Treatment, Survival, and Demographics in Temporal Bone Malignancies: A Pooled Data Analysis
- PMID: 36452912
- PMCID: PMC9704031
- DOI: 10.7759/cureus.31973
Treatment, Survival, and Demographics in Temporal Bone Malignancies: A Pooled Data Analysis
Abstract
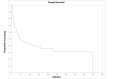
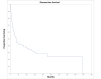
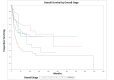
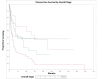
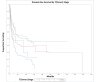
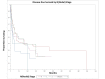
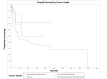
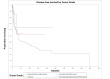
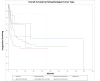
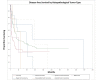
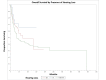
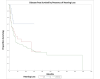
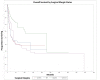
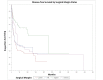
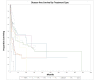
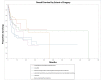
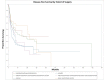
Temporal bone malignancies are relatively uncommon tumors. Their location adjacent to vital structures such as the carotid artery, jugular vein, otic capsule, and temporal lobe can make their treatment potentially challenging. The purpose of this study was to compare outcomes in temporal bone malignancies obtained via pooled literature data. The study sought to examine factors affecting survival in temporal bone malignancies based on the studies in the existing published literature. A systematic search was conducted on the PubMed (Medline), Embase, and Google Scholar databases to identify relevant studies from 1951 to 2022 that described the treatment of temporal bone malignancies. Articles that fulfilled the inclusion criteria were assessed and analyzed by the author. The literature search identified 5875 case series and case reports, and 161 of them contained sufficient data to be included in the pooled data analysis, involving a total of 825 patients. Multivariate analysis of the pooled literature data showed that overall stage, presence of facial palsy, and surgical margin status significantly affected overall survival (OS), while overall stage and presence of facial palsy significantly affected disease-free survival (DFS). To summarize, this study examined pooled survival data on demographics, treatment, and survival of patients with temporal bone malignancies utilizing an extensive literature-based pooled data meta-analysis. Overall stage, facial nerve status, and surgical margin status appeared to most strongly affect survival in patients with temporal bone malignancies.
Keywords: cancer; ear; head and neck; oncology; survival.
Copyright © 2022, Gore et al.
Conflict of interest statement
The authors have declared that no competing interests exist.
Figures








Similar articles
-
Temporal bone resection for lateral skull-base malignancies.J Neurooncol. 2020 Dec;150(3):437-444. doi: 10.1007/s11060-020-03445-4. Epub 2020 Feb 27. J Neurooncol. 2020. PMID: 32108295 Review.
-
Temporal-Parotid Resection for Malignant Parotid Tumors: A Systematic Review.Laryngoscope. 2025 May 14. doi: 10.1002/lary.32267. Online ahead of print. Laryngoscope. 2025. PMID: 40365836 Review.
-
The role of perineural invasion in parotid malignancy outcomes: A systematic review and meta-analysis.Oral Oncol. 2022 Jul;130:105937. doi: 10.1016/j.oraloncology.2022.105937. Epub 2022 Jun 1. Oral Oncol. 2022. PMID: 35662029
-
Temporal bone malignancies involving the jugular foramen: diagnosis and management.ORL J Otorhinolaryngol Relat Spec. 2014;76(4):227-35. doi: 10.1159/000368320. Epub 2014 Nov 14. ORL J Otorhinolaryngol Relat Spec. 2014. PMID: 25401454
-
Temporal Bone Resection for Squamous Cell Carcinoma of the Lateral Skull Base: Systematic Review and Meta-analysis.Otolaryngol Head Neck Surg. 2023 Feb;168(2):154-164. doi: 10.1177/01945998221084912. Otolaryngol Head Neck Surg. 2023. PMID: 35290141
References
-
- Temporal bone malignancies. Gidley PW, DeMonte F. Neurosurg Clin N Am. 2013;24:97–110. - PubMed
-
- Critical evaluation of the Newcastle-Ottawa scale for the assessment of the quality of nonrandomized studies in meta-analyses. Stang A. Eur J Epidemiol. 2010;25:603–605. - PubMed
-
- Otopathology in angiosarcoma of the temporal bone. Chen JX, Kozin ED, O'Malley J, et al. Laryngoscope. 2019;129:737–742. - PubMed
Publication types
LinkOut - more resources
Full Text Sources
