MRI-Derived Apparent Diffusion Coefficient of Peri-Prostatic Adipose Tissue Is a Potential Determinant of Prostate Cancer Aggressiveness in Preoperative Setting: A Preliminary Report
- PMID: 36498069
- PMCID: PMC9736448
- DOI: 10.3390/ijerph192315996
MRI-Derived Apparent Diffusion Coefficient of Peri-Prostatic Adipose Tissue Is a Potential Determinant of Prostate Cancer Aggressiveness in Preoperative Setting: A Preliminary Report
Abstract
Background: The aim of this study was to test the association between periprostatic adipose tissue (PPAT)—apparent diffusion coefficient (ADC) value recorded at multiparametric magnetic resonance imaging (mpMRI) and determinants of prostate cancer (PCa) aggressiveness in the preoperative setting. Methods: Data from 219 consecutive patients undergoing prostate biopsy (PBx) for suspicion of PCa, between January 2020 and June 2022, at our institution were retrospectively evaluated. Only patients who had mpMRI performed before PBx were included. The distribution of demographics and clinical features among PPAT-ADC values up to vs. above the median was studied using both parametric and non-parametric tests, according to variables. Linear and logistic regression models tested the association between PPAT-ADC values and determinants of PCa aggressiveness and the presence of intermediate-high risk PCa, respectively. Results: Of 132 included patients, 76 (58%) had PCa. Median PPAT-ADC was 876 (interquartile range: 654 − 1112) × 10−6 mm2/s. Patients with PPAT-ADC up to the median had a higher rate of PIRADS (Prostate Imaging—Reporting and Data System) 5 lesions (41% vs. 23%, p = 0.032), a higher percentage of PBx positive cores (25% vs. 6%, p = 0.049) and more frequently harbored ISUP (International Society of Urological Pathology) > 1 PCa (50% vs. 28%, p = 0.048). At univariable linear regression analyses, prostate-specific antigen (PSA), PSA density, PIRADS 5, and percentage of PBx positive cores were associated with lower PPAT-ADC values. PPAT-ADC up to the median was an independent predictor for intermediate-high risk PCa (odds ratio: 3.24, 95%CI: 1.17−9.46, p = 0.026) after adjustment for age and body mass index. Conclusions: Lower PPAT-ADC values may be associated with higher biopsy ISUP grade group PCa and a higher percentage of PBx-positive cores. Higher-level studies are needed to confirm these preliminary results.
Keywords: ADC; MRI; periprostatic adipose tissue; prostate biopsy; prostate cancer.
Conflict of interest statement
The authors declare no conflict of interest.
Figures
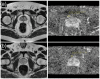
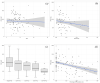
References
-
- Mottet N., van den Bergh R.C., Briers E., Van den Broeck T., Cumberbatch M.G., De Santis M., Fanti S., Fossati N., Gandaglia G., Gillessen S. EAU-EANM-ESTRO-ESUR-SIOG guidelines on prostate cancer—2020 update. Part 1: Screening, diagnosis, and local treatment with curative intent. Eur. Urol. 2021;79:243–262. doi: 10.1016/j.eururo.2020.09.042. - DOI - PubMed
-
- Mottet N., Bellmunt J., Bolla M., Briers E., Cumberbatch M.G., De Santis M., Fossati N., Gross T., Henry A.M., Joniau S. EAU-ESTRO-SIOG guidelines on prostate cancer. Part 1: Screening, diagnosis, and local treatment with curative intent. Eur. Urol. 2017;71:618–629. doi: 10.1016/j.eururo.2016.08.003. - DOI - PubMed
MeSH terms
Supplementary concepts
LinkOut - more resources
Full Text Sources
Medical
Research Materials
Miscellaneous

