CNS-peripheral immune interactions in hemorrhagic stroke
- PMID: 36476130
- PMCID: PMC9903219
- DOI: 10.1177/0271678X221145089
CNS-peripheral immune interactions in hemorrhagic stroke
Abstract
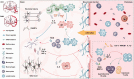
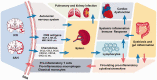
Stroke is a sudden and rapidly progressing ischemic or hemorrhagic cerebrovascular disease. When stroke damages the brain, the immune system becomes hyperactive, leading to systemic inflammatory response and immunomodulatory disorders, which could significantly impact brain damage, recovery, and prognosis of stroke. Emerging researches suggest that ischemic stroke-induced spleen contraction could activate a peripheral immune response, which may further aggravate brain injury. This review focuses on hemorrhagic strokes including intracerebral hemorrhage (ICH) and subarachnoid hemorrhage (SAH) and discusses the central nervous system-peripheral immune interactions after hemorrhagic stroke induction. First, inflammatory progression after ICH and SAH is investigated. As a part of this review, we summarize the various kinds of inflammatory cell infiltration to aggravate brain injury after blood-brain barrier interruption induced by hemorrhagic stroke. Then, we explore hemorrhagic stroke-induced systemic inflammatory response syndrome (SIRS) and discuss the interactions of CNS and peripheral inflammatory response. In addition, potential targets related to inflammatory response for ICH and SAH are discussed in this review, which may lead to novel therapeutic strategies for hemorrhagic stroke.
Keywords: Systemic inflammation; immune dysregulation; intracerebral hemorrhage; stroke; subarachnoid hemorrhage.
Conflict of interest statement
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Figures
Similar articles
-
Systemic inflammation in hemorrhagic strokes - A novel neurological sign and therapeutic target?J Cereb Blood Flow Metab. 2019 Jun;39(6):959-988. doi: 10.1177/0271678X19841443. Epub 2019 Apr 8. J Cereb Blood Flow Metab. 2019. PMID: 30961425 Free PMC article. Review.
-
Role of Inflammatory Processes in Hemorrhagic Stroke.Stroke. 2023 Feb;54(2):605-619. doi: 10.1161/STROKEAHA.122.037155. Epub 2023 Jan 5. Stroke. 2023. PMID: 36601948 Review.
-
A Therapeutic Target of Cerebral Hemorrhagic Stroke: Matrix Metalloproteinase- 9.Curr Drug Targets. 2017;18(12):1358-1366. doi: 10.2174/1389450118666170427151657. Curr Drug Targets. 2017. PMID: 28460607 Review.
-
Neuroinflammation in Acute Ischemic and Hemorrhagic Stroke.Curr Neurol Neurosci Rep. 2023 Aug;23(8):407-431. doi: 10.1007/s11910-023-01282-2. Epub 2023 Jul 3. Curr Neurol Neurosci Rep. 2023. PMID: 37395873 Free PMC article. Review.
-
T-Lymphocyte Interactions with the Neurovascular Unit: Implications in Intracerebral Hemorrhage.Cells. 2022 Jun 24;11(13):2011. doi: 10.3390/cells11132011. Cells. 2022. PMID: 35805099 Free PMC article. Review.
Cited by
-
Systematic Insights into the Relationship between the Microbiota-Gut-Brain Axis and Stroke with the Focus on Tryptophan Metabolism.Metabolites. 2024 Jul 24;14(8):399. doi: 10.3390/metabo14080399. Metabolites. 2024. PMID: 39195495 Free PMC article. Review.
-
Single-cell sequencing reveals intracranial microvasculature-derived CXCL12 promotes CD8+ T-cell infiltration and blood-brain barrier dysfunction after subarachnoid hemorrhage in mice.J Neuroinflammation. 2025 Apr 23;22(1):116. doi: 10.1186/s12974-025-03444-0. J Neuroinflammation. 2025. PMID: 40270006 Free PMC article.
-
Development of a Clinical and Laboratory-Based Predictive Nomogram Model for Unfavorable Functional Outcomes Among Patients Who Undergo Interventions for Aneurysmal Subarachnoid Hemorrhage.J Clin Med. 2025 Feb 21;14(5):1443. doi: 10.3390/jcm14051443. J Clin Med. 2025. PMID: 40094914 Free PMC article.
-
The role of ACSL4 in stroke: mechanisms and potential therapeutic target.Mol Cell Biochem. 2025 Apr;480(4):2223-2246. doi: 10.1007/s11010-024-05150-6. Epub 2024 Nov 4. Mol Cell Biochem. 2025. PMID: 39496916 Free PMC article. Review.
-
Single-cell RNA sequencing reveals the evolution of the immune landscape during perihematomal edema progression after intracerebral hemorrhage.J Neuroinflammation. 2024 May 28;21(1):140. doi: 10.1186/s12974-024-03113-8. J Neuroinflammation. 2024. PMID: 38807233 Free PMC article.
References
-
- Kleindorfer DO, Towfighi A, Chaturvedi S, et al.. 2021 Guideline for the prevention of stroke in patients with stroke and transient ischemic attack: a guideline from the American heart association/American stroke association. Stroke 2021; 52: e364–e467. - PubMed
-
- Montano A, Hanley DF, Hemphill JC, et al.. Hemorrhagic stroke. Handb Clin Neurol 2021; 176: 229–248. - PubMed
Publication types
MeSH terms
LinkOut - more resources
Full Text Sources
Medical
Research Materials

