Prognostic Impact of Positive Peritoneal Lavage Cytology on Resectable Pancreatic Body and Tail Cancer: A Retrospective Study
- PMID: 36357802
- PMCID: PMC9895002
- DOI: 10.1007/s00268-022-06818-0
Prognostic Impact of Positive Peritoneal Lavage Cytology on Resectable Pancreatic Body and Tail Cancer: A Retrospective Study
Abstract
Background: The prognostic impact of positive peritoneal lavage cytology on pancreatic cancer is unclear. Therefore, this study aimed to evaluate its impact in resectable pancreatic body and tail cancer.
Methods: Between January 2006 and December 2019, 97 patients with pancreatic body and tail cancer underwent peritoneal lavage cytology and curative resection at our institution. We analyzed the impact of positive peritoneal lavage cytology on clinicopathological factors and on the prognosis of pancreatic body and tail cancer.
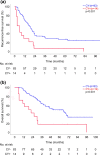
Results: Malignant cells were detected in 14 patients (14.4%) using peritoneal lavage cytology. In these patients, the tumor diameter was significantly larger (p < 0.001) and anterior serosal invasion (p = 0.034), splenic artery invasion (p = 0.013), lympho-vessel invasion (p = 0.025), and perineural invasion (p = 0.008) were significantly more frequent. The R1 resection rate was also significantly higher in patients with positive peritoneal lavage cytology than in negative patients (p = 0.015). Positive peritoneal lavage cytology had a significantly poor impact on overall survival (p = 0.001) and recurrence-free survival (p < 0.001). This cytology was also an independent poor prognostic factor for recurrence (p = 0.022) and was associated with peritoneal dissemination and liver metastasis.
Conclusions: Positive peritoneal lavage cytology is considered to be indicative of more systemic disease in patients with resectable pancreatic body and tail cancer than in patients with negative peritoneal lavage cytology. Early detection of pancreatic cancer before it develops micrometastases is important to improve prognosis, and CY+ patients require more intensive multimodality treatment than standard treatment for resectable pancreatic cancer.
© 2022. The Author(s).
Conflict of interest statement
The authors declare that they have no conflict of interest.
Figures

Similar articles
-
Prognostic significance of intraoperative peritoneal washing cytology for patients with potentially resectable pancreatic ductal adenocarcinoma.Pancreatology. 2017 Jan-Feb;17(1):109-114. doi: 10.1016/j.pan.2016.11.001. Epub 2016 Nov 7. Pancreatology. 2017. PMID: 27840175
-
Prognostic importance of peritoneal washing cytology in patients with otherwise resectable pancreatic ductal adenocarcinoma who underwent pancreatectomy: A nationwide, cancer registry-based study from the Japan Pancreas Society.Surgery. 2019 Dec;166(6):997-1003. doi: 10.1016/j.surg.2019.06.023. Epub 2019 Aug 21. Surgery. 2019. PMID: 31445763
-
Impact of endoscopic ultrasound-guided fine needle aspiration on positive peritoneal lavage cytology in patients with resectable pancreatic body and tail cancer.J Hepatobiliary Pancreat Sci. 2024 Dec;31(12):897-905. doi: 10.1002/jhbp.12064. Epub 2024 Aug 8. J Hepatobiliary Pancreat Sci. 2024. PMID: 39117567
-
Should Positive Cytology Revealed by Intraoperative Lavage Preclude Radical Resection in Resectable Pancreatic Cancer?: A Systemic Review and Meta-analysis.Pancreas. 2022 Nov-Dec 01;51(10):1263-1276. doi: 10.1097/MPA.0000000000002163. Pancreas. 2022. PMID: 37099766
-
Incidence and prognostic significance of positive peritoneal lavage in colorectal cancer.Surg Today. 2015 Sep;45(9):1073-81. doi: 10.1007/s00595-014-1066-2. Epub 2014 Nov 7. Surg Today. 2015. PMID: 25373362 Review.
References
MeSH terms
LinkOut - more resources
Full Text Sources
Medical

