Approach to the Patient With Adrenal Hemorrhage
- PMID: 36404284
- PMCID: PMC9999363
- DOI: 10.1210/clinem/dgac672
Approach to the Patient With Adrenal Hemorrhage
Abstract
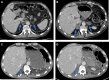
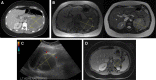
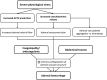
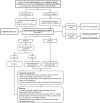
Adrenal hemorrhage is an uncommon, underrecognized condition that can be encountered in several clinical contexts. Diagnosing adrenal hemorrhage is challenging due to its nonspecific clinical features. Therefore, it remains a diagnosis that is made serendipitously on imaging of acutely unwell patients rather than with prospective clinical suspicion. Adrenal hemorrhage can follow abdominal trauma or appear on a background of predisposing conditions such as adrenal tumors, sepsis, or coagulopathy. Adrenal hemorrhage is also increasingly reported in patients with COVID-19 infection and in the context of vaccine-induced immune thrombocytopenia and thrombosis. Unexplained abdominal pain with hemodynamic instability in a patient with a predisposing condition should alert the physician to the possibility of adrenal hemorrhage. Bilateral adrenal hemorrhage can lead to adrenal insufficiency and potentially fatal adrenal crisis without timely recognition and treatment. In this article, we highlight the clinical circumstances that are associated with higher risk of adrenal hemorrhage, encouraging clinicians to prospectively consider the diagnosis, and we share a diagnostic and management strategy.
Keywords: COVID-19; adrenal apoplexy; adrenal crisis; adrenal incidentaloma; adrenal insufficiency; antiphospholipid syndrome.
© The Author(s) 2022. Published by Oxford University Press on behalf of the Endocrine Society.
Figures
Similar articles
-
Bilateral adrenal hemorrhage: learning notes from clinical practice and literature review.Front Endocrinol (Lausanne). 2023 Nov 3;14:1233710. doi: 10.3389/fendo.2023.1233710. eCollection 2023. Front Endocrinol (Lausanne). 2023. PMID: 38027193 Free PMC article. Review.
-
[Bilateral hemorrhagic necrosis of the adrenal glands in antiphospholipid syndrome: diagnostic pitfall and rare cause of acute abdominal pain syndrome].Gastroenterol Clin Biol. 1995 Jan;19(1):129-31. Gastroenterol Clin Biol. 1995. PMID: 7720976 French. No abstract available.
-
Primary adrenal insufficiency due to bilateral adrenal hemorrhage-adrenal infarction in a patient with systemic lupus erythematosus and antiphospholipid syndrome: case presentation and review of the literature.Hormones (Athens). 2023 Sep;22(3):521-531. doi: 10.1007/s42000-023-00463-5. Epub 2023 Jul 12. Hormones (Athens). 2023. PMID: 37436639 Free PMC article. Review.
-
Acute adrenal insufficiency due to bilateral adrenal hemorrhage in the context of antiphospholipid syndrome.Med Clin (Barc). 2023 Nov 10;161(9):413-414. doi: 10.1016/j.medcli.2023.06.020. Epub 2023 Jul 18. Med Clin (Barc). 2023. PMID: 37474397 English, Spanish. No abstract available.
-
Clinical characteristics of systemic lupus erythematosus patients with adrenal hemorrhage.Clin Rheumatol. 2024 Jul;43(7):2223-2227. doi: 10.1007/s10067-024-06938-z. Epub 2024 May 9. Clin Rheumatol. 2024. PMID: 38724818
Cited by
-
A 65-Year-Old Man with Bilateral Adrenal Hemorrhage Following Prophylaxis for Postoperative Deep Vein Thrombosis with Rivaroxaban.Am J Case Rep. 2023 Sep 2;24:e939816. doi: 10.12659/AJCR.939816. Am J Case Rep. 2023. PMID: 37658601 Free PMC article.
-
Unilateral Non-Hemorrhagic Adrenal Infarction in Pregnancy: Case Series and Literature Review.J Clin Med. 2023 Jul 24;12(14):4855. doi: 10.3390/jcm12144855. J Clin Med. 2023. PMID: 37510974 Free PMC article.
-
Bilateral adrenal hemorrhage in a postpartum woman with multiple thromboemboli: A case report.J Med Case Rep. 2024 Oct 25;18(1):518. doi: 10.1186/s13256-024-04834-3. J Med Case Rep. 2024. PMID: 39449152 Free PMC article.
-
Biochemically Negative Pheochromocytoma With Spontaneous Hemorrhage.AACE Endocrinol Diabetes. 2025 May 26;12(2):93-96. doi: 10.1016/j.aed.2025.05.004. eCollection 2025 Jul-Aug. AACE Endocrinol Diabetes. 2025. PMID: 40786995 Free PMC article.
-
Successful Conservative Treatment of Maternal Spontaneous Unilateral Adrenal Hemorrhage Causing Severe Anemia in the Third Trimester of Pregnancy-A Case Report.Medicina (Kaunas). 2024 Sep 4;60(9):1448. doi: 10.3390/medicina60091448. Medicina (Kaunas). 2024. PMID: 39336489 Free PMC article.
References
-
- Botteri A, Orell SR. Adrenal hemorrhage and necrosis in the adult. Acta Med Scand. 1964;175(4):409–419. - PubMed
-
- Xarli VP, Steele AA, Davis PJ, Buescher ES, Rios CN, Garcia-Bunuel R. Adrenal hemorrhage in the adult. Medicine (Baltimore). 1978;57(3):211–221. - PubMed
-
- Russell P. The adrenal glands in shock. Pathology. 1972;4(1):5–8. - PubMed
-
- Vella A, Nippoldt TB, Morris JC. Adrenal hemorrhage: a 25-year experience at the Mayo Clinic. Mayo Clin Proc. 2001;76(2):161–168. - PubMed
-
- Rao RH, Vagnucci AH, Amico JA. Bilateral massive adrenal hemorrhage: early recognition and treatment. Ann Intern Med. 1989;110(3):227–235. - PubMed
MeSH terms
LinkOut - more resources
Full Text Sources
Medical

