Effectiveness of a Health Coaching Intervention for Patient-Family Dyads to Improve Outcomes Among Adults With Diabetes: A Randomized Clinical Trial
- PMID: 36374502
- PMCID: PMC9664266
- DOI: 10.1001/jamanetworkopen.2022.37960
Effectiveness of a Health Coaching Intervention for Patient-Family Dyads to Improve Outcomes Among Adults With Diabetes: A Randomized Clinical Trial
Abstract
Importance: More than 75% of US adults with diabetes do not meet treatment goals. More effective support from family and friends ("supporters") may improve diabetes management and outcomes.
Objective: To determine if the Caring Others Increasing Engagement in Patient Aligned Care Teams (CO-IMPACT) intervention improves patient activation, diabetes management, and outcomes compared with standard care.
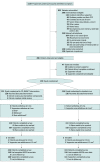
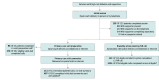
Design, setting, and participants: This randomized clinical trial was conducted from November 2016 to August 2019 among participants recruited from 2 Veterans Health Administration primary care sites. All patient participants were adults aged 30 to 70 years with diabetes who had hemoglobin A1c (HbA1c) levels greater than 8% of total hemoglobin (to convert to proportion of total hemoglobin, multiply by 0.01) or systolic blood pressure (SBP) higher than 150 mm Hg; each participating patient had an adult supporter. Of 1119 recruited, 239 patient-supporter dyads were enrolled between November 2016 and May 2018, randomized 1:1 to receive the CO-IMPACT intervention or standard care, and followed up for 12 to 15 months. Investigators and analysts were blinded to group assignment.
Interventions: Patient-supporter dyads received a health coaching session focused on dyadic information sharing and positive support techniques, then 12 months of biweekly automated monitoring telephone calls to prompt dyadic actions to meet diabetes goals, coaching calls to help dyads prepare for primary care visits, and after-visit summaries. Standard-care dyads received general diabetes education materials only.
Main outcomes and measures: Intent-to-treat analyses were conducted according to baseline dyad assignment. Primary prespecified outcomes were 12-month changes in Patient Activation Measure-13 (PAM-13) and UK Prospective Diabetes Study (UKPDS) 5-year diabetes-specific cardiac event risk scores. Secondary outcomes included 12-month changes in HbA1c levels, SBP, diabetes self-management behaviors, diabetes distress, diabetes management self-efficacy, and satisfaction with health system support for the involvement of family supporters. Changes in outcome measures between baseline and 12 months were analyzed using linear regression models.
Results: A total of 239 dyads enrolled; among patient participants, the mean (SD) age was 60 (8.9) years, and 231 (96.7%) were male. The mean (SD) baseline HbA1c level was 8.5% (1.6%) and SBP was 140.2 mm Hg (18.4 mm Hg). A total of 168 patients (70.3%) lived with their enrolled supporter; 229 patients (95.8%) had complete 12-month outcome data. In intention-to-treat analyses vs standard care, CO-IMPACT patients had greater 12-month improvements in PAM-13 scores (intervention effect, 2.60 points; 95% CI, 0.02-5.18 points; P = .048) but nonsignificant differences in UKPDS 5-year cardiac risk (intervention effect, 1.01 points; 95% CI, -0.74 to 2.77 points; P = .26). Patients in the CO-IMPACT arm also had greater 12-month improvements in healthy eating (intervention effect, 0.71 d/wk; 95% CI, 0.20-1.22 d/wk; P = .007), diabetes self-efficacy (intervention effect, 0.40 points; 95% CI, 0.09-0.71 points; P = .01), and satisfaction with health system support for the family supporter participants' involvement (intervention effect, 0.28 points; 95% CI, 0.07-0.49 points; P = .009); however, the 2 arms had similar improvements in HbA1c levels and in other measures.
Conclusions and relevance: In this randomized clinical trial, the CO-IMPACT intervention successfully engaged patient-supporter dyads and led to improved patient activation and self-efficacy. Physiological outcomes improved similarly in both arms. More intensive direct coaching of supporters, or targeting patients with less preexisting support or fewer diabetes management resources, may have greater impact.
