Prognostic significance of modified lung immune prognostic index in osteosarcoma patients
- PMID: 36303539
- PMCID: PMC9592918
- DOI: 10.3389/fgene.2022.972352
Prognostic significance of modified lung immune prognostic index in osteosarcoma patients
Abstract
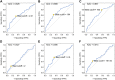
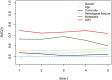
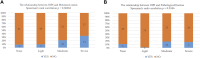
Purpose: Osteosarcoma is the most common primary malignancy of bone with a dismal prognosis for patients with pulmonary metastases. Evaluation of osteosarcoma prognosis would facilitate the prognosis consultation as well as the development of personalized treatment decisions. However, there is limited effective prognostic predictor at present. Lung Immune Prognostic Index (LIPI) is a novel prognostic factor in pulmonary cancers, whereas, the prognostic significance of LIPI in osteosarcoma has not yet been well clarified. In this study, we firstly explore the prognostic role of LIPI and further modify this predictive model in osteosarcoma. Patients and methods: A retrospectively study was conducted at Musculoskeletal Tumor Center of West China Hospital between January 2016 and January 2021. Hematological factors and clinical features of osteosarcoma patients were collected and analyzed. The area under curve (AUC) and optimal cuff-off of each single hematological factor was calculated. Results: In this study, lactate dehydrogenase (LDH), derived neurtrophil to lymphocyte ratio (dNLR), and Hydroxybutyrate dehydrogenase (HBDH) have higher AUC values. LIPI was composed of LDH and dNLR and was further modified by combing the HBDH, forming the osteosarcoma immune prognostic index (OIPI). OIPI divided 223 osteosarcoma patients divided into four groups, none, light, moderate, and severe (p < 0.0001). OIPI has a higher AUC value than LIPI and other hematological indexes in t-ROC curve. According to the univariate and multivariate analysis, pathological fracture, metastasis, NLR, platelet-lymphocyte ratio (PLR), and OIPI were associated with the prognosis; and metastasis and OIPI were independent prognostic factors of osteosarcoma patients. An OIPI-based nomogram was also established and could predict the 3-year and 5-year overall survival. In addition, OIPI was also revealed correlated with metastasis and pathological fracture in osteosarcoma. Conclusion: This study first explore the prognostic significance of LIPI in osteosarcoma patients. In addition, we developed a modified LIPI, the OIPI, for osteosarcoma patients. Both the LIPI and OIPI could predict the overall survival of osteosarcoma patients well, while OIPI may be more suitable for osteosarcoma patients. In particular, OIPI may have the ability to identify some high-risk patients from clinically low-risk patients.
Keywords: inflammation; lung immune prognostic index; osteosarcoma; prognostic predictive factors; tumor immune micro-environment.
Copyright © 2022 He, Tang, Zou, Li, Wang, Kenmegne, Zhou, Lu, Min, Luo and Tu.
Conflict of interest statement
The authors declare that the research was conducted in the absence of any commercial or financial relationships that could be construed as a potential conflict of interest.
Figures




Similar articles
-
A novel model for predicting the prognosis of postoperative intrahepatic cholangiocarcinoma patients.Sci Rep. 2023 Nov 6;13(1):19267. doi: 10.1038/s41598-023-45056-9. Sci Rep. 2023. PMID: 37935735 Free PMC article.
-
Lung Immune Prognostic Index Could Predict Metastasis in Patients With Osteosarcoma.Front Surg. 2022 Jul 8;9:923427. doi: 10.3389/fsurg.2022.923427. eCollection 2022. Front Surg. 2022. PMID: 35874141 Free PMC article.
-
Osteosarcoma immune prognostic index can indicate the nature of indeterminate pulmonary nodules and predict the metachronous metastasis in osteosarcoma patients.Front Oncol. 2022 Jul 22;12:952228. doi: 10.3389/fonc.2022.952228. eCollection 2022. Front Oncol. 2022. PMID: 35936683 Free PMC article.
-
Systemic Inflammatory Markers of Survival in Epidermal Growth Factor-Mutated Non-Small-Cell Lung Cancer: Single-Institution Analysis, Systematic Review, and Meta-analysis.Clin Lung Cancer. 2021 Sep;22(5):390-407. doi: 10.1016/j.cllc.2021.01.002. Epub 2021 Jan 10. Clin Lung Cancer. 2021. PMID: 33582072
-
The Predictive Value of Pretreatment Lactate Dehydrogenase and Derived Neutrophil-to-Lymphocyte Ratio in Advanced Non-Small Cell Lung Cancer Patients Treated With PD-1/PD-L1 Inhibitors: A Meta-Analysis.Front Oncol. 2022 Jul 18;12:791496. doi: 10.3389/fonc.2022.791496. eCollection 2022. Front Oncol. 2022. PMID: 35924149 Free PMC article.
Cited by
-
A novel model for predicting the prognosis of postoperative intrahepatic cholangiocarcinoma patients.Sci Rep. 2023 Nov 6;13(1):19267. doi: 10.1038/s41598-023-45056-9. Sci Rep. 2023. PMID: 37935735 Free PMC article.
-
The combination of baseline neutrophil to lymphocyte ratio and dynamic changes during treatment can better predict the survival of osteosarcoma patients.Front Oncol. 2023 Nov 14;13:1235158. doi: 10.3389/fonc.2023.1235158. eCollection 2023. Front Oncol. 2023. PMID: 38033504 Free PMC article.
-
Antisense mediated blockade of Dickkopf 1 attenuates tumor survival, metastases and bone damage in experimental osteosarcoma.Sci Rep. 2025 Jan 13;15(1):1878. doi: 10.1038/s41598-024-84037-4. Sci Rep. 2025. PMID: 39805917 Free PMC article.
-
The application of lung immune prognostic index in predicting the prognosis of 302 STS patients.Front Oncol. 2024 Sep 9;14:1460600. doi: 10.3389/fonc.2024.1460600. eCollection 2024. Front Oncol. 2024. PMID: 39314631 Free PMC article.
-
Diagnostic value of combined detection of AKP, TSGF, and LDH for pediatric osteosarcoma: a case-control study.Am J Transl Res. 2024 Aug 15;16(8):3667-3677. doi: 10.62347/IGEA4076. eCollection 2024. Am J Transl Res. 2024. PMID: 39262698 Free PMC article.
References
-
- Bielack S. S., Kempf-Bielack B., Delling G., Exner G. U., Flege S., Helmke K., et al. (2002). Prognostic factors in high-grade osteosarcoma of the extremities or trunk: An analysis of 1, 702 patients treated on neoadjuvant cooperative osteosarcoma study group protocols. J. Clin. Oncol. 20 (3), 776–790. 10.1200/jco.2002.20.3.776 - DOI - PubMed
LinkOut - more resources
Full Text Sources

