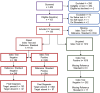
Diagnostic accuracy for self-reported methamphetamine use versus oral fluid test as the reference standard in a methamphetamine-dependent intervention trial population
- PMID: 36367075
- PMCID: PMC10952224
- DOI: 10.1111/add.16085
Diagnostic accuracy for self-reported methamphetamine use versus oral fluid test as the reference standard in a methamphetamine-dependent intervention trial population
Abstract
Aims: Treatment of methamphetamine dependence requires monitoring of recent use or abstinence. Self-report is commonly used for routine monitoring, but the accuracy of self-report is not established. For the treating clinician, the key accuracy statistic is the negative predictive value (NPV). The study aim was to estimate the NPV of self-reported non-use of methamphetamine compared with an oral fluid reference standard.
Design, setting and participants: This study was a secondary (subgroup) analysis from a randomized controlled pharmacotherapy trial. Three Australian outpatient addiction services took part. Particpants were 139 people dependent on methamphetamine.
Measurements: Weekly oral fluid samples over 12 weeks to determine methamphetamine (and amphetamine) concentrations were used as the reference standard. Self-report of any methamphetamine use in the previous 7 days by the time-line follow-back method was the index test. Standard diagnostic accuracy statistics were calculated for all available paired episodes (n = 1134). Three NPV values were calculated: unadjusted NPV and NPV adjusted for clustering of observations through logistic regression and generalized estimating equation (GEE). We also calculated the NPVs for a range of prevalence rates of methamphetamine use, for the calculated levels of sensitivity and specificity.
Findings: Sensitivity was 96.4% [95% confidence interval (CI) = 95-97.5], specificity was 63.7% (95% CI = 57.3-69.8) and positive predictive value (PPV) was 90.8% (95% CI = 88.8-92.6). The unadjusted NPV was 82.7% (95% CI = 76.5-87.9), adjusted NPV by logistic regression 82.7% (95% CI = 73.9-91.5) and GEE 76.8% (95% CI = 66.8-86.8). At a methamphetamine use prevalence of 5%, the estimated NPV would be 99.7% (95% CI = 99.6-99.9) and at 95% prevalence, 48.2% (95% CI = 39.6-57.0).
Conclusions: Self-report of no recent methamphetamine use appears to be sufficiently accurate to be clinically useful at the expected prevalence rates of methamphetamine use in clinical treatment settings. If generalizable to clinical settings, where these tests are routinely conducted, this may permit a reduction in the frequency and cost of oral fluid assays.
Keywords: Addiction; clinical trial; diagnostic accuracy; methamphetamine; oral fluid; psychiatry; saliva; self-report; substance use disorders.
© 2022 The Authors. Addiction published by John Wiley & Sons Ltd on behalf of Society for the Study of Addiction.
Conflict of interest statement
G.C. has received educational and travel support from Servier, Astra Zeneca, Otsuka Australia, Merck Sharp & Dohme and Janssen‐Cilag in the past 5 years. O.D. has received grant support from the Brain and Behavior Foundation, Simons Autism Foundation, Stanley Medical Research Institute, Deakin University, Lilly, NHMRC and ASBDD/Servier. She has also received support in kind from BioMedica Nutraceuticals, NutritionCare and Bioceuticals. D.L. has provided consultancy advice to Lundbeck and Indivior and has received travel support and speaker honoraria from Camurus, Indivior, Janssen, Lundbeck, Servier and Shire. He has received research grants from Camurus and Seqirus. P.D. has received investigator‐initiated funding from Gilead Sciences, an untied educational grant from Indivior, and is an unpaid member of an Advisory Board for Mundipharma for work unrelated to this study. M.B. has received Grant/Research Support from the NIH, Cooperative Research Centre, Simons Autism Foundation, Cancer Council of Victoria, Stanley Medical Research Foundation, Medical Benefits Fund, National Health and Medical Research Council, Medical Research Futures Fund, Beyond Blue, Rotary Health, A2 milk company, Meat and Livestock Board, Woolworths, Avant and the Harry Windsor Foundation, has been a speaker for Abbot, Astra Zeneca, Janssen and Janssen, Lundbeck and Merck and served as a consultant to Allergan, Astra Zeneca, Bioadvantex, Bionomics, Collaborative Medicinal Development, Eisai, Janssen and Janssen, Lundbeck Merck, Pfizer and Servier. P.H. has received investigator‐initiated research funded by Gilead Sciences and Abbvie. S.A. has received speaker honoraria from Camurus, Gilead, Janssen and Servier.
