Counter-regulatory renin-angiotensin system in hypertension: Review and update in the era of COVID-19 pandemic
- PMID: 36481346
- PMCID: PMC9721294
- DOI: 10.1016/j.bcp.2022.115370
Counter-regulatory renin-angiotensin system in hypertension: Review and update in the era of COVID-19 pandemic
Abstract
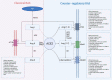
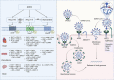
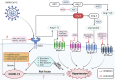
Cardiovascular disease is the major cause of mortality and disability, with hypertension being the most prevalent risk factor. Excessive activation of the renin-angiotensin system (RAS) under pathological conditions, leading to vascular remodeling and inflammation, is closely related to cardiovascular dysfunction. The counter-regulatory axis of the RAS consists of angiotensin-converting enzyme 2 (ACE2), angiotensin (1-7), angiotensin (1-9), alamandine, proto-oncogene Mas receptor, angiotensin II type-2 receptor and Mas-related G protein-coupled receptor member D. Each of these components has been shown to counteract the effects of the overactivated RAS. In this review, we summarize the latest insights into the complexity and interplay of the counter-regulatory RAS axis in hypertension, highlight the pathophysiological functions of ACE2, a multifunctional molecule linking hypertension and COVID-19, and discuss the function and therapeutic potential of targeting this counter-regulatory RAS axis to prevent and treat hypertension in the context of the current COVID-19 pandemic.
Keywords: ACE2; COVID-19; Counter-regulatory renin-angiotensin system; Hypertension.
Copyright © 2022 Elsevier Inc. All rights reserved.
Conflict of interest statement
Declaration of Competing Interest The authors declare that they have no known competing financial interests or personal relationships that could have appeared to influence the work reported in this paper.
Figures

References
-
- Kearney P.M., Whelton M., Reynolds K., Muntner P., Whelton P.K., He J. Global burden of hypertension: analysis of worldwide data. Lancet. 2005;365(9455):217–223. - PubMed
-
- Paul M., Poyan Mehr A., Kreutz R. Physiology of local renin-angiotensin systems. Physiol. Rev. 2006;86(3):747–803. - PubMed
-
- Basso N., Terragno N.A. History about the discovery of the renin-angiotensin system. Hypertension. 2001;38(6):1246–1249. - PubMed
-
- Mehta P.K., Griendling K.K. Angiotensin II cell signaling: physiological and pathological effects in the cardiovascular system. Am. J. Physiol. Cell Physiol. 2007;292(1):C82–C97. - PubMed
-
- Donoghue M., Hsieh F., Baronas E., Godbout K., Gosselin M., Stagliano N., Donovan M., Woolf B., Robison K., Jeyaseelan R., Breitbart R.E., Acton S. A novel angiotensin-converting enzyme-related carboxypeptidase (ACE2) converts angiotensin I to angiotensin 1–9. Circ. Res. 2000;87(5):E1–E9. - PubMed
Publication types
MeSH terms
Substances
LinkOut - more resources
Full Text Sources
Medical
Molecular Biology Databases

