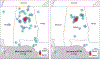
Geographic disparities in peripartum cardiomyopathy outcomes
- PMID: 36309247
- PMCID: PMC10257938
- DOI: 10.1016/j.ajogmf.2022.100788
Geographic disparities in peripartum cardiomyopathy outcomes
Abstract
Background: Cardiomyopathy causes more than a third of late postpartum pregnancy-related deaths in the United States, and racial disparities in outcomes among pregnant individuals with cardiomyopathy exist. Underlying community factors may contribute to disparities in peripartum cardiomyopathy outcomes.
Objective: This study aimed to identify the geographic distribution of and disparities in peripartum cardiomyopathy outcomes, hypothesizing that patients living in communities with higher social vulnerability may have worse outcomes.
Study design: This was a retrospective cohort study of patients with peripartum cardiomyopathy per the National Heart, Lung, and Blood Institute definition from January 2000 to November 2017 at a single center, excluding those with a post office box address as a post office box address may not reflect the census tract in which a patient resides. Severe peripartum cardiomyopathy (vs less severe peripartum cardiomyopathy) was defined as ejection fraction <30%, death, intensive care unit admission, left ventricular assist device or implantable cardioverter defibrillator placement, or transplant. The US census tract for the patient's address was linked to the Centers for Disease Control and Prevention Social Vulnerability Index, a 0 to 1 scale of a community's vulnerability to external stresses on health, with higher values indicating greater vulnerability. The Social Vulnerability Index includes social factors divided into socioeconomic, household composition, minority status, and housing type and transportation themes. The Social Vulnerability Index and Social Vulnerability Index components were compared among patients by peripartum cardiomyopathy severity.
Results: Of 95 patients in the original cohort, 5 were excluded because of the use of a post office box address. Of the remaining 90 patients, 56 met severe peripartum cardiomyopathy criteria. At baseline, individuals with and without severe peripartum cardiomyopathy had similar ages, marital status, payor type, tobacco use, gestational age at delivery, and mode of delivery; however, individuals with severe peripartum cardiomyopathy were more likely to be Black (vs White) (59% vs 29%; P<.007) and less likely to recover ejection fraction (EF) to ≥55% by 12 months (36% vs 62%; P=.02) than individuals with less severe peripartum cardiomyopathy. Patients with severe peripartum cardiomyopathy were more likely to live in areas with a higher Social Vulnerability Index (0.51 vs 0.31; P=.002) and with more residents who were unemployed, impoverished, without a high school diploma, in single-parent households, of minority status, without a vehicle, and in institutionalized group quarters than patients with less severe peripartum cardiomyopathy. The median income was lower in communities of individuals with severe peripartum cardiomyopathy than in communities of individuals with less severe peripartum cardiomyopathy.
Conclusion: Patients with severe peripartum cardiomyopathy outcomes were more likely to live in communities with greater social vulnerability than patients with less severe peripartum cardiomyopathy outcomes. To reduce disparities and maternal mortality rates, resources may need to be directed to socially vulnerable communities.
Keywords: cardiomyopathies; disparity; geographic disparities; health equity; inequity; maternal morbidity; maternal mortality; peripartum cardiomyopathy; postpartum period; racial disparities; social determinants of health; social factors; social vulnerability.
Copyright © 2022 Elsevier Inc. All rights reserved.
Conflict of interest statement
The authors report no conflict of interest.
Figures
References
-
- Cunningham FG, Byrne JJ, Nelson DB. Peripartum cardiomyopathy. Obstet Gynecol 2019;133:167–79. - PubMed
-
- Pearson GD, Veille JC, Rahimtoola S, et al. Peripartum cardiomyopathy: National Heart, Lung, and Blood Institute and Office of Rare Diseases (National Institutes of Health) workshop recommendations and review. JAMA 2000;283:1183–8. - PubMed
-
- Whitehead SJ, Berg CJ, Chang J. Pregnancy-related mortality due to cardiomyopathy: United States, 1991–1997. Obstet Gynecol 2003;102:1326–31. - PubMed
MeSH terms
Grants and funding
LinkOut - more resources
Full Text Sources
Medical
Miscellaneous