Opioid-reduced anesthesia based on esketamine in gynecological day surgery: a randomized double-blind controlled study
- PMID: 36384481
- PMCID: PMC9667678
- DOI: 10.1186/s12871-022-01889-x
Opioid-reduced anesthesia based on esketamine in gynecological day surgery: a randomized double-blind controlled study
Abstract
Background: Opioid-reduced anesthesia may accelerate postoperative rehabilitation by reducing opioid-related side effects. The objective was to investigate the feasibility of opioid-reduced general anesthesia based on esketamine and to observe postoperative nausea and vomiting (PONV), postoperative pain, hemodynamics and other adverse reactions in gynecological day surgery compared with the traditional opioid-based anesthesia program.
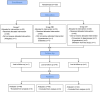
Method: This study was conducted as a prospective parallel-group randomized controlled trial. A total of 141 adult women undergoing gynecological day surgery were included. Patients were randomly assigned to receive traditional opioid-based anesthesia (Group C) with alfentanil, or opioid-reduced anesthesia (a moderate-opioid group (Group MO) and low-opioid group (Group LO) with esketamine and alfentanil). For anesthesia induction, the three groups received 20, 20, 10 μg/kg alfentanil respectively and Group LO received an additional 0.2 mg/kg esketamine. For maintenance of anesthesia, the patients in Group C received 40 μg/kg/h alfentanil, and those in Group MO and Group LO received 0.5 mg/kg/h esketamine.
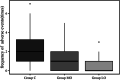
Results: Patients in the three groups had comparable clinical and surgical data. A total of 33.3% of patients in Group C, 18.4% of patients in Group MO and 43.2% of patients in Group LO met the primary endpoint (p = 0.033), and the incidence of nausea within 24 hours after surgery in Group MO was lower than in Group LO (p < 0.05). The extubation time, median length of stay in the hospital after surgery and visual analog scale (VAS) of postoperative pain were equivalent in the three groups. The frequencies of adverse hemodynamic events in the MO 1(0, 2) and LO 0(0, 1) groups were significantly decreased (p < 0.05). Compared with Group C, the median length of stay in the postanesthesia care unit (PACU) in Group LO was increased, 60.0 (36.25, 88.75) vs. 42.5 (25, 73.75) minutes (p < 0.05).
Conclusions: Opioid-reduced anesthesia based on esketamine is feasible and provides effective analgesia for patients. Esketamine provided a positive analgesic effect and the opioid-reduced groups showed more stable hemodynamics. However, less or no use of opioids did not result in a more comfortable prognosis.
Trial registration: This study was registered at Chictr.org.cn (NO. ChiCTR2100053153 ); November 13, 2021.
Keywords: Esketamine; Hemodynamics; Opioid-reduced anesthesia; PONV.
© 2022. The Author(s).
Conflict of interest statement
The authors declare that they have no competing interests.
Figures
References
Publication types
MeSH terms
Substances
Associated data
LinkOut - more resources
Full Text Sources
Miscellaneous