Predictors of Retention and Drug Use Among Patients With Opioid Use Disorder Transferred to a Specialty "Second Chance" Methadone Program
- PMID: 36407024
- PMCID: PMC9669697
- DOI: 10.1177/11782218221138335
Predictors of Retention and Drug Use Among Patients With Opioid Use Disorder Transferred to a Specialty "Second Chance" Methadone Program
Abstract
Background: Many patients in methadone treatment have difficulty achieving or maintaining drug abstinence, and many clinics have policies that lead to discharging these patients. We designed a pilot "Second Chance" (SC) program for patients scheduled to be discharged from other local methadone clinics to be transferred to our clinic.
Aim: Determine whether SC patients' retention and opioid use is related to physical or mental health conditions, non-opioid substance use, or treatment features.
Methods: From December 2012 to December 2014, this program enrolled 70 patients who were discharged from other clinics in the area; we were their last remaining option for methadone treatment. Unlike the clinic's standard policies, the treatment focus for SC patients was retention rather than abstinence. This program focused on connection to care (eg, psychiatric services) and enabled patients to continue receiving services despite ongoing substance use. Each patient was assessed at treatment entry and followed until June 2016 to evaluate outcomes.
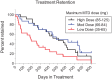
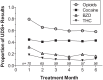
Results: SC patients receiving disability benefits (n = 37) vs. non-disabled (n = 33) had significantly (P < .05) higher rates of current DSM-IV Axis I psychiatric diagnosis (97% vs 70%), prescriptions for opioids (84% vs 55%) and benzodiazepines (65% vs 27%), and higher methadone doses at admission (58 vs 46 mg) but did not differ significantly in rates of 6-month or 1-year retention (77% and 56%, respectively) or all-drug use (39% positive urine drug screens). Methadone doses >65 mg predicted significantly longer retention and less opioid use, but these effects were not moderated by baseline characteristics.
Conclusions: Patients in methadone treatment struggling to achieve abstinence may benefit from retention-oriented harm-reduction programs. Higher methadone doses can improve retention and opioid abstinence despite psychiatric comorbidities. Further work is needed to improve program implementation and outcomes in this complex population.
Keywords: Methadone treatment; benzodiazepines; disability; harm reduction; opioid; retention.
© The Author(s) 2022.
Conflict of interest statement
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Figures
Similar articles
-
Gender-specific predictors of retention and opioid abstinence during methadone maintenance treatment.J Subst Abuse Treat. 2015 Jul;54:37-43. doi: 10.1016/j.jsat.2015.01.009. Epub 2015 Jan 31. J Subst Abuse Treat. 2015. PMID: 25795601
-
Methadone induction in primary care for opioid dependence: a pragmatic randomized trial (ANRS Methaville).PLoS One. 2014 Nov 13;9(11):e112328. doi: 10.1371/journal.pone.0112328. eCollection 2014. PLoS One. 2014. PMID: 25393311 Free PMC article. Clinical Trial.
-
Gender-specific predictors of methadone treatment outcomes among African Americans at an urban clinic.Subst Abus. 2019;40(2):185-193. doi: 10.1080/08897077.2018.1547810. Epub 2019 Mar 19. Subst Abus. 2019. PMID: 30888262
-
Primary care management of opioid use disorders: Abstinence, methadone, or buprenorphine-naloxone?Can Fam Physician. 2017 Mar;63(3):200-205. Can Fam Physician. 2017. PMID: 28292795 Free PMC article. Review.
-
Depression and Outcomes of Methadone and Buprenorphine Treatment Among People with Opioid Use Disorders: A Literature Review.J Dual Diagn. 2020 Apr-Jun;16(2):191-207. doi: 10.1080/15504263.2020.1726549. Epub 2020 Feb 23. J Dual Diagn. 2020. PMID: 32089124 Review.
Cited by
-
"They make it too hard and too many hoops to jump": system and organizational barriers to drug treatment during epidemic rates of opioid overdose.Harm Reduct J. 2024 Feb 27;21(1):52. doi: 10.1186/s12954-024-00964-5. Harm Reduct J. 2024. PMID: 38413972 Free PMC article.
References
-
- Krawczyk N, Jent V, Hadland SE, Cerdá M. Utilization of medications for opioid use disorder across US states: relationship to treatment availability and overdose mortality. J Addict Med. 2022;16:114-117. - PubMed
Grants and funding
LinkOut - more resources
Full Text Sources

