Colorectal Cancer Stage at Diagnosis Before vs During the COVID-19 Pandemic in Italy
- PMID: 36409496
- PMCID: PMC9679872
- DOI: 10.1001/jamanetworkopen.2022.43119
Colorectal Cancer Stage at Diagnosis Before vs During the COVID-19 Pandemic in Italy
Abstract
Importance: Delays in screening programs and the reluctance of patients to seek medical attention because of the outbreak of SARS-CoV-2 could be associated with the risk of more advanced colorectal cancers at diagnosis.
Objective: To evaluate whether the SARS-CoV-2 pandemic was associated with more advanced oncologic stage and change in clinical presentation for patients with colorectal cancer.
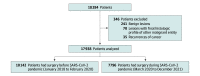
Design, setting, and participants: This retrospective, multicenter cohort study included all 17 938 adult patients who underwent surgery for colorectal cancer from March 1, 2020, to December 31, 2021 (pandemic period), and from January 1, 2018, to February 29, 2020 (prepandemic period), in 81 participating centers in Italy, including tertiary centers and community hospitals. Follow-up was 30 days from surgery.
Exposures: Any type of surgical procedure for colorectal cancer, including explorative surgery, palliative procedures, and atypical or segmental resections.
Main outcomes and measures: The primary outcome was advanced stage of colorectal cancer at diagnosis. Secondary outcomes were distant metastasis, T4 stage, aggressive biology (defined as cancer with at least 1 of the following characteristics: signet ring cells, mucinous tumor, budding, lymphovascular invasion, perineural invasion, and lymphangitis), stenotic lesion, emergency surgery, and palliative surgery. The independent association between the pandemic period and the outcomes was assessed using multivariate random-effects logistic regression, with hospital as the cluster variable.
Results: A total of 17 938 patients (10 007 men [55.8%]; mean [SD] age, 70.6 [12.2] years) underwent surgery for colorectal cancer: 7796 (43.5%) during the pandemic period and 10 142 (56.5%) during the prepandemic period. Logistic regression indicated that the pandemic period was significantly associated with an increased rate of advanced-stage colorectal cancer (odds ratio [OR], 1.07; 95% CI, 1.01-1.13; P = .03), aggressive biology (OR, 1.32; 95% CI, 1.15-1.53; P < .001), and stenotic lesions (OR, 1.15; 95% CI, 1.01-1.31; P = .03).
Conclusions and relevance: This cohort study suggests a significant association between the SARS-CoV-2 pandemic and the risk of a more advanced oncologic stage at diagnosis among patients undergoing surgery for colorectal cancer and might indicate a potential reduction of survival for these patients.
Conflict of interest statement
References
-
- World Health Organization . WHO coronavirus (COVID-19) dashboard. Published June 13, 2022. Accessed June 14, 2022. https://covid19.who.int/
Publication types
MeSH terms
LinkOut - more resources
Full Text Sources
Medical
Miscellaneous