Pattern of Radiotherapy Treatment in Low-Risk, Intermediate-Risk, and High-Risk Prostate Cancer Patients: Analysis of National Cancer Database
- PMID: 36428595
- PMCID: PMC9688758
- DOI: 10.3390/cancers14225503
Pattern of Radiotherapy Treatment in Low-Risk, Intermediate-Risk, and High-Risk Prostate Cancer Patients: Analysis of National Cancer Database
Abstract
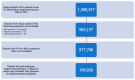
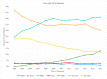
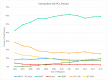
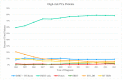
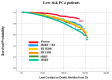
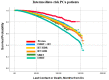
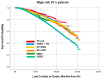
Background: In this study, the utilization rates and survival outcomes of different radiotherapy techniques are compared in prostate cancer (PCa) patients stratified by risk group. Methods: We analyzed an extensive data set of N0, M0, non-surgical PCa patients diagnosed between 2004 and 2015 from the National Cancer Database (NCDB). Patients were grouped into six categories based on RT modality: an intensity-modulated radiation therapy (IMRT) group with brachytherapy (BT) boost, IMRT with/without IMRT boost, proton therapy, stereotactic body radiation therapy (SBRT), low-dose-rate brachytherapy (BT LDR), and high-dose-rate brachytherapy (BT HDR). Patients were also stratified by the National Comprehensive Cancer Network (NCCN) guidelines: low-risk (clinical stage T1−T2a, Gleason Score (GS) ≤ 6, and Prostate-Specific Antigen (PSA) < 10), intermediate-risk (clinical stage T2b or T2c, GS of 7, or PSA of 10−20), and high-risk (clinical stage T3−T4, or GS of 8−10, or PSA > 20). Overall survival (OS) probability was determined using a Kaplan−Meier estimator. Univariate and multivariate analyses were performed by risk group for the six treatment modalities. Results: The most utilized treatment modality for all PCa patients was IMRT (53.1%). Over the years, a steady increase in SBRT utilization was observed, whereas BT HDR usage declined. IMRT-treated patient groups exhibited relatively lower survival probability in all risk categories. A slightly better survival probability was observed for the proton therapy group. Hormonal therapy was used for a large number of patients in all risk groups. Conclusion: This study revealed that IMRT was the most common treatment modality for PCa patients. Brachytherapy, SBRT, and IMRT+BT exhibited similar survival rates, whereas proton showed slightly better overall survival across the three risk groups. However, analysis of the demographics indicates that these differences are at least in part due to selection bias.
Keywords: IMRT; SBRT; brachytherapy; overall survival; prostate cancer; proton-beam therapy; radiotherapy.
Conflict of interest statement
The authors declare no conflict of interest.
Figures
Similar articles
-
SBRT and HDR brachytherapy produce lower PSA nadirs and different PSA decay patterns than conventionally fractionated IMRT in patients with low- or intermediate-risk prostate cancer.Pract Radiat Oncol. 2016 Jul-Aug;6(4):268-275. doi: 10.1016/j.prro.2015.11.002. Epub 2015 Nov 10. Pract Radiat Oncol. 2016. PMID: 26850649
-
Prostate-specific antigen kinetics and biochemical control following stereotactic body radiation therapy, high dose rate brachytherapy, and low dose rate brachytherapy: A multi-institutional analysis of 3502 patients.Radiother Oncol. 2020 Oct;151:26-32. doi: 10.1016/j.radonc.2020.07.014. Epub 2020 Jul 11. Radiother Oncol. 2020. PMID: 32663537
-
Comparison of Image-Guided Intensity-Modulated Radiotherapy and Low-dose Rate Brachytherapy with or without External Beam Radiotherapy in Patients with Localized Prostate Cancer.Sci Rep. 2018 Jul 12;8(1):10538. doi: 10.1038/s41598-018-28730-1. Sci Rep. 2018. PMID: 30002393 Free PMC article.
-
Brachytherapy boost (BT-boost) or stereotactic body radiation therapy boost (SBRT-boost) for high-risk prostate cancer (HR-PCa).Cancer Radiother. 2021 Jun;25(4):400-409. doi: 10.1016/j.canrad.2020.11.004. Epub 2021 Jan 18. Cancer Radiother. 2021. PMID: 33478838
-
High-dose-rate intensity-modulated brachytherapy with external beam radiotherapy for prostate cancer: California endocurietherapy's 10-year results.Int J Radiat Oncol Biol Phys. 2005 Apr 1;61(5):1306-16. doi: 10.1016/j.ijrobp.2004.08.014. Int J Radiat Oncol Biol Phys. 2005. PMID: 15817332 Review.
Cited by
-
The role of eIF4F-driven mRNA translation in regulating the tumour microenvironment.Nat Rev Cancer. 2023 Jun;23(6):408-425. doi: 10.1038/s41568-023-00567-5. Epub 2023 May 4. Nat Rev Cancer. 2023. PMID: 37142795 Review.
References
-
- Society A.C. Cancer Statistics Center. 2021. [(accessed on 1 February 2022)]. Available online: https://cancerstatisticscenter.cancer.org/
-
- Network NCC NCCN Guidelines Version 2.2021 Prostate Cancer. 2021. [(accessed on 1 February 2022)]. Available online: https://www.nccn.org/professionals/physician_gls/pdf/prostate.pdf.
-
- Tsubokura T., Yamazaki H., Masui K., Sasaki N., Shimizu D., Suzuki G., Nakamura S., Yamada K., Okihara K., Shiraishi T., et al. Comparison of Image-Guided Intensity-Modulated Radiotherapy and Low-dose Rate Brachytherapy with or without External Beam Radiotherapy in Patients with Localized Prostate Cancer. Sci. Rep. 2018;8:10538. doi: 10.1038/s41598-018-28730-1. - DOI - PMC - PubMed
LinkOut - more resources
Full Text Sources
Research Materials
Miscellaneous

