Integrating Enhanced HIV Pre-exposure Prophylaxis Into a Sexually Transmitted Infection Clinic in Lilongwe: Protocol for a Prospective Cohort Study
- PMID: 36469400
- PMCID: PMC9764156
- DOI: 10.2196/37395
Integrating Enhanced HIV Pre-exposure Prophylaxis Into a Sexually Transmitted Infection Clinic in Lilongwe: Protocol for a Prospective Cohort Study
Abstract
Background: Pre-exposure prophylaxis (PrEP) reduces HIV acquisition risk by >90% and is a critical lever to reduce HIV incidence. Identifying individuals most likely to benefit from PrEP and retaining them on PrEP throughout HIV risk is critical to realize PrEP's prevention potential. Individuals with sexually transmitted infections (STIs) are an obvious priority PrEP population, but there are no data from sub-Saharan Africa (SSA) confirming the effectiveness of integrating PrEP into STI clinics. Assisted partner notification may further enhance STI clinic-based PrEP programming by recruiting PrEP users from the pool of named sexual partners of individuals presenting with an incident STI. However, the acceptability, feasibility, and effectiveness of these integrated and enhanced strategies are unknown.
Objective: This study aims to describe the implementation outcomes of acceptability, feasibility, and effectiveness (regarding PrEP uptake and persistence) of integrating an enhanced PrEP implementation strategy into an STI clinic in Malawi.
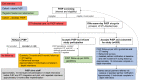
Methods: The enhanced PrEP STI study is a prospective cohort study enrolling patients who are eligible for PrEP (aged ≥15 years) who are seeking STI services at a Lilongwe-based STI clinic. Data collection relies on a combination of in-depth interviews, patient and clinic staff surveys, and clinic record review. All enrolled PrEP users will be screened for acute HIV infection and receive quarterly testing for Neisseria gonorrhea, Chlamydia trachomatis, and syphilis. Participants will be asked to name recent sexual partners for assisted notification; returning partners will be screened for PrEP eligibility and, if interested, enrolled into the cohort of PrEP initiators. We will also enroll patients who are eligible for PrEP but choose not to initiate it, from the STI clinic. Patient participants will be followed for 6 months; we will assess self-reported PrEP use, PrEP refills, sexual behaviors, perceived HIV risk, and incident STIs. Clinic staff participants will be interviewed at baseline and at approximately 6 months and will complete surveys examining the perceived acceptability and feasibility of the integrated and enhanced PrEP strategy.
Results: Enrollment began in March 2022 and is projected to continue until February 2023, with patient participant follow-up through August 2023. The results of this study are expected to be reported in 2024.
Conclusions: This study will generate important evidence regarding the potential integration of PrEP services into STI clinics in SSA and preliminary data regarding the effectiveness of an enhanced intervention that includes assisted partner notification as a strategy to identify potential PrEP users. Furthermore, this trial will provide some of the first insights into STI incidence among PrEP users recruited from an STI clinic in SSA-critical data to inform the use of etiologic STI testing where syndromic management is the current standard. These findings will help to design future PrEP implementation strategies in SSA.
Trial registration: ClinicalTrials.gov NCT05307991; https://clinicaltrials.gov/ct2/show/NCT05307991.
International registered report identifier (irrid): DERR1-10.2196/37395.
Keywords: PrEP; STI; partner notification; pre-exposure prophylaxis; sexually transmitted infections; sub-Saharan Africa.
©Sarah E Rutstein, Mitch Matoga, Jane S Chen, Esther Mathiya, Beatrice Ndalama, Naomi Nyirenda, Naomi Bonongwe, Shyreen Chithambo, Maganizo Chagomerana, Gerald Tegha, Mina C Hosseinipour, Michael E Herce, Edward Jere, Robert G Krysiak, Irving F Hoffman. Originally published in JMIR Research Protocols (https://www.researchprotocols.org), 05.12.2022.
Conflict of interest statement
Conflicts of Interest: None declared.
