Time since primary transplant and poor functional status predict survival after redo lung transplant
- PMID: 36389317
- PMCID: PMC9641320
- DOI: 10.21037/jtd-22-334
Time since primary transplant and poor functional status predict survival after redo lung transplant
Abstract
Background: In previous studies, lower functional status measured by Karnofsky Performance Status (KPS) correlated with worse survival after redo lung transplant. We hypothesize that combining reduced functional status and time from primary lung transplant will correlate with the etiology of lung allograft failure after primary lung transplant and more accurately predict survival after redo lung transplant.
Methods: This retrospective study was approved by University of Minnesota Institutional Review Board. From the Scientific Registry of Transplant Recipients (SRTR) database, 739 patients underwent redo lung transplant (01/01/2005-8/30/2019). Pre-lung transplant characteristics, KPS, time between primary and redo lung transplant, outcomes, overall survival were evaluated. Paired comparisons were used to compare pre-transplant variables. A Cox regression model was fit to examine re-transplant survival. Due to non-proportional hazards, time between transplants was split into <1-year vs. 1+ years and analyzed with time-dependent coefficients, with follow-up time considered in three segments (0-6, 6-24, 24+ months).
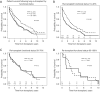
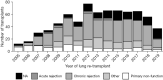
Results: After KPS grouping (10-40%, 50-70%, 80-100%), KPS 10-40% were less likely to be discharged after primary transplant and more likely required mechanical ventilation or extracorporeal membrane oxygenation (ECMO) bridging (P<0.001). Redo lung transplant survival was worse in the KPS 10-40% group who more likely underwent lung transplant <1 year after primary lung transplant. Mortality was significantly higher for patients who underwent redo lung transplant within one year of primary transplant when KPS was 10-40% (P<0.001). These patients were more likely to require redo lung transplant due to primary graft failure or acute cellular rejection.
Conclusions: Functional status and time from primary lung transplant are strong predictors of outcome after redo lung transplant. We categorized redo lung transplant recipients in two distinct groups. One group has early allograft failure and poor functional status with a very poor prognosis after redo lung transplant. The other group has chronic allograft failure and overall better functional status with relatively better survival after redo lung transplant. Salvage redo lung transplant for primary allograft failure or acute rejection is associated with low one year survival.
Keywords: Karnofsky Performance Status (KPS); Redo lung transplant; lung allocation score (LAS).
2022 Journal of Thoracic Disease. All rights reserved.
Conflict of interest statement
Conflicts of Interest: All authors have completed the ICMJE uniform disclosure form (available at https://jtd.amegroups.com/article/view/10.21037/jtd-22-334/coif). The authors have no conflicts of interest to declare.
Figures






Comment in
-
Time is ticking: the role of time after primary transplant and functional impairment on survival after redo lung transplant.J Thorac Dis. 2023 Apr 28;15(4):1523-1525. doi: 10.21037/jtd-22-1817. Epub 2023 Mar 14. J Thorac Dis. 2023. PMID: 37197525 Free PMC article. No abstract available.
References
-
- Ramsey SD, Patrick DL, Lewis S, et al. Improvement in quality of life after lung transplantation: a preliminary study. The University of Washington Medical Center Lung Transplant Study Group. J Heart Lung Transplant 1995;14:870-7. - PubMed
LinkOut - more resources
Full Text Sources
