A Pilot Study of High-Definition Transcranial Direct Current Stimulation in Refractory Status Epilepticus: The SURESTEP Trial
- PMID: 36323975
- PMCID: PMC9629761
- DOI: 10.1007/s13311-022-01317-5
A Pilot Study of High-Definition Transcranial Direct Current Stimulation in Refractory Status Epilepticus: The SURESTEP Trial
Abstract
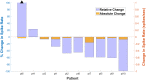
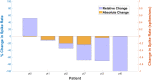
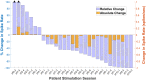
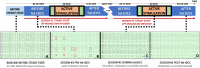
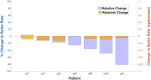
Refractory status epilepticus (RSE) is a life-threatening emergency with high mortality and poor functional outcomes in survivors. Treatment is typically limited to intravenous anesthetic infusions and multiple anti-seizure medications. While ongoing seizures can cause permanent neurological damage, medical therapies also pose severe and life-threatening side effects. We tested the feasibility of using high-definition transcranial direct current stimulation (hd-tDCS) in the treatment of RSE. We conducted 20-min hd-tDCS sessions at an outward field orientation, intensity of 2-mA, 4 + 1 channels, and customized for deployment over the electrographic maximum of epileptiform activity ("spikes") determined by real-time clinical EEG monitoring. There were no adverse events from 32 hd-tDCS sessions in 10 RSE patients. Over steady dosing states of infusions and medications in 29 included sessions, median spike rates/patient fell by 50% during hd-tDCS on both automated (p = 0.0069) and human (p = 0.0277) spike counting. Median spike rates for any given stimulation session also fell by 50% during hd-tDCS on automated spike counting (p = 0.0032). Immediately after hd-tDCS, median spike rates/patient remained down by 25% on human spike counting (p = 0.018). Compared to historical controls, hd-tDCS subjects were successfully discharged from the intensive care unit (ICU) 45.8% more often (p = 0.004). When controls were selected using propensity score matching, the discharge rate advantage improved to 55% (p = 0.002). Customized EEG electrode targeting of hd-tDCS is a safe and non-invasive method of hyperacutely reducing epileptiform activity in RSE. Compared to historical controls, there was evidence of a cumulative chronic clinical response with more hd-tDCS subjects discharged from ICU.
© 2022. The American Society for Experimental Neurotherapeutics, Inc.
Figures


Similar articles
-
High-definition transcranial direct current stimulation desynchronizes refractory status epilepticus.Neurotherapeutics. 2024 Jul;21(4):e00343. doi: 10.1016/j.neurot.2024.e00343. Epub 2024 Apr 4. Neurotherapeutics. 2024. PMID: 38580510 Free PMC article.
-
Transcranial direct current stimulation for focal status epilepticus or lateralized periodic discharges in four patients in a critical care setting.Epilepsia. 2023 Apr;64(4):875-887. doi: 10.1111/epi.17514. Epub 2023 Feb 7. Epilepsia. 2023. PMID: 36661376
-
Extended Multiple-Field High-Definition transcranial direct current stimulation (HD-tDCS) is well tolerated and safe in healthy adults.Restor Neurol Neurosci. 2017;35(6):631-642. doi: 10.3233/RNN-170757. Restor Neurol Neurosci. 2017. PMID: 29172010 Free PMC article.
-
More focal, less heterogeneous? Multi-level meta-analysis of cathodal high-definition transcranial direct current stimulation effects on language and cognition.J Neural Transm (Vienna). 2022 Jul;129(7):861-878. doi: 10.1007/s00702-022-02507-3. Epub 2022 May 18. J Neural Transm (Vienna). 2022. PMID: 35585206 Free PMC article. Review.
-
Dietary, immunological, surgical, and other emerging treatments for pediatric refractory status epilepticus.Seizure. 2019 May;68:89-96. doi: 10.1016/j.seizure.2018.09.002. Epub 2018 Sep 14. Seizure. 2019. PMID: 30245007 Review.
Cited by
-
Noninvasive Brain Stimulation as Focal Epilepsy Treatment in the Hospital, Clinic, and Home.medRxiv [Preprint]. 2025 Feb 5:2025.02.03.25321406. doi: 10.1101/2025.02.03.25321406. medRxiv. 2025. Update in: Epilepsia Open. 2025 Jun;10(3):787-795. doi: 10.1002/epi4.70033. PMID: 39974017 Free PMC article. Updated. Preprint.
-
A New Non-invasive Neuromodulation Technique for Super Refractory Status Epilepticus: Can We Consider tDCS for This Devastating Condition?Neurotherapeutics. 2023 Jan;20(1):179-180. doi: 10.1007/s13311-022-01329-1. Epub 2022 Dec 9. Neurotherapeutics. 2023. PMID: 36484907 Free PMC article. No abstract available.
-
Dreams interrupted: characteristics of REM sleep-associated seizures and status epilepticus.J Clin Sleep Med. 2025 Jan 1;21(1):23-32. doi: 10.5664/jcsm.11336. J Clin Sleep Med. 2025. PMID: 39167425
-
Noninvasive brain stimulation as focal epilepsy treatment in the hospital, clinic, and home.Epilepsia Open. 2025 Jun;10(3):787-795. doi: 10.1002/epi4.70033. Epub 2025 Apr 10. Epilepsia Open. 2025. PMID: 40208019 Free PMC article.
-
Efficacy and safety of transcranial direct current stimulation (tDCS) in treatment of refractory epilepsy: an updated systematic review and meta-analysis of randomized sham-controlled trials.Neurol Sci. 2025 Feb;46(2):671-687. doi: 10.1007/s10072-024-07866-1. Epub 2024 Nov 13. Neurol Sci. 2025. PMID: 39532798 Free PMC article.
References
Publication types
MeSH terms
Grants and funding
LinkOut - more resources
Full Text Sources
Medical

