Right atrial structural remodeling predict worse outcomes in transcatheter mitral valve repair
- PMID: 36321593
- PMCID: PMC10092558
- DOI: 10.1002/ccd.30471
Right atrial structural remodeling predict worse outcomes in transcatheter mitral valve repair
Abstract
Background: In the current study, we assess the predictive role of right and left atrial volume indices (RAVI and LAVI) as well as the ratio of RAVI/LAVI (RLR) on mortality following transcatheter mitral valve repair (TMVr).
Methods: Transthoracic echocardiograms of 158 patients who underwent TMVr at a single academic medical center from 2011 to 2018 were reviewed retrospectively. RAVI and LAVI were calculated using Simpson's method. Patients were stratified based on etiology of mitral regurgitation (MR). Cox proportional-hazard regression was created utilizing MR type, STS-score, and RLR to assess the independent association of RLR with survival. Kaplan-Meier analysis was used to analyze the association between RAVI and LAVI with all-cause mortality. Hemodynamic values from preprocedural right heart catheterization were also compared between RLR groups.
Results: Among 123 patients included (median age 81.3 years; 52.5% female) there were 50 deaths during median follow-up of 3.0 years. Patients with a high RAVI and low LAVI had significantly higher all-cause mortality while patients with high LAVI and low RAVI had significantly improved all-cause mortality compared to other groups (p = 0.0032). RLR was significantly associated with mortality in patients with both functional and degenerative MR (p = 0.0038). Finally, Cox proportion-hazard modeling demonstrated that an elevated RLR above the median value was an independent predictor of all-cause mortality [HR = 2.304; 95% CI = 1.26-4.21, p = 0.006] when MR type and STS score were accounted for.
Conclusion: Patients with a high RAVI and low LAVI had significantly increased mortality than other groups following TMVr suggesting RA remodeling may predict worse outcomes following the procedure. Concordantly, RLR was predictive of mortality independent of MR type and preprocedural STS-score. These indices may provide additional risk stratification in patients undergoing evaluation for TMVr.
Keywords: Cardiac Remodeling; Echocardiography; LAVI; Mitraclip; Mitral Regurgitation; RAVI; RAVI/LAVI Ratio; Transcatheter Mitral Valve Repair.
© 2022 The Authors. Catheterization and Cardiovascular Interventions published by Wiley Periodicals LLC.
Conflict of interest statement
The authors declare no conflict of interest.
Figures
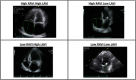


Comment in
-
Telltale atria-The meaning of adverse remodeling.Catheter Cardiovasc Interv. 2023 Jan;101(1):225-226. doi: 10.1002/ccd.30555. Catheter Cardiovasc Interv. 2023. PMID: 36655562 No abstract available.
References
MeSH terms
LinkOut - more resources
Full Text Sources
Medical

