Structural and Socio-Spatial Determinants Influencing Care and Survival of Patients with a Pancreatic Adenocarcinoma: Results of the PANDAURA Cohort
- PMID: 36358831
- PMCID: PMC9658615
- DOI: 10.3390/cancers14215413
Structural and Socio-Spatial Determinants Influencing Care and Survival of Patients with a Pancreatic Adenocarcinoma: Results of the PANDAURA Cohort
Abstract
Background and aims: Pancreatic cancer is highly lethal and often diagnosed at an advanced stage. This cohort study analyzes the impact of care pathways, delays, and socio-spatial determinants on pancreatic cancer patients’ diagnosis, treatment, and prognosis. Method: Patients with pancreatic adenocarcinoma newly diagnosed at all stages between January and June 2016 in the AuRA French region were included. The influence on survival of delays of care, healthcare centers’ expertise, and socio-spatial determinants was evaluated. Results: Here, 538 patients were included in 76 centers including 116 patients (21.8%) with resectable, 64 (12.0%) borderline-resectable, 147 (27.6%) locally-advanced tumors, and 205 (38.5%) with metastatic disease. A delay between first symptoms and CT scans did not statistically influence overall survival (OS). In resected patients, OS was significantly higher in centers with more than 20 surgeries (HR<5 surgeries/year = 2.236 and HR5-20 surgeries/year = 1.215 versus centers with > 20 surgeries/year p = 0.0081). Regarding socio-spatial determinants, patients living in municipalities with greater access to a general practitioner (HR = 1.673, p = 0.0153) or with a population density below 795.1 people/km2 (HR = 1.881, p = 0.0057) were significantly more often resectable. Conclusion: This cohort study supports the pivotal role of general practitioner in cancer care and the importance of the centralization of pancreatic surgery to optimize pancreatic cancer patients’ care and outcomes. However, delays of care did not impact patient survival.
Keywords: care delays; general practitioner; localized potential accessibility; pancreatic adenocarcinoma; pancreatic surgery; socio-spatial disparities.
Conflict of interest statement
The authors declare no conflict of interest.
Figures
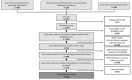
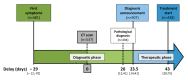
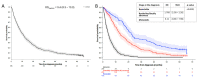
References
LinkOut - more resources
Full Text Sources
Miscellaneous