Trial registration: ClinicalTrials.gov Identifier: NCT02328326.
Conflict of interest statement
Figures
Similar articles
-
Engaging family supporters of adult patients with diabetes to improve clinical and patient-centered outcomes: study protocol for a randomized controlled trial.Trials. 2018 Jul 24;19(1):394. doi: 10.1186/s13063-018-2785-2. Trials. 2018. PMID: 30041685 Free PMC article.
-
Effect of a Collaborative Care Model on Depressive Symptoms and Glycated Hemoglobin, Blood Pressure, and Serum Cholesterol Among Patients With Depression and Diabetes in India: The INDEPENDENT Randomized Clinical Trial.JAMA. 2020 Aug 18;324(7):651-662. doi: 10.1001/jama.2020.11747. JAMA. 2020. PMID: 32809002 Free PMC article. Clinical Trial.
-
Effect of a Peer Health Coaching Intervention on Clinical Outcomes Among US Veterans With Cardiovascular Risks: The Vet-COACH Randomized Clinical Trial.JAMA Netw Open. 2023 Jun 1;6(6):e2317046. doi: 10.1001/jamanetworkopen.2023.17046. JAMA Netw Open. 2023. PMID: 37278999 Free PMC article. Clinical Trial.
-
Comparing a Self-Management Program with and without Peer Support to Improve Quality of Life for Patients with COPD [Internet].Washington (DC): Patient-Centered Outcomes Research Institute (PCORI); 2021 Jun. Washington (DC): Patient-Centered Outcomes Research Institute (PCORI); 2021 Jun. PMID: 38593187 Free Books & Documents. Review.
-
Assessment of Interprofessional Collaborative Practices and Outcomes in Adults With Diabetes and Hypertension in Primary Care: A Systematic Review and Meta-analysis.JAMA Netw Open. 2021 Feb 1;4(2):e2036725. doi: 10.1001/jamanetworkopen.2020.36725. JAMA Netw Open. 2021. PMID: 33576817 Free PMC article.
Cited by
-
Impact of a resilience-building energy management intervention for people with systemic sclerosis: a mixed methods study.Rheumatol Adv Pract. 2024 Mar 8;8(2):rkae040. doi: 10.1093/rap/rkae040. eCollection 2024. Rheumatol Adv Pract. 2024. PMID: 38618141 Free PMC article.
-
Acceptability of an AI-enabled family module in a mobile app for enhanced diabetes management: Patient and family perspectives.Digit Health. 2025 Mar 25;11:20552076251322654. doi: 10.1177/20552076251322654. eCollection 2025 Jan-Dec. Digit Health. 2025. PMID: 40144049 Free PMC article.
-
5. Facilitating Positive Health Behaviors and Well-being to Improve Health Outcomes: Standards of Care in Diabetes-2025.Diabetes Care. 2025 Jan 1;48(1 Suppl 1):S86-S127. doi: 10.2337/dc25-S005. Diabetes Care. 2025. PMID: 39651983 Review.
-
2025 Clinical Practice Guidelines for Diabetes Management in Korea: Recommendation of the Korean Diabetes Association.Diabetes Metab J. 2025 Jul;49(4):582-783. doi: 10.4093/dmj.2025.0469. Epub 2025 Jul 1. Diabetes Metab J. 2025. PMID: 40631460 Free PMC article. No abstract available.
-
Use of Voice-Based Conversational Artificial Intelligence for Basal Insulin Prescription Management Among Patients With Type 2 Diabetes: A Randomized Clinical Trial.JAMA Netw Open. 2023 Dec 1;6(12):e2340232. doi: 10.1001/jamanetworkopen.2023.40232. JAMA Netw Open. 2023. PMID: 38039007 Free PMC article. Clinical Trial.
References
Publication types
MeSH terms
Substances
Associated data
Grants and funding
LinkOut - more resources
Full Text Sources
Medical
Miscellaneous

