The burden and predictors of venous thromboembolic diseases in patients with multiple primary malignancies
- PMID: 36314077
- PMCID: PMC10026306
- DOI: 10.1002/cnr2.1742
The burden and predictors of venous thromboembolic diseases in patients with multiple primary malignancies
Abstract
Background: Venous thromboembolism (VTE) represents a considerable burden on cancer patients' survival and quality of life, but this burden varies based on the patient's baseline characteristics and cancer-related factors. Although solid evidence on the predictors and effect of VTE in cancer patients exists.
Aim: To evaluate VTE rate, morbidity, and mortality to develop parameters that could predict VTEs and their associated mortality in patients with multiple primary malignancies (MPMs).
Method and results: This was a retrospective cohort study that took place at King Abdulaziz Medical City, Riyadh, Kingdom of Saudi Arabia. Two hundred and forty-two patients with at least two biopsy-proven malignancies and had at least 3 months of follow-up after MPMs diagnosis were included. VTE was diagnosed in 14.5% of the cases, two-thirds of which were deep vein thrombosis. VTE was significantly associated with a higher mortality and worse survival. Predictors of VTE after MPMs diagnosis were a high ECOG performance status at MPMs diagnosis, a metastatic first primary malignancy, and ICU admission after MPMs diagnosis. Having a GI or hematological malignancy as the second primary malignancy, a high D-dimer at ICU admission, and palliative care referral were significantly associated with a higher mortality in patients who had VTE.
Conclusion: VTE was diagnosed in 14.5% of patients with MPMs and it significantly compromises their survival. We believe that these results might be of particular benefit since the phenomenon of MPMs is becoming more frequently encountered.
Keywords: cancer-associated thrombosis; multiple primaries; multiple primary malignancies; thromboprophylaxis; venous thromboembolism.
© 2022 The Authors. Cancer Reports published by Wiley Periodicals LLC.
Conflict of interest statement
The authors have stated explicitly that there are no conflicts of interest in connection with this article.
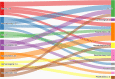
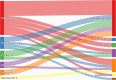
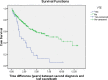
Figures


Similar articles
-
Venous thromboembolism as the first sign of malignancy.J Vasc Surg Venous Lymphat Disord. 2022 Nov;10(6):1260-1266. doi: 10.1016/j.jvsv.2022.05.014. Epub 2022 Jul 22. J Vasc Surg Venous Lymphat Disord. 2022. PMID: 35872141
-
Incidence and Clinical Characteristic of Venous Thromboembolism in Gynecologic Oncology Patients attending King Chulalongkorn Memorial Hospital over a 10 Year Period.Asian Pac J Cancer Prev. 2015;16(15):6705-9. doi: 10.7314/apjcp.2015.16.15.6705. Asian Pac J Cancer Prev. 2015. PMID: 26434898
-
Venous thromboembolism after severe trauma: incidence, risk factors and outcome.Injury. 2010 Jan;41(1):97-101. doi: 10.1016/j.injury.2009.06.010. Injury. 2010. PMID: 19608183
-
[Clinical features of patients with venous thromboembolism: 177 case analysis in 10 years].Zhonghua Wei Zhong Bing Ji Jiu Yi Xue. 2019 Apr;31(4):453-457. doi: 10.3760/cma.j.issn.2095-4352.2019.04.016. Zhonghua Wei Zhong Bing Ji Jiu Yi Xue. 2019. PMID: 31109420 Review. Chinese.
-
A narrative review on the epidemiology, prevention, and treatment of venous thromboembolic events in the context of chronic venous disease.J Vasc Surg Venous Lymphat Disord. 2021 Nov;9(6):1557-1567. doi: 10.1016/j.jvsv.2021.03.018. Epub 2021 Apr 16. J Vasc Surg Venous Lymphat Disord. 2021. PMID: 33866055 Review.
Cited by
-
Cardiac Morbidity and Mortality in Patients with Sarcoma: A Population-Based Study.Clin Med Insights Oncol. 2024 Mar 28;18:11795549241237703. doi: 10.1177/11795549241237703. eCollection 2024. Clin Med Insights Oncol. 2024. PMID: 38558879 Free PMC article.
-
Blood hypercoagulability and thrombosis mechanisms in cancer patients -A brief review.Heliyon. 2024 Oct 1;10(19):e38831. doi: 10.1016/j.heliyon.2024.e38831. eCollection 2024 Oct 15. Heliyon. 2024. PMID: 39435109 Free PMC article. Review.
References
MeSH terms
LinkOut - more resources
Full Text Sources
Medical

