First-Trimester Triglyceride-Glucose Index and Risk of Pregnancy-Related Complications: A Prospective Birth Cohort Study in Southeast China
- PMID: 36465992
- PMCID: PMC9717426
- DOI: 10.2147/DMSO.S378964
First-Trimester Triglyceride-Glucose Index and Risk of Pregnancy-Related Complications: A Prospective Birth Cohort Study in Southeast China
Abstract
Purpose: To evaluate the relationships of the triglyceride-glucose (TyG) index with pregnancy-related complications (PRCs) and to clarify the predictability of the TyG index for PRCs.
Patients and methods: Totally of 11,387 women with a singleton pregnancy were prospectively followed until after delivery. Maternal fasting lipids and glucose concentration were measured in the first trimester (11 weeks gestation on average). The TyG index was calculated as ln [triglyceride (mg/dL) × fasting plasma glucose (mg/dL)/2]. We used generalized linear models to calculate the relative risks and 95% confidence intervals. Receiver-operating characteristic curve analysis was employed to assess the ability of the TyG index to predict the risks of PRCs.
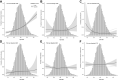
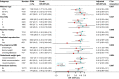
Results: Smooth spline reveals that the probability of gestational diabetes mellitus (GDM) is intensified with the increasing TyG index. Multivariate logistic regression adjusted for risk factors demonstrates a 1-unit and a 1-SD increment in the TyG index raises the risk of GDM by 3.63 and 1.57 times, respectively. Identically, the risk of GDM maximizes in the TyG quintile 5 (OR: 3.14; 95% CI: 2.55~3.85) relative to the lowest TyG index group. However, no association between TyG index and the risk of other PRCs was observed after full adjustment. The area under receiver operating characteristic curves is 0.647 (95% CI: 0.632-0.66) for GDM, and the optimal predictive cut-off is 8.55, with a specificity of 0.679 and sensitivity of 0.535.
Conclusion: The first-trimester TyG index is significantly associated with the risk of incident GDM, while the relationships between the TyG index and other PRCs need further exploration.
Keywords: first-trimester; gestational diabetes mellitus; pregnancy-related complications; singleton pregnancy; triglyceride-glucose index.
© 2022 Li et al.
Conflict of interest statement
The authors report no conflicts of interest in this work.
Figures
Similar articles
-
Triglyceride-glucose index in early pregnancy predicts the risk of gestational diabetes: a prospective cohort study.Lipids Health Dis. 2024 Mar 25;23(1):87. doi: 10.1186/s12944-024-02076-2. Lipids Health Dis. 2024. PMID: 38528508 Free PMC article.
-
First-Trimester Triglyceride-Glucose Index and Triglyceride/High-Density Lipoprotein Cholesterol are Predictors of Gestational Diabetes Mellitus Among the Four Surrogate Biomarkers of Insulin Resistance.Diabetes Metab Syndr Obes. 2024 Apr 8;17:1575-1583. doi: 10.2147/DMSO.S454826. eCollection 2024. Diabetes Metab Syndr Obes. 2024. PMID: 38616992 Free PMC article.
-
An elevated triglyceride-glucose index in the first-trimester predicts adverse pregnancy outcomes: a retrospective cohort study.Arch Gynecol Obstet. 2025 Mar;311(3):915-927. doi: 10.1007/s00404-025-07973-0. Epub 2025 Feb 26. Arch Gynecol Obstet. 2025. PMID: 40009162 Free PMC article.
-
The Predictive Ability of Two Triglyceride-Associated Indices for Gestational Diabetes Mellitus and Large for Gestational Age Infant Among Chinese Pregnancies: A Preliminary Cohort Study.Diabetes Metab Syndr Obes. 2020 Jun 16;13:2025-2035. doi: 10.2147/DMSO.S251846. eCollection 2020. Diabetes Metab Syndr Obes. 2020. PMID: 32606861 Free PMC article.
-
Association of Triglyceride-Glucose Index with Risk of Large for Gestational Age: A Prospective Cohort Study.Diabetes Metab Syndr Obes. 2023 Nov 27;16:3837-3846. doi: 10.2147/DMSO.S436611. eCollection 2023. Diabetes Metab Syndr Obes. 2023. PMID: 38044980 Free PMC article.
Cited by
-
The Relationship between Coronary Flow Reserve and the TyG Index in Patients with Gestational Diabetes Mellitus.Medicina (Kaunas). 2023 Oct 12;59(10):1811. doi: 10.3390/medicina59101811. Medicina (Kaunas). 2023. PMID: 37893529 Free PMC article.
-
Triglyceride-glucose index in early pregnancy predicts the risk of gestational diabetes: a prospective cohort study.Lipids Health Dis. 2024 Mar 25;23(1):87. doi: 10.1186/s12944-024-02076-2. Lipids Health Dis. 2024. PMID: 38528508 Free PMC article.
-
Causal relationships between metabolic syndrome, plasma metabolites, and female reproductive diseases: insights from a two-step mendelian randomization approach.Nutr Metab (Lond). 2025 Jun 13;22(1):60. doi: 10.1186/s12986-025-00955-8. Nutr Metab (Lond). 2025. PMID: 40514674 Free PMC article.
-
First-Trimester Triglyceride-Glucose Index and Triglyceride/High-Density Lipoprotein Cholesterol are Predictors of Gestational Diabetes Mellitus Among the Four Surrogate Biomarkers of Insulin Resistance.Diabetes Metab Syndr Obes. 2024 Apr 8;17:1575-1583. doi: 10.2147/DMSO.S454826. eCollection 2024. Diabetes Metab Syndr Obes. 2024. PMID: 38616992 Free PMC article.
-
Association of the Triglyceride-Glucose Index During the First Trimester of Pregnancy with Adverse Perinatal Outcomes.Diagnostics (Basel). 2025 Apr 29;15(9):1129. doi: 10.3390/diagnostics15091129. Diagnostics (Basel). 2025. PMID: 40361947 Free PMC article.
References
LinkOut - more resources
Full Text Sources

