Adherence to inhaled corticosteroids in relation to quality of life and symptoms of anxiety and depression in asthma
- PMID: 36452910
- PMCID: PMC9704108
- DOI: 10.1080/20018525.2022.2149920
Adherence to inhaled corticosteroids in relation to quality of life and symptoms of anxiety and depression in asthma
Abstract
Background: Poor asthma control, often caused by non-adherence with controller medication, is a well-known risk factor for impaired quality of life (QoL) and major mood disorders (MMD). Previous studies have shown a relationship between non-adherence, lower QoL, and MMD across chronic diseases, but the relationship remains uncertain in asthma.
Methods: All asthma patients followed at the respiratory outpatient clinic at Copenhagen University Hospital - Hvidovre were invited to fill-in the Hospital Anxiety and Depression Scale (HADS) and the Mini Asthma Quality of Life Questionnaire (miniAQLQ). Medication Possession Ratio (MPR) was calculated using pharmacy redemption data. Relationships between questionnaire scores, inhaled corticosteroid MPR and use of rescue medication were investigated using Pearson correlation and multivariable linear regression adjusted for age, sex, FEV1, and GINA Step. Data from scheduled visits were collected from patients' medical records.
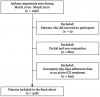
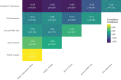
Results: A total of 308 patients (73% females, median age 51 years (interquartile range (IQR) 37, 62)) completed the questionnaires and had 1-year medication data available. Median adherence to inhaled corticosteroids (ICS) was 57% (35%, 75%) with 18% of patients having adherence above 80%. Of the participating patients, 14% and 27% reported depressive and anxiety-related symptoms, respectively, and 72% reported impaired QoL. In correlation analyses, ICS adherence was not significantly associated with either prevalence of MMD symptoms or impaired QoL in asthma patients. However, a strong correlation was found between ACQ-6 and both MMD symptoms and impaired QoL, as well as between rescue medication use and impaired QoL. In adjusted analysis, however, the latter correlation was no longer statistically significant.
Conclusion: Our results suggest that ICS adherence is not directly correlated with either impaired quality of life or major mood disorder symptoms in asthma patients. Self-reported asthma control, on the other hand, is strongly correlated with both QoL and MMD.
Keywords: Asthma; anxiety; depression; inhaled corticosteroids; major mood disorder.
© 2022 The Author(s). Published by Informa UK Limited, trading as Taylor & Francis Group.
Conflict of interest statement
MRL has nothing to declare. KEJH has received personal fees from AstraZeneca, Chiesi, GSK, Sanofi Genzyme, and TEVA. CSU has received personal fees from AstraZeneca, GSK, TEVA, Sanofi Genzyme, Boehringer-Ingelheim, Chiesi, Orion Pharma, Novartis, ALK-Abello, Mundipharma, and Actelion.
Figures

Similar articles
-
Self-reported vs. objectively assessed adherence to inhaled corticosteroids in asthma.Asthma Res Pract. 2021 May 31;7(1):7. doi: 10.1186/s40733-021-00072-2. Asthma Res Pract. 2021. PMID: 34059120 Free PMC article.
-
Determining Persistence with an Inhaled Corticosteroid in Asthma: Assessment Using an Objective Measurement vs the Self-Reported Foster Score.J Asthma Allergy. 2022 Jan 5;15:25-33. doi: 10.2147/JAA.S332756. eCollection 2022. J Asthma Allergy. 2022. PMID: 35023932 Free PMC article.
-
Enrolment in an Asthma Management Program during Pregnancy and Adherence with Inhaled Corticosteroids: The 'Management of Asthma during Pregnancy' Program.Respiration. 2016;92(1):9-15. doi: 10.1159/000447244. Epub 2016 Jun 28. Respiration. 2016. PMID: 27348313 Clinical Trial.
-
As-needed ICS-LABA in Mild Asthma: What Does the Evidence Say?Drugs. 2019 Nov;79(16):1729-1737. doi: 10.1007/s40265-019-01202-0. Drugs. 2019. PMID: 31584145 Review.
-
Impact of educational intervention by community pharmacists on asthma clinical outcomes, quality of life and medication adherence: A systematic review and meta-analysis.J Clin Pharm Ther. 2021 Oct;46(5):1254-1262. doi: 10.1111/jcpt.13419. Epub 2021 Apr 5. J Clin Pharm Ther. 2021. PMID: 33817821
Cited by
-
Environmental, healthcare and societal impacts of asthma: a UK model-based assessment.ERJ Open Res. 2024 Jul 22;10(4):00577-2023. doi: 10.1183/23120541.00577-2023. eCollection 2024 Jul. ERJ Open Res. 2024. PMID: 39040585 Free PMC article.
-
Identifying and characterising asthma subgroups at high risk of severe exacerbations using machine learning and longitudinal real-world data.BMJ Health Care Inform. 2025 Jul 7;32(1):e101282. doi: 10.1136/bmjhci-2024-101282. BMJ Health Care Inform. 2025. PMID: 40623771 Free PMC article.
-
Asthma medication adherence, control, and psychological symptoms: a cross-sectional study.BMC Pulm Med. 2024 Apr 19;24(1):189. doi: 10.1186/s12890-024-02995-x. BMC Pulm Med. 2024. PMID: 38641584 Free PMC article.
References
-
- Leander M, Lampa E, Rask-Andersen A, et al. Impact of anxiety and depression on respiratory symptoms. Respir Med. 2014. Nov;108(11):1594–8. - PubMed
-
- Bateman ED, Hurd SS, Barnes PJ, et al. Global strategy for asthma management and prevention. GINA. 2020. - PubMed
-
- Vos T, Abajobir AA, Abbafati C, et al. Global, regional, and national incidence, prevalence, and years lived with disability for 328 diseases and injuries for 195 countries, 1990-2016: a systematic analysis for the global burden of disease study 2016. Lancet. 2017;390(10100):1211–1259. - PMC - PubMed
-
- von Bülow A, Kriegbaum M, Backer V, et al. The prevalence of severe asthma and low asthma control among Danish adults. J Allergy Clin Immunol Pract. 2014;2(6):759–767. - PubMed
-
- Backer V, Bornemann M, Knudsen D, et al. Scheduled asthma management in general practice generally improve asthma control in those who attend. Respir Med. 2012;106(5):635–641. - PubMed
LinkOut - more resources
Full Text Sources