Figures
Similar articles
-
Correlates of Validity of Self-Reported Methamphetamine Use among a Sample of Dependent Adults.Subst Use Misuse. 2018 Aug 24;53(10):1742-1755. doi: 10.1080/10826084.2018.1432649. Epub 2018 Feb 20. Subst Use Misuse. 2018. PMID: 29461134 Free PMC article. Clinical Trial.
-
Detection of illicit drugs in oral fluid from drivers as biomarker for drugs in blood.Forensic Sci Int. 2015 Nov;256:42-5. doi: 10.1016/j.forsciint.2015.06.027. Epub 2015 Jul 10. Forensic Sci Int. 2015. PMID: 26295911
-
Accuracy of hysterosalpingo-foam sonography in comparison to hysterosalpingo-contrast sonography with air/saline and to laparoscopy with dye.Hum Reprod. 2017 Apr 1;32(4):758-769. doi: 10.1093/humrep/dex013. Hum Reprod. 2017. PMID: 28184447
-
Polymerase chain reaction blood tests for the diagnosis of invasive aspergillosis in immunocompromised people.Cochrane Database Syst Rev. 2019 Sep 3;9(9):CD009551. doi: 10.1002/14651858.CD009551.pub4. Cochrane Database Syst Rev. 2019. PMID: 31478559 Free PMC article.
-
Non-contact tests for identifying people at risk of primary angle closure glaucoma.Cochrane Database Syst Rev. 2020 May 28;5(5):CD012947. doi: 10.1002/14651858.CD012947.pub2. Cochrane Database Syst Rev. 2020. PMID: 32468576 Free PMC article.
Cited by
-
Feasibility, Engagement, and Usability of a Remote, Smartphone-Based Contingency Management Program as a Treatment Add-On for Patients Who Use Methamphetamine: Single-Arm Pilot Study.JMIR Form Res. 2023 Jul 6;7:e47516. doi: 10.2196/47516. JMIR Form Res. 2023. PMID: 37410529 Free PMC article.
-
Lisdexamfetamine in the treatment of methamphetamine dependence: A randomised, placebo-controlled trial.Addiction. 2025 Jul;120(7):1345-1359. doi: 10.1111/add.16730. Epub 2024 Dec 19. Addiction. 2025. PMID: 39701142 Free PMC article. Clinical Trial.
-
How does a family history of psychosis influence the risk of methamphetamine-related psychotic symptoms: Evidence from longitudinal panel data.Addiction. 2023 Oct;118(10):1975-1983. doi: 10.1111/add.16230. Epub 2023 May 30. Addiction. 2023. PMID: 37157055 Free PMC article. Clinical Trial.
References
-
- Degenhardt L, Sara G, McKetin R, Roxburgh A, Dobbins T, Farrell M, et al. Crystalline methamphetamine use and methamphetamine‐related harms in Australia. Drug Alcohol Rev. 2017;36:160–70. - PubMed
-
- Bosanquet D, MacDougall HG, Rogers SJ, Starmer GA, McKetin R, Blaszczynski A, et al. Driving on ice: impaired driving skills in current methamphetamine users. Psychopharmacology. 2013;225:161–72. - PubMed
-
- Davey J, Armstrong K, Martin P. Results of the Queensland 2007–2012 roadside drug testing program: the prevalence of three illicit drugs. Accid Anal Prev. 2014;65:11–7. - PubMed
-
- Gjerde H, Langel K, Favretto D, Verstraete AG. Detection of illicit drugs in oral fluid from drivers as biomarker for drugs in blood. Forensic Sci Int. 2015;256:42–5. - PubMed
Publication types
MeSH terms
Substances
LinkOut - more resources
Full Text Sources
Medical