Cementation in total hip arthroplasty: history, principles, and technique
- PMID: 36475555
- PMCID: PMC9780613
- DOI: 10.1530/EOR-22-0002
Cementation in total hip arthroplasty: history, principles, and technique
Abstract
Total hip arthroplasty (THA) is a remarkably successful operation that has grown rapidly its utilization. Early modern THA constructs as developed by Sir John Charnley featured cemented femoral stems and acetabular components. The technique of cementing components for THA has evolved over time. Modern acetabular preparation requires exposure of the subchondral bone with appropriate cement penetration into the trabecular bone, whereas femoral preparation requires cleaning of the canal, cement restrictor placement, retrograde filling, and pressurization of the cement. When used appropriately, these techniques result in excellent long-term survivorship of implants and are also widely considered to be the ideal method of fixation for hip fractures. The purpose of this article to review the history, properties, techniques, and outcomes of bone cement utilization in THA.
Keywords: arthroplasty; bone cement; surgical technique; total hip replacement.
Figures
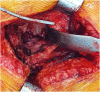
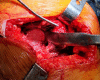
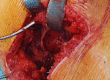

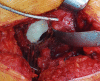



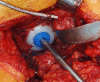
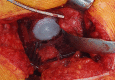








References
-
- Coventry MB.Foreward. Hip Arthroplasty. New York: Churchill Livingstone; 1991.
-
- Halawa M, Lee AJ, Ling RS, Vangala SS. The shear strength of trabecular bone from the femur, and some factors affecting the shear strength of the cement-bone interface. Archives of Orthopaedic and Traumatic Surgery. Archiv Fur Orthopadische und Unfall-Chirurgie 19789219–30. (10.1007/BF00381636) - DOI - PubMed
LinkOut - more resources
Full Text Sources

