Primary targeted medical therapy for management of bilateral head and neck lymphatic malformations in infants
- PMID: 36459725
- PMCID: PMC10243723
- DOI: 10.1016/j.ijporl.2022.111371
Primary targeted medical therapy for management of bilateral head and neck lymphatic malformations in infants
Abstract
Objectives: Patients born with bilateral head and neck lymphatic malformations (BHNLMs) often require multiple invasive treatments, including tracheostomy. We hypothesized that primary targeted medical therapy (pTMT) with diagnostic needle aspiration reduces the need for invasive therapy such as surgical resection and/or sclerotherapy.
Methods: Retrospective case review was performed of infants with BHNLMs (Grade 2 or De Serres stage IV and V) treated only at our institution from 2000 to 2021. Patients were divided into two cohorts: those managed with pTMT and those managed with observation, sclerotherapy, or surgical intervention (non-pTMT). Data regarding interventions, clinical outcomes, morbidity, and mortality were analyzed with descriptive statistics.
Results: Nine children with BHNLMs met inclusion criteria. Three (33%) were in the pTMT cohort and six (66%) were non-pTMT. Eight (89%) malformations were genotyped, and all demonstrated hotspot PIK3CA variants. All pTMT patients had sirolimus initiated in the first month of life and underwent needle aspiration of malformation cyst fluid for cell-free DNA samples. All pTMT patients tolerated medical therapy. For the non-pTMT cohort, primary treatment included none (deceased, n = 1, 17%), observation with needle aspiration (n = 1, 17%), surgical resection (n = 2, 33%), or combination surgery and sclerotherapy (n = 2, 33%). Intubation duration, intensive care and initial hospital length of stay were not different between cohorts. Four non-pTMT patients (67%) required tracheostomy, and two (33%) died prior to discharge. All pTMT patients survived and none required tracheostomy. Non-pTMT patients required a median of two invasive therapies prior to discharge (IQR 1-4) and a mean total of 13 over the course of their lifetime (IQR 1-16), compared to the pTMT group who did not require any lifetime invasive therapy, even after initial pTMT and discharge home.
Conclusion: This study compares patients with BHNLMs (Grade 2) treated with pTMT versus those treated with observation or invasive therapy. Patients treated with pTMT required no surgical or invasive procedural treatment of their malformations, no tracheostomy placement, no unplanned readmissions after discharge, and had no mortalities. Needle aspiration was useful as a therapeutic adjunct for cell-free DNA diagnosis of PIK3CA variants, which guided TMT.
Keywords: Lymphatic malformation; Needle aspiration; PI3K; Surgery; Targeted therapy; Treatment.
Copyright © 2022. Published by Elsevier B.V.
Conflict of interest statement
Declaration of competing interest Dr. Randall Bly is co-founder and holds a financial interest of ownership equity with Edus Health, Inc and EigenHealth, Inc. He is consultant and stockholder, Spiway, LLC. These are not related to this study. All other authors do not have information to disclose.
Figures
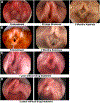
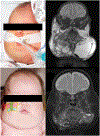
Similar articles
-
Active Observation as an Alternative to Invasive Treatments for Pediatric Head and Neck Lymphatic Malformations.Laryngoscope. 2021 Jun;131(6):1392-1397. doi: 10.1002/lary.29180. Epub 2020 Oct 27. Laryngoscope. 2021. PMID: 33107991
-
Utilizing immediate preoperative n-BCA in the resection of head and neck venous and lymphatic malformations.Int J Pediatr Otorhinolaryngol. 2020 Nov;138:110388. doi: 10.1016/j.ijporl.2020.110388. Epub 2020 Sep 17. Int J Pediatr Otorhinolaryngol. 2020. PMID: 33152979
-
Primary surgery vs primary sclerotherapy for head and neck lymphatic malformations.JAMA Otolaryngol Head Neck Surg. 2014 Jan;140(1):41-5. doi: 10.1001/jamaoto.2013.5849. JAMA Otolaryngol Head Neck Surg. 2014. PMID: 24288004
-
Surgery versus sclerotherapy versus combined therapy in head and neck lymphatic malformations in the pediatric population: systematic review and meta-analysis.Eur Arch Otorhinolaryngol. 2024 Sep;281(9):4529-4539. doi: 10.1007/s00405-024-08661-6. Epub 2024 May 7. Eur Arch Otorhinolaryngol. 2024. PMID: 38714549 Free PMC article.
-
Current treatment paradigms in the management of lymphatic malformations.Laryngoscope. 2011 Jan;121(1):56-9. doi: 10.1002/lary.20768. Laryngoscope. 2011. PMID: 21046541 Review.
Cited by
-
Incidence and Factors Associated With Spontaneous Regression in Head and Neck Lymphatic Malformations.JAMA Otolaryngol Head Neck Surg. 2025 May 1;151(5):503-512. doi: 10.1001/jamaoto.2025.0104. JAMA Otolaryngol Head Neck Surg. 2025. PMID: 40146172
-
Treatments and Outcomes of Pediatric Head and Neck Lymphatic Malformations: A 20-Year Single Institution Experience.Otolaryngol Head Neck Surg. 2025 Mar;172(3):1026-1035. doi: 10.1002/ohn.1077. Epub 2024 Dec 15. Otolaryngol Head Neck Surg. 2025. PMID: 39675029 Free PMC article.
References
MeSH terms
Grants and funding
LinkOut - more resources
Full Text Sources
Miscellaneous

