Different effects of low muscle mass on the risk of non-alcoholic fatty liver disease and hepatic fibrosis in a prospective cohort
- PMID: 36403577
- PMCID: PMC9891951
- DOI: 10.1002/jcsm.13125
Different effects of low muscle mass on the risk of non-alcoholic fatty liver disease and hepatic fibrosis in a prospective cohort
Abstract
Background: Non-alcoholic fatty liver disease (NAFLD) and sarcopenia share insulin resistance as a common pathophysiology and have overlapping clinical manifestation of metabolic derangement; hence, it is difficult to differentiate the independent effect of sarcopenia on the development of NAFLD from concomitant metabolic disorders. Using a community-based prospective cohort study, the contributions of low muscle mass and genetic risk factors to the development of NAFLD and NAFLD-related hepatic fibrosis were investigated in the Korean population.
Methods: This prospective community-based cohort study included 40-70-year-old adults, followed up biennially from 2001-2002 to 2017-2018. NAFLD was defined as a hepatic steatosis index of ≥36, and hepatic fibrosis was defined based on the fibrosis-4 index. Sex-specific quartiles of body mass index (BMI)-adjusted muscle mass were calculated (muscle mass/BMI), and low muscle mass was defined as the lowest quartile (Q1). Cox proportional hazard models for incident NAFLD or hepatic fibrosis incorporating age, sex, BMI of ≥25 kg/m2 , metabolic syndrome and PNPLA3 and TM6SF2 risk alleles were used to assess the independent determinants for incident NAFLD and hepatic fibrosis among individuals with NAFLD at baseline.
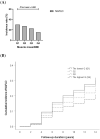
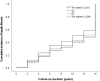
Results: Among the 4038 participants without NAFLD at baseline (mean age, 51.5 ± 8.8 years), 920 (22.8%) developed NAFLD during the 12-year follow-up period. As muscle mass decreased, the risk of NAFLD increased even after adjustment for age, sex, obesity, metabolic syndrome and PNPLA3 and TM6SF2 risk alleles [hazard ratio (HR) per quartile, 1.18, 95% confidence interval (CI), 1.11-1.27, P < 0.001]. TM6SF2 also affected the risk of NAFLD development [HR 1.19, (95% CI, 1.00-1.40), P = 0.044]. Of the 1176 patients with NAFLD but without hepatic fibrosis at baseline, the incident of hepatic fibrosis was found in 51.8%, 44.7%, 42.6% and 41.0% in Q1, Q2, Q3 and Q4 of BMI-adjusted muscle mass, respectively, during the follow-up period (P for trend = 0.006). However, this trend lost its statistical significance when adjusted for confounders. The PNPLA3 risk variant, but not the TM6SF2 genotype, was an independent risk factor for developing hepatic fibrosis among patients with NAFLD (HR 1.17, 95% CI 1.04-1.32, P = 0.010).
Conclusions: Both lower muscle mass index and genetic risk variants are important contributors to the development of NAFLD. In patients already diagnosed with NAFLD, however, PNPLA3 confers a greater risk for hepatic fibrosis progression than lower muscle mass.
Keywords: Liver fibrosis; Non-alcoholic fatty liver disease; PNPLA3; Sarcopenia; TM6SF2.
© 2022 The Authors. Journal of Cachexia, Sarcopenia and Muscle published by John Wiley & Sons Ltd on behalf of Society on Sarcopenia, Cachexia and Wasting Disorders.
Conflict of interest statement
The authors declare no conflict of interest.
Figures

References
-
- Cotter TG, Rinella M. Nonalcoholic fatty liver disease 2020: The state of the disease. Gastroenterology 2020;158:1851–1864. - PubMed
-
- Mantovani A, Csermely A, Petracca G, Beatrice G, Corey KE, Simon TG, et al. Non‐alcoholic fatty liver disease and risk of fatal and non‐fatal cardiovascular events: An updated systematic review and meta‐analysis. Lancet Gastroenterol Hepatol 2021;6:903–913. - PubMed
-
- Ekstedt M, Hagström H, Nasr P, Fredrikson M, Stål P, Kechagias S, et al. Fibrosis stage is the strongest predictor for disease‐specific mortality in NAFLD after up to 33 years of follow‐up. Hepatology 2015;61:1547–1554. - PubMed
-
- Koo BK, Kim D, Joo SK, Kim JH, Chang MS, Kim BG, et al. Sarcopenia is an independent risk factor for non‐alcoholic steatohepatitis and significant fibrosis. J Hepatol 2017;66:123–131. - PubMed
Publication types
MeSH terms
Substances
Grants and funding
LinkOut - more resources
Full Text Sources
Medical
Research Materials

