Association between Migraines and Prior Proton Pump Inhibitor Use: A Nested Case-Control Study Using a National Health Screening Cohort
- PMID: 36355557
- PMCID: PMC9694889
- DOI: 10.3390/ph15111385
Association between Migraines and Prior Proton Pump Inhibitor Use: A Nested Case-Control Study Using a National Health Screening Cohort
Abstract
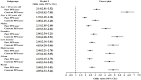
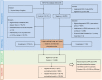
The effect of proton pump inhibitor (PPI) use on migraine risk remains controversial. We explored the odds of migraines in relation to prior PPI use and treatment duration. Data from the Korean National Health Insurance Service-Health Screening Cohort (2002−2015) were analyzed in this nested case-control study involving 28,159 participants with incident migraines and 112,636 controls (1:4 matched by sex, age, income, and residential region). The baseline covariates were balanced by performing propensity score overlap weighting-based adjustments, and the effect of prior PPI use (past vs. current) and treatment duration (<30 and 30−365 days vs. ≥365 days) on incident migraines was evaluated using logistic regression. In past and current PPI users, prior PPI use raised the likelihood of migraines (adjusted odds ratio [95% confidence interval]: 2.56 [2.36−2.79] and 4.66 [4.29−5.06], respectively). Participants who used PPI for <30, 30−365, or ≥365 days exhibited high odds of migraines (2.49 [2.29−2.72], 4.41 [4.05−4.79], and 4.14 [3.77−4.54], respectively). Incident migraines with or without aura also increased independently of PPI use history or duration. In summary, prior PPI use, irrespective of the elapsed time since use and the duration of use, is possibly associated with incident migraines with or without aura.
Keywords: aura; migraine; nested case-control study; proton pump inhibitors.
Conflict of interest statement
The authors declare no conflict of interest.
Figures

References
-
- Disease G.B.D., Injury I., Prevalence C. Global, regional, and national incidence, prevalence, and years lived with disability for 328 diseases and injuries for 195 countries, 1990–2016: A systematic analysis for the Global Burden of Disease Study 2016. Lancet. 2017;390:1211–1259. doi: 10.1016/S0140-6736(17)32154-2. - DOI - PMC - PubMed
-
- Silberstein S.D., Dodick D., Freitag F., Pearlman S.H., Hahn S.R., Scher A.I., Lipton R.B. Pharmacological approaches to managing migraine and associated comorbidities--clinical considerations for monotherapy versus polytherapy. Headache. 2007;47:585–599. doi: 10.1111/j.1526-4610.2007.00760.x. - DOI - PubMed
Grants and funding
LinkOut - more resources
Full Text Sources
Miscellaneous

