
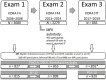
Management of radiological incidental findings (IF) is of rising importance; however, psychosocial implications of IF reporting remain unclear. We compared long-term psychosocial effects between individuals who underwent whole-body magnetic resonance imaging (MRI) with and without reported IF, and individuals who did not undergo imaging. We used a longitudinal population-based cohort from Western Europe. Longitudinal analysis included three examinations (exam 1, 6 years prior to MRI; exam 2, MRI; exam 3, 4 years after MRI). Psychosocial outcomes included PHQ-9 (Patient Health Questionnaire), DEEX (Depression and Exhaustion Scale), PSS-10 (Perceived Stress Scale) and a Somatization Scale. Univariate analyses and adjusted linear mixed models were calculated. Among 855 included individuals, 25% (n = 212) underwent MRI and 6% (n = 50) had at least one reported IF. Compared to MRI participants, non-participants had a higher psychosocial burden indicated by PHQ-9 in exam 1 (3.3 ± 3.3 vs. 2.5 ± 2.3) and DEEX (8.6 ± 4.7 vs. 7.7 ± 4.4), Somatization Scale (5.9 ± 4.3 vs. 4.8 ± 3.8) and PSS-10 (14.7 ± 5.7 vs. 13.7 ± 5.3, all p < 0.05) in exam 3. MRI participation without IF reporting was significantly associated with lower values of DEEX, PHQ-9 and Somatization Scale. There were no significant differences at the three timepoints between MRI participants with and without IF. In conclusion, individuals who voluntarily participated in whole-body MRI had less psychosocial burden and imaging and IF reporting were not associated with adverse long-term psychosocial consequences. However, due to the study design we cannot conclude that the MRI exam itself represented a beneficial intervention causing improvement in mental health scores.
Keywords: incidental findings; longitudinal study; magnetic resonance imaging; mental health; whole body imaging.
Conflict of interest statement
The authors declare no conflict of interest. The funders had no role in the design of the study; in the collection, analyses, or interpretation of data; in the writing of the manuscript; or in the decision to publish the results.
Figures

Similar articles
-
Incidental findings in whole-body MR imaging of a population-based cohort study: Frequency, management and psychosocial consequences.Eur J Radiol. 2021 Jan;134:109451. doi: 10.1016/j.ejrad.2020.109451. Epub 2020 Nov 28. Eur J Radiol. 2021. PMID: 33279799
-
Impact of whole-body MRI in a general population study.Eur J Epidemiol. 2016 Jan;31(1):31-9. doi: 10.1007/s10654-015-0101-y. Epub 2015 Nov 23. Eur J Epidemiol. 2016. PMID: 26597793
-
Psychosocial consequences and severity of disclosed incidental findings from whole-body MRI in a general population study.Eur Radiol. 2013 May;23(5):1343-51. doi: 10.1007/s00330-012-2723-8. Epub 2012 Dec 13. Eur Radiol. 2013. PMID: 23239059
-
Whole-body MRI for preventive health screening: A systematic review of the literature.J Magn Reson Imaging. 2019 Nov;50(5):1489-1503. doi: 10.1002/jmri.26736. Epub 2019 Apr 1. J Magn Reson Imaging. 2019. PMID: 30932247 Free PMC article.
-
Whole-body magnetic resonance imaging (WB-MRI) for cancer screening in asymptomatic subjects of the general population: review and recommendations.Cancer Imaging. 2020 May 11;20(1):34. doi: 10.1186/s40644-020-00315-0. Cancer Imaging. 2020. PMID: 32393345 Free PMC article. Review.
Cited by
-
Observations Regarding the Detection of Abnormal Findings Following a Cancer Screening Whole-Body MRI in Asymptomatic Subjects: The Psychological Consequences and the Role of Personality Traits Over Time.J Magn Reson Imaging. 2025 Feb;61(2):634-645. doi: 10.1002/jmri.29461. Epub 2024 May 31. J Magn Reson Imaging. 2025. PMID: 38821883 Free PMC article.
-
Incidental findings on non-contrast abdominal computed tomography in an asymptomatic population: Prevalence, economic and health implications.PLoS One. 2025 Aug 4;20(8):e0328049. doi: 10.1371/journal.pone.0328049. eCollection 2025. PLoS One. 2025. PMID: 40758690 Free PMC article.
References
-
- Bamberg F., Hetterich H., Rospleszcz S., Lorbeer R., Auweter S.D., Schlett C.L., Schafnitzel A., Bayerl C., Schindler A., Saam T., et al. Subclinical Disease Burden as Assessed by Whole-Body MRI in Subjects with Prediabetes, Subjects with Diabetes, and Normal Control Subjects from the General Population: The KORA-MRI Study. Diabetes. 2017;66:158–169. doi: 10.2337/db16-0630. - DOI - PubMed
-
- Hegenscheid K., Seipel R., Schmidt C.O., Völzke H., Kühn J.-P., Biffar R., Kroemer H.K., Hosten N., Puls R. Potentially relevant incidental findings on research whole-body MRI in the general adult population: Frequencies and management. Eur. Radiol. 2013;23:816–826. doi: 10.1007/s00330-012-2636-6. - DOI - PubMed
-
- Bamberg F., Kauczor H.U., Weckbach S., Schlett C.L., Forsting M., Ladd S.C., Greiser K.H., Weber M., Schulz-Menger J., Niendorf T., et al. Whole-Body MR Imaging in the German National Cohort: Rationale, Design, and Technical Background. Radiology. 2015;277:206–220. doi: 10.1148/radiol.2015142272. - DOI - PubMed
-
- Padhani A.R., Lecouvet F.E., Tunariu N., Koh D., de Keyzer F., Collins D.J., Sala E., Schlemmer H.P., Petralia G., Vargas H.A., et al. METastasis Reporting and Data System for Prostate Cancer: Practical Guidelines for Acquisition, Interpretation, and Reporting of Whole-body Magnetic Resonance Imaging-based Evaluations of Multiorgan Involvement in Advanced Prostate Cancer. Eur. Urol. 2017;71:81–92. doi: 10.1016/j.eururo.2016.05.033. - DOI - PMC - PubMed
-
- Messiou C., Hillengass J., Delorme S., Lecouvet F.E., Moulopoulos L., Collins D., Blackledge M.D., Abildgaard N., Østergaard B., Schlemmer H.-P., et al. Guidelines for Acquisition, Interpretation, and Reporting of Whole-Body MRI in Myeloma: Myeloma Response Assessment and Diagnosis System (MY-RADS) Radiology. 2019;291:5–13. doi: 10.1148/radiol.2019181949. - DOI - PubMed
Grants and funding
LinkOut - more resources
Full Text Sources
Miscellaneous