Figures
References
-
- Grant RM, Lama JR, Anderson PL, McMahan V, Liu AY, Vargas L, Goicochea P, Casapía M, Guanira-Carranza JV, Ramirez-Cardich ME, Montoya-Herrera O, Fernández T, Veloso VG, Buchbinder SP, Chariyalertsak S, Schechter M, Bekker LG, Mayer KH, Kallás EG, Amico KR, Mulligan K, Bushman LR, Hance RJ, Ganoza C, Defechereux P, Postle B, Wang F, McConnell JJ, Zheng JH, Lee J, Rooney JF, Jaffe HS, Martinez AI, Burns DN, Glidden DV, iPrEx Study Team Preexposure chemoprophylaxis for HIV prevention in men who have sex with men. N Engl J Med. 2010 Dec 30;363(27):2587–99. doi: 10.1056/NEJMoa1011205. https://europepmc.org/abstract/MED/21091279 - DOI - PMC - PubMed
-
- McCormack S, Dunn DT, Desai M, Dolling DI, Gafos M, Gilson R, Sullivan AK, Clarke A, Reeves I, Schembri G, Mackie N, Bowman C, Lacey CJ, Apea V, Brady M, Fox J, Taylor S, Antonucci S, Khoo SH, Rooney J, Nardone A, Fisher M, McOwan A, Phillips AN, Johnson AM, Gazzard B, Gill ON. Pre-exposure prophylaxis to prevent the acquisition of HIV-1 infection (PROUD): effectiveness results from the pilot phase of a pragmatic open-label randomised trial. Lancet. 2016 Jan 02;387(10013):53–60. doi: 10.1016/S0140-6736(15)00056-2. https://linkinghub.elsevier.com/retrieve/pii/S0140-6736(15)00056-2 S0140-6736(15)00056-2 - DOI - PMC - PubMed
-
- Choopanya K, Martin M, Suntharasamai P, Sangkum U, Mock PA, Leethochawalit M, Chiamwongpaet S, Kitisin P, Natrujirote P, Kittimunkong S, Chuachoowong R, Gvetadze RJ, McNicholl JM, Paxton LA, Curlin ME, Hendrix CW, Vanichseni S, Bangkok Tenofovir Study Group Antiretroviral prophylaxis for HIV infection in injecting drug users in Bangkok, Thailand (the Bangkok Tenofovir Study): a randomised, double-blind, placebo-controlled phase 3 trial. Lancet. 2013 Jun 15;381(9883):2083–90. doi: 10.1016/S0140-6736(13)61127-7.S0140-6736(13)61127-7 - DOI - PubMed
-
- Baeten JM, Donnell D, Ndase P, Mugo NR, Campbell JD, Wangisi J, Tappero JW, Bukusi EA, Cohen CR, Katabira E, Ronald A, Tumwesigye E, Were E, Fife KH, Kiarie J, Farquhar C, John-Stewart G, Kakia A, Odoyo J, Mucunguzi A, Nakku-Joloba E, Twesigye R, Ngure K, Apaka C, Tamooh H, Gabona F, Mujugira A, Panteleeff D, Thomas KK, Kidoguchi L, Krows M, Revall J, Morrison S, Haugen H, Emmanuel-Ogier M, Ondrejcek L, Coombs RW, Frenkel L, Hendrix C, Bumpus NN, Bangsberg D, Haberer JE, Stevens WS, Lingappa JR, Celum C, Partners PrEP Study Team Antiretroviral prophylaxis for HIV prevention in heterosexual men and women. N Engl J Med. 2012 Aug 02;367(5):399–410. doi: 10.1056/NEJMoa1108524. https://europepmc.org/abstract/MED/22784037 - DOI - PMC - PubMed
-
- Thigpen MC, Kebaabetswe PM, Paxton LA, Smith DK, Rose CE, Segolodi TM, Henderson FL, Pathak SR, Soud FA, Chillag KL, Mutanhaurwa R, Chirwa LI, Kasonde M, Abebe D, Buliva E, Gvetadze RJ, Johnson S, Sukalac T, Thomas VT, Hart C, Johnson JA, Malotte CK, Hendrix CW, Brooks JT, TDF2 Study Group Antiretroviral preexposure prophylaxis for heterosexual HIV transmission in Botswana. N Engl J Med. 2012 Aug 02;367(5):423–34. doi: 10.1056/NEJMoa1110711. - DOI - PubMed
Associated data
LinkOut - more resources
Full Text Sources
Medical
Research Materials
Miscellaneous