Transjugular intrahepatic portosystemic shunt vs conservative treatment for recurrent ascites: A propensity score matched comparison
- PMID: 36405105
- PMCID: PMC9669826
- DOI: 10.3748/wjg.v28.i41.5944
Transjugular intrahepatic portosystemic shunt vs conservative treatment for recurrent ascites: A propensity score matched comparison
Abstract
Background: Transjugular intrahepatic portosystemic shunt (TIPS) placement is an effective intervention for recurrent tense ascites. Some studies show an increased risk of acute on chronic liver failure (ACLF) associated with TIPS placement. It is not clear whether ACLF in this context is a consequence of TIPS or of the pre-existing liver disease.
Aim: To better understand the risks of TIPS in this challenging setting and to compare them with those of conservative therapy.
Methods: Two hundred and fourteen patients undergoing their first TIPS placement for recurrent tense ascites at our tertiary-care center between 2007 and 2017 were identified (TIPS group). Three hundred and ninety-eight patients of the same time interval with liver cirrhosis and recurrent tense ascites not undergoing TIPS placement (No TIPS group) were analyzed as a control group. TIPS indication, diagnosis of recurrent ascites, further diagnoses and clinical findings were obtained from a database search and patient records. The in-hospital mortality and ACLF incidence of both groups were compared using 1:1 propensity score matching and multivariate logistic regressions.
Results: After propensity score matching, the TIPS and No TIPS groups were comparable in terms of laboratory values and ACLF incidence at hospital admission. There was no detectable difference in mortality (TIPS: 11/214, No TIPS 13/214). During the hospital stay, ACLF occurred more frequently in the TIPS group than in the No TIPS group (TIPS: 70/214, No TIPS: 57/214, P = 0.04). This effect was confined to patients with severely impaired liver function at hospital admission as indicated by a significant interaction term of Child score and TIPS placement in multivariate logistic regression. The TIPS group had a lower ACLF incidence at Child scores < 8 points and a higher ACLF incidence at ≥ 11 points. No significant difference was found between groups in patients with Child scores of 8 to 10 points.
Conclusion: TIPS placement for recurrent tense ascites is associated with an increased rate of ACLF in patients with severely impaired liver function but does not result in higher in-hospital mortality.
Keywords: Acute on chronic liver failure; Ascites; Liver cirrhosis; Mortality; Propensity score; Transjugular intrahepatic portosystemic shunt.
©The Author(s) 2022. Published by Baishideng Publishing Group Inc. All rights reserved.
Conflict of interest statement
Conflict-of-interest statement: There are no conflicts of interest to report.
Figures
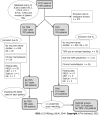

References
-
- Lebrec D, Giuily N, Hadengue A, Vilgrain V, Moreau R, Poynard T, Gadano A, Lassen C, Benhamou JP, Erlinger S. Transjugular intrahepatic portosystemic shunts: comparison with paracentesis in patients with cirrhosis and refractory ascites: a randomized trial. French Group of Clinicians and a Group of Biologists. J Hepatol. 1996;25:135–144. - PubMed
-
- Ginès P, Uriz J, Calahorra B, Garcia-Tsao G, Kamath PS, Del Arbol LR, Planas R, Bosch J, Arroyo V, Rodés J. Transjugular intrahepatic portosystemic shunting versus paracentesis plus albumin for refractory ascites in cirrhosis. Gastroenterology. 2002;123:1839–1847. - PubMed
-
- Sanyal AJ, Genning C, Reddy KR, Wong F, Kowdley KV, Benner K, McCashland T North American Study for the Treatment of Refractory Ascites Group. The North American Study for the Treatment of Refractory Ascites. Gastroenterology. 2003;124:634–641. - PubMed
-
- Rössle M, Ochs A, Gülberg V, Siegerstetter V, Holl J, Deibert P, Olschewski M, Reiser M, Gerbes AL. A comparison of paracentesis and transjugular intrahepatic portosystemic shunting in patients with ascites. N Engl J Med. 2000;342:1701–1707. - PubMed
-
- Salerno F, Merli M, Riggio O, Cazzaniga M, Valeriano V, Pozzi M, Nicolini A, Salvatori F. Randomized controlled study of TIPS versus paracentesis plus albumin in cirrhosis with severe ascites. Hepatology. 2004;40:629–635. - PubMed
MeSH terms
LinkOut - more resources
Full Text Sources

