Surface electromyography study on asymmetry in paravertebral muscle degeneration in patients with degenerative lumbar scoliosis
- PMID: 36333417
- PMCID: PMC9636411
- DOI: 10.1038/s41598-022-23541-x
Surface electromyography study on asymmetry in paravertebral muscle degeneration in patients with degenerative lumbar scoliosis
Abstract
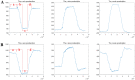
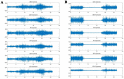
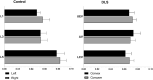
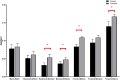
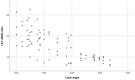
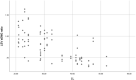
The asymmetry of paravertebral muscle (PVM) degeneration in degenerative lumbar scoliosis (DLS) patients has been extensively studied by imaging and histological examination and has not yet been verified by surface electromyography (sEMG) techniques. To study the relationship between the surface electromyography (sEMG) and degenerative characteristics of paravertebral muscles (PVMs) in patients with degenerative lumbar scoliosis (DLS). In twenty DLS patients and fifteen healthy subjects, sEMG activity of the PVMs at the level of the upper end vertebra (UEV), apical vertebra (AV) and lower end vertebra (LEV) was measured during static standing and dynamic standing forward flexion and backward extension tasks. Action segmentation was achieved according to inertial measurement unit (IMU) data. The sEMG characteristics of the PVMs on the convex and concave sides were compared, and the relationship of these data with the Cobb angle and lumbar lordotic angle (LL) was analyzed. In the DLS group, there was no difference in sEMG activity between the convex and concave sides at the UEV or AV level, but in the motion and return phases of the standing forward flexion task (P = 0.000, P = 0.015) and the maintenance and return phases of the standing backward extension task (P = 0.001, P = 0.01), there was a significant difference in sEMG activity between the convex and concave sides at the LEV level. Asymmetrical sEMG activity at the LEV level was negatively correlated with the Cobb angle (F = 93.791, P < 0.001) and LL angle (F = 65.564, P < 0.001). In the DLS group, asymmetrical sEMG activity of the PVMs appeared at the LEV level, with the concave side being more active than the convex side. This sEMG characteristics were consistent with their imaging and histological degenerative features and correlated with bone structural parameters.
© 2022. The Author(s).
Conflict of interest statement
The authors declare no competing interests.
Figures





Similar articles
-
Degenerative characteristics of multifidus at different vertebral levels of scoliosis in patients with degenerative lumbar scoliosis and relationship of these degenerative characteristics with surface electromyography activity.BMC Musculoskelet Disord. 2022 Dec 8;23(1):1074. doi: 10.1186/s12891-022-06038-6. BMC Musculoskelet Disord. 2022. PMID: 36476222 Free PMC article.
-
Quantitative analysis of paravertebral muscle asymmetry and its correlation with spinal deformity in patients with degenerative lumbar scoliosis: a retrospective case-control study.Quant Imaging Med Surg. 2024 May 1;14(5):3593-3605. doi: 10.21037/qims-23-1668. Epub 2024 Apr 18. Quant Imaging Med Surg. 2024. PMID: 38720864 Free PMC article.
-
[Radiological comparison of bilateral paravertebral muscles in degenerative lumbar scoliosis and its potential importance].Zhonghua Wai Ke Za Zhi. 2012 Nov;50(11):975-80. Zhonghua Wai Ke Za Zhi. 2012. PMID: 23302479 Chinese.
-
Correlation between multifidus muscle atrophy, spinopelvic parameters, and severity of deformity in patients with adult degenerative scoliosis: the parallelogram effect of LMA on the diagonal through the apical vertebra.J Orthop Surg Res. 2019 Aug 28;14(1):276. doi: 10.1186/s13018-019-1323-6. J Orthop Surg Res. 2019. PMID: 31455401 Free PMC article.
-
Asymmetric degeneration of paravertebral muscles in patients with degenerative lumbar scoliosis.Spine (Phila Pa 1976). 2012 Jul 15;37(16):1398-406. doi: 10.1097/BRS.0b013e31824c767e. Spine (Phila Pa 1976). 2012. PMID: 22322373
Cited by
-
Comparing Electromyographic Muscle Activities and Kinematics During Sit-to-Stand Transitions in Patients with Adult Spinal Deformity Versus Healthy Controls.J Clin Med. 2025 Apr 7;14(7):2514. doi: 10.3390/jcm14072514. J Clin Med. 2025. PMID: 40217963 Free PMC article.
-
Extent of fatty infiltration in lumbar paraspinal muscles in adults with degenerative scoliosis: segmental differences in muscle involvement.Eur Spine J. 2025 Jul 21. doi: 10.1007/s00586-025-09165-5. Online ahead of print. Eur Spine J. 2025. PMID: 40689985
-
Answer to the Letter to the Editor of M. Hamza, et al. concerning "Association between lumbar paraspinal muscle activities and quality in chronic low back pain: a cross-sectional analysis" by Zhang T, Firouzabadi A, Becker L, et al. (Eur Spine J [2025]: doi: 10.1007/s00586-025-08727-x).Eur Spine J. 2025 Jun;34(6):2498-2501. doi: 10.1007/s00586-025-08845-6. Epub 2025 Apr 29. Eur Spine J. 2025. PMID: 40301149 No abstract available.
-
Correlation analysis between multifidus muscle atrophy and the severity of degenerative scoliosis retrospective, cross-sectional study.Sci Rep. 2025 Aug 17;15(1):30133. doi: 10.1038/s41598-025-15622-4. Sci Rep. 2025. PMID: 40820023 Free PMC article.
References
Publication types
MeSH terms
Grants and funding
LinkOut - more resources
Full Text Sources
Medical

