Percutaneous nephrostomy for complex renal stones: Percutaneous renal access behind the stone versus renal calyx dilation
- PMID: 36454857
- PMCID: PMC9714915
- DOI: 10.1371/journal.pone.0278485
Percutaneous nephrostomy for complex renal stones: Percutaneous renal access behind the stone versus renal calyx dilation
Abstract
Objective: To evaluate the technical success rate and complications associated with percutaneous nephrostomy (PCN) via percutaneous renal access behind the stone and renal calyx dilation in patients with complex renal stones.
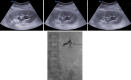
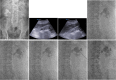
Materials and methods: From January 2010 to February 2021, we identified 69 patients with 70 complex renal stones who underwent PCN. Complex renal stones were classified as simple (renal pelvis only) (27.1%, 19/70), borderline staghorn (8.6%, 6/70), partial staghorn (51.4%, 36/70), or complete staghorn (12.9%, 9/70). All PCNs were performed under ultrasound and fluoroscopic guidance using one of two renal-entry techniques: puncture behind the stone (56%, 39/70) or renal calyx dilation (44%, 31/70). Then, we retrospectively evaluated the technical success rates and complications associated with each renal entry access technique.
Results: The overall technical success rate was 100%, and the complication rate was 20.0% (14/70). For those who underwent renal access behind the stone, the complication rate was 15.4% (6/39), and six patients (six PCNs) had transient gross hematuria. For those who underwent dilated renal calyx entry, the complication rate was 25.8% (8/31), and one patient had significant bleeding complications requiring transfusion. Furthermore, seven patients (seven PCNs) had transient gross hematuria. Overall, the complication rates did not differ between the technique groups (p = 0.279).
Conclusion: PCN for complex renal stones has a high technical success rate and an acceptable complication rate regardless of the specific technique. Renal entry behind the stone is as safe and feasible as approaching via a dilated renal calyx.
Copyright: © 2022 Ahn et al. This is an open access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.
Conflict of interest statement
The authors have declared that no competing interests exist.
Figures
Similar articles
-
The effect of stone localization on the success and complication rates of percutaneous nephrolithotomy.Urol J. 2014 Nov 30;11(6):1938-42. Urol J. 2014. PMID: 25433471
-
Does Access Location Influence Outcome of Percutaneous Nephrolithotomy in Staghorn Stones?J Coll Physicians Surg Pak. 2021 Sep;31(9):1075-1080. doi: 10.29271/jcpsp.2021.09.1075. J Coll Physicians Surg Pak. 2021. PMID: 34500524
-
Single upper-pole percutaneous access for treatment of > or = 5-cm complex branched staghorn calculi: is shockwave lithotripsy necessary?J Endourol. 2002 Sep;16(7):477-81. doi: 10.1089/089277902760367430. J Endourol. 2002. PMID: 12396440
-
Evolution of the technique of combination therapy for staghorn calculi: a decreasing role for extracorporeal shock wave lithotripsy.J Urol. 1992 Sep;148(3 Pt 2):1058-62. doi: 10.1016/s0022-5347(17)36816-7. J Urol. 1992. PMID: 1507330 Review.
-
Management of staghorn calculus: single puncture with judicious use of the flexible nephroscope.Curr Opin Urol. 2008 Mar;18(2):224-8. doi: 10.1097/MOU.0b013e3282f517c0. Curr Opin Urol. 2008. PMID: 18303549 Review.
Cited by
-
Machine learning algorithm to predict postoperative bleeding complications after lateral decubitus percutaneous nephrolithotomy.Medicine (Baltimore). 2024 Jan 26;103(4):e37050. doi: 10.1097/MD.0000000000037050. Medicine (Baltimore). 2024. PMID: 38277513 Free PMC article.
-
Prospective Comparative Analysis of Supine Versus Prone Percutaneous Nephrolithotomy in Patients with Complex Renal Stone Disease and Difficult Anatomy.Urol Res Pract. 2024 Mar;50(2):107-114. doi: 10.5152/tud.2024.24010. Urol Res Pract. 2024. PMID: 39128124 Free PMC article.
-
Nephrostomy (PCN) versus nephroureteral stent (Double JJ); An ongoing battle.Urologia. 2025 Aug;92(3):424-431. doi: 10.1177/03915603251316702. Epub 2025 Feb 10. Urologia. 2025. PMID: 39925227 Free PMC article. Review.
References
MeSH terms
LinkOut - more resources
Full Text Sources

