The Role of Ketogenic Diet in the Treatment of Neurological Diseases
- PMID: 36501033
- PMCID: PMC9739023
- DOI: 10.3390/nu14235003
The Role of Ketogenic Diet in the Treatment of Neurological Diseases
Abstract
Over a hundred years of study on the favourable effect of ketogenic diets in the treatment of epilepsy have contributed to a long-lasting discussion on its potential influence on other neurological diseases. A significant increase in the number of scientific studies in that field has been currently observed. The aim of this paper is a widespread, thorough analysis of the available scientific evidence in respect of the role of the ketogenic diet in the therapy of neurological diseases such as: epilepsy, Alzheimer's disease (AD), Parkinson's disease (PD), multiple sclerosis (MS) and migraine. A wide range of the mechanisms of action of the ketogenic diet has been demonstrated in neurological diseases, including, among other effects, its influence on the reduction in inflammatory conditions and the amount of reactive oxygen species (ROS), the restoration of the myelin sheath of the neurons, the formation and regeneration of mitochondria, neuronal metabolism, the provision of an alternative source of energy for neurons (ketone bodies), the reduction in glucose and insulin concentrations, the reduction in amyloid plaques, the induction of autophagy, the alleviation of microglia activation, the reduction in excessive neuronal activation, the modulation of intestinal microbiota, the expression of genes, dopamine production and the increase in glutamine conversion into GABA. The studies discussed (including randomised controlled studies), conducted in neurological patients, have stressed the effectiveness of the ketogenic diet in the treatment of epilepsy and have demonstrated its promising therapeutic potential in Alzheimer's disease (AD), Parkinson's disease (PD), multiple sclerosis (MS) and migraine. A frequent advantage of the diet was demonstrated over non-ketogenic diets (in the control groups) in the therapy of neurological diseases, with simultaneous safety and feasibility when conducting the nutritional model.
Keywords: Alzheimer’s disease (AD); Parkinson’s disease (PD); anti-inflammatory; brain; epilepsy; high fat; inflammatory; ketogenic; ketogenic diet; ketone bodies; low carb; migraine; multiple sclerosis (MS); neuroinflammation; neurological diseases; neurone; neuroplasticity; neurotransmitters; nutrition; prevention; treatment.
Conflict of interest statement
The authors declare no conflict of interest.
Figures
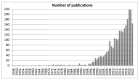

References
-
- Taquet M., Sillett R., Zhu L., Mendel J., Camplisson I., Dercon Q., Harrison P.J. Neurological and psychiatric risk trajectories after SARS-CoV-2 infection: An analysis of 2-year retrospective cohort studies including 1284437 patients. Lancet Psychiatry. 2022;9:815–827. doi: 10.1016/S2215-0366(22)00260-7. - DOI - PMC - PubMed
Publication types
MeSH terms
LinkOut - more resources
Full Text Sources
Medical

