Acanthosis Nigricans: Pointer of Endocrine Entities
- PMID: 36292208
- PMCID: PMC9600076
- DOI: 10.3390/diagnostics12102519
Acanthosis Nigricans: Pointer of Endocrine Entities
Abstract
Acanthosis nigricans (AN) has been reported in relation to insulin resistance (IR). We aim to review AN through an endocrine and metabolic perspective focusing on IR in association with metabolic complications such as obesity, diabetes mellitus (DM), and metabolic syndrome (MS) with/without polycystic ovary syndrome (PCOS). We revised English papers on PubMed covering publications from the last 5 years. The current prevalence of AN varies from 4.5 to 74% (or even 100%, depending on the studied population), with equal distribution among females and males. Despite higher incidence with an age-dependent pattern, an alarming escalation of cases has been noted for obesity and MS in younger populations. Most frequent IR-associated sites are the neck, axilla, and knuckles, but unusual locations such as the face have also been reported. Quantitative scales such as Burke have been used to describe the severity of the dermatosis, particularly in correlation with IR elements. Dermoscopic examination are required, for instance, in cases with sulcus cutis, hyperpigmented spots, crista cutis, and papillary projections. A skin biopsy may be necessary, but it is not the rule. Both IR that clinically manifests with or without obesity/MS correlates with AN; most studies are cross-sectional, with only a few longitudinal. The approach varied from screening during school periodic checkups/protocols/programs to subgroups of individuals who were already known to be at high cardio-metabolic risk. AN was associated with type2DM, as well as type 1DM. Females with PCOS may already display metabolic complications in 60-80% of cases, with AN belonging to the associated skin spectrum. AN management depends on underlying conditions, and specific dermatological therapy is not generally required, unless the patient achieves metabolic control, has severe skin lesions, or desires cosmetic improvement. In IR cases, lifestyle interventions can help, including weight control up to bariatric surgery. In addition, metformin is a key player in the field of oral medication against DM type 2, a drug whose indication is extended to PCOS and even to AN itself, outside the specific panel of glucose anomalies. In terms of cosmetic intervention, limited data have been published on melatonin, urea cream, topical retinoids, vitamin D analogs, or alexandrite laser. In conclusion, awareness of IR and its associated clinical features is essential to provide prompt recognition of underlying conditions. AN represents a useful non-invasive surrogate marker of this spectrum in both children and adults. The pivotal role of this dermatosis could massively improve endocrine and metabolic assessments.
Keywords: acanthosis nigricans; diabetes mellitus; endocrine; glucose; insulin resistance; metabolic syndrome; obesity; polycystic ovary syndrome.
Conflict of interest statement
The authors declare no conflict of interest.
Figures
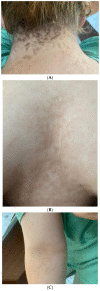

Similar articles
-
Therapeutic implications of dermoscopic findings in acanthosis nigricans: A clinical and histopathological study.Dermatol Ther. 2020 Nov;33(6):e14521. doi: 10.1111/dth.14521. Epub 2020 Nov 26. Dermatol Ther. 2020. PMID: 33176058
-
Correlation of acanthosis nigricans with insulin resistance, anthropometric, and other metabolic parameters in diabetic Indians.Indian J Endocrinol Metab. 2012 Dec;16(Suppl 2):S436-7. doi: 10.4103/2230-8210.104122. Indian J Endocrinol Metab. 2012. PMID: 23565457 Free PMC article.
-
Clinico-investigative Study of Facial Acanthosis Nigricans.Indian Dermatol Online J. 2022 Mar 3;13(2):221-228. doi: 10.4103/idoj.IDOJ_855_20. eCollection 2022 Mar-Apr. Indian Dermatol Online J. 2022. PMID: 35287408 Free PMC article.
-
Acanthosis Nigricans: An Updated Review.Curr Pediatr Rev. 2022;19(1):68-82. doi: 10.2174/1573396318666220429085231. Curr Pediatr Rev. 2022. PMID: 36698243 Review.
-
Acanthosis nigricans: A review.J Cosmet Dermatol. 2020 Aug;19(8):1857-1865. doi: 10.1111/jocd.13544. J Cosmet Dermatol. 2020. PMID: 32516476 Review.
Cited by
-
Paraneoplastic Syndromes in Gallbladder Cancer: A Systematic Review.Medicina (Kaunas). 2025 Feb 27;61(3):417. doi: 10.3390/medicina61030417. Medicina (Kaunas). 2025. PMID: 40142228 Free PMC article.
-
New Perspectives on Nutraceutical Insulin Sensitizing Agents in the Treatment of Psoriasis and Other Dermatological Diseases.Int J Mol Sci. 2025 Aug 4;26(15):7538. doi: 10.3390/ijms26157538. Int J Mol Sci. 2025. PMID: 40806666 Free PMC article. Review.
-
Impact of Comorbid Polycystic Ovary Syndrome on Clinical and Laboratory Parameters in Female Adolescents with Metabolic Dysfunction-Associated Steatotic Liver Disease: A Cross-Sectional Study.J Clin Med. 2024 Oct 2;13(19):5885. doi: 10.3390/jcm13195885. J Clin Med. 2024. PMID: 39407944 Free PMC article.
-
Hyperandrogenism and Cardiometabolic Risk in Pre- and Postmenopausal Women-What Is the Evidence?J Clin Endocrinol Metab. 2024 Apr 19;109(5):1202-1213. doi: 10.1210/clinem/dgad590. J Clin Endocrinol Metab. 2024. PMID: 37886900 Free PMC article. Review.
-
Trichloroacetic Acid 15% Peel Alone versus in Combination with Microneedling in Patients with Acanthosis Nigricans.J Clin Aesthet Dermatol. 2024 Apr;17(4):28-32. J Clin Aesthet Dermatol. 2024. PMID: 38638182 Free PMC article.
References
Publication types
LinkOut - more resources
Full Text Sources

