Loss of the volume-regulated anion channel components LRRC8A and LRRC8D limits platinum drug efficacy
- PMID: 36467895
- PMCID: PMC7613873
- DOI: 10.1158/2767-9764.CRC-22-0208
Loss of the volume-regulated anion channel components LRRC8A and LRRC8D limits platinum drug efficacy
Abstract
In recent years platinum (Pt) drugs have been found to be especially efficient to treat patients with cancers that lack a proper DNA damage response, e.g. due to dysfunctional BRCA1. Despite this knowledge, we are still missing helpful markers to predict Pt response in the clinic. We have previously shown that volume-regulated anion channels, containing the subunits LRRC8A and LRRC8D, promote the uptake of cisplatin and carboplatin in BRCA1-proficient cell lines. Here, we show that the loss of LRRC8A or LRRC8D significantly reduces the uptake of cis- and carboplatin in BRCA1;p53-deficient mouse mammary tumor cells. This results in reduced DNA damage and in vivo drug resistance. In contrast to Lrrc8a, the deletion of the Lrrc8d gene does not affect the viability and fertility of mice. Interestingly, Lrrc8d-/- mice tolerate a two-fold cisplatin maximum-tolerable dose. This allowed us to establish a mouse model for intensified Pt-based chemotherapy, and we found that an increased cisplatin dose eradicates BRCA1;p53-deficient tumors, whereas eradication is not possible in WT mice. Moreover, we show that decreased expression of LRRC8A/D in head and neck squamous cell carcinoma patients, who are treated with a Pt-based chemoradiotherapy, leads to decreased overall survival of the patients. In particular, high cumulative cisplatin dose treatments lost their efficacy in patients with a low LRRC8A/D expression in their cancers. Our data therefore suggest that LRRC8A and LRRC8D should be included in a prospective trial to predict the success of intensified cis- or car-boplatin-based chemotherapy.
Keywords: BRCA1; HNSCC; LRRC8A; LRRC8D; Platinum drug resistance; VRAC; breast cancer; genetically engineered mouse model; high-dose chemotherapy.
Conflict of interest statement
Declaration of Interests The authors declare no competing interests. Conflict of interest: The authors declare no potential conflicts of interest.
Figures
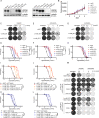




References
-
- Kelland L. The resurgence of platinum-based cancer chemotherapy. Nat Rev Cancer 2007;7:573–84. - PubMed
-
- Rottenberg S, Disler C, Perego P. The rediscovery of platinum-based cancer therapy. Nat Rev Cancer 2021;21:37–50. - PubMed
-
- Pujade-Lauraine E, Fujiwara K, Ledermann JA, Oza AM, Kristeleit R, Ray-Coquard IL, et al. . Avelumab alone or in combination with chemotherapy versus chemotherapy alone in platinum-resistant or platinum-refractory ovarian cancer (JAVELIN Ovarian 200): an open-label, three-arm, randomised, phase 3 study. Lancet Oncol 2021;22:1034–46. - PubMed
-
- Burtness B, Harrington KJ, Greil R, Soulières D, Tahara M, de Castro G, et al. . Pembrolizumab alone or with chemotherapy versus cetuximab with chemotherapy for recurrent or metastatic squamous cell carcinoma of the head and neck (KEYNOTE-048): a randomised, open-label, phase 3 study. Lancet 2019;394:1915–28. - PubMed
-
- Gandhi L, Rodríguez-Abreu D, Gadgeel S, Esteban E, Felip E, De Angelis F, et al. . Pembrolizumab plus chemotherapy in metastatic non-small-cell lung cancer. N Engl J Med 2018;378:2078–92. - PubMed
Publication types
MeSH terms
Substances
Grants and funding
LinkOut - more resources
Full Text Sources
Research Materials
Miscellaneous

