Pressure-flow responses to exercise in aortic stenosis, mitral regurgitation and diastolic dysfunction
- PMID: 36356959
- PMCID: PMC9664118
- DOI: 10.1136/heartjnl-2022-321204
Pressure-flow responses to exercise in aortic stenosis, mitral regurgitation and diastolic dysfunction
Abstract
Background: Haemodynamic exercise testing is important for evaluating patients with dyspnoea on exertion and preserved ejection fraction. Despite very different pathologies, patients with pressure (aortic stenosis (AS)) and volume (mitral regurgitation (MR)) overload and diastolic dysfunction after recent acute myocardial infarction (AMI) reach similar filling pressure levels with exercise. The pressure-flow relationships (the association between change in cardiac output (∆CO) and change in pulmonary arterial wedge pressure (∆PAWP) may provide insight into haemodynamic adaptation to exercise in these groups.
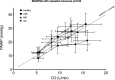
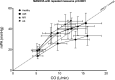
Methods and results: One hundred sixty-eight subjects aged >50 years with a left ventricular ejection fraction of ≥50% underwent invasive exercise testing. They were enrolled in four different studies: AS (40 patients), AMI (52 patients), MR (43 patients) and 33 healthy subjects. Haemodynamic data were measured at rest, at 25 W, 75 W and at peak exercise. In all groups, PAWP increased with exercise. The greatest increase was observed in patients with AMI (from 12.7±3.9 mm Hg to 33.1±8.2 mm Hg, p<0.0001) and patients with AS (from 11.8±3.9 mm Hg to 31.4±6.1 mm Hg, p<0.0001), and the smallest was observed in healthy subjects (from 8.3±2.4 mm Hg to 21.1±7.5 mm Hg, p<0.0001). In all groups, the relative pressure increase was greatest at the beginning of the exercise. CO increased most in healthy patients (from 5.3±1.1 to 16.0±3.0 L/min, p<0.0001) and least in patients with AS (from 5.3±1.2 L/min to 12.4±2.6 L/min, p<0.0001). The pressure-flow relationships (∆PAWP/∆CO) and differed among groups (p=0.02). In all groups, the pressure-flow relationship was steepest in the initial phase of the exercise test. The AMI and AS groups (2.3±1.2 mm Hg/L/min and 3.0±1.3 mm Hg/L/min, AMI and AS, respectively) had the largest overall pressure-flow relationship; the healthy group had the smallest initially and at peak exercise (1.3±1.1 mm Hg/L/min) followed by MR group (1.9±1.4 mm Hg/L/min).
Conclusion: The pressure-flow relationship was steepest in the initial phase of the exercise test in all groups. The pressure-flow relationship differs between groups.
Trial registration numbers: NCT01974557, NCT01046838, NCT02961647 and NCT02395107.
Keywords: Aortic stenosis; Heart Failure, Diastolic; Mitral regurgitation; Myocardial Infarction.
© Author(s) (or their employer(s)) 2022. Re-use permitted under CC BY-NC. No commercial re-use. See rights and permissions. Published by BMJ.
Conflict of interest statement
Competing interests: None declared.
Figures

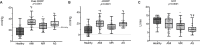
Comment in
-
Insights of pressure-flow relationship during exercise in cardiovascular diseases.Heart. 2022 Nov 10;108(23):1841-1842. doi: 10.1136/heartjnl-2022-321524. Heart. 2022. PMID: 36356960 No abstract available.
Similar articles
-
Hemodynamic Characteristics in Significant Symptomatic and Asymptomatic Primary Mitral Valve Regurgitation at Rest and During Exercise.Circ Cardiovasc Imaging. 2018 Feb;11(2):e007171. doi: 10.1161/CIRCIMAGING.117.007171. Circ Cardiovasc Imaging. 2018. PMID: 29449412
-
Exercise testing in asymptomatic or minimally symptomatic aortic regurgitation: relationship of left ventricular ejection fraction to left ventricular filling pressure during exercise.Circulation. 1983 May;67(5):1091-100. doi: 10.1161/01.cir.67.5.1091. Circulation. 1983. PMID: 6299613
-
Doppler evaluations of left ventricular diastolic filling and pulmonary wedge pressure provide similar prognostic information in patients with systolic dysfunction after myocardial infarction.Am Heart J. 1995 Apr;129(4):716-25. doi: 10.1016/0002-8703(95)90321-6. Am Heart J. 1995. PMID: 7900623
-
Pulmonary Hypertension in Aortic Stenosis and Mitral Regurgitation: Rest and Exercise Echocardiography Significance.Prog Cardiovasc Dis. 2016 Jul-Aug;59(1):59-70. doi: 10.1016/j.pcad.2016.06.004. Epub 2016 Jul 4. Prog Cardiovasc Dis. 2016. PMID: 27389810 Review.
-
Pulmonary Arterial Wedge Pressure at Rest and During Exercise in Healthy Adults: A Systematic Review and Meta-analysis.J Card Fail. 2019 Feb;25(2):114-122. doi: 10.1016/j.cardfail.2018.10.009. Epub 2018 Oct 23. J Card Fail. 2019. PMID: 30366054
Cited by
-
Pulmonary vascular dysfunction in systemic sclerosis.JHLT Open. 2023 Nov 19;3:100024. doi: 10.1016/j.jhlto.2023.100024. eCollection 2024 Feb. JHLT Open. 2023. PMID: 40145114 Free PMC article.
References
Publication types
MeSH terms
Associated data
LinkOut - more resources
Full Text Sources
Medical
Research Materials
