Virtual Planning and 3D Printing in the Management of Acute Orbital Fractures and Post-Traumatic Deformities
- PMID: 36506274
- PMCID: PMC9729060
- DOI: 10.1055/s-0042-1754387
Virtual Planning and 3D Printing in the Management of Acute Orbital Fractures and Post-Traumatic Deformities
Abstract
Virtual surgical planning (VSP) and three-dimensional (3D) printing have advanced surgical reconstruction of orbital defects. Individualized 3D models of patients' orbital bony and soft tissues provide the surgeon with corrected orbital volume based on normalized anatomy, precise location of critical structures, and when needed a better visualization of the defect or altered anatomy that are paramount in preoperative planning. The use of 3D models preoperatively allows surgeons to improve the accuracy and safety of reconstruction, reduces intraoperative time, and most importantly lowers the rate of common postoperative complications, including over- or undercontouring of plates, orbital implant malposition, enophthalmos, and hypoglobus. As 3D printers and materials become more accessible and cheaper, the utility of printing patient-specific implants becomes more feasible. This article summarizes the traditional surgical management of orbital fractures and reviews advances in VSP and 3D printing in this field. It also discusses the use of in-house (point-of-care) VSP and 3D printing to further advance care of acute orbital trauma and posttraumatic deformities.
Keywords: orbital fracture; orbital reconstruction; point-of-care; three-dimensional printing; virtual surgical planning.
Thieme. All rights reserved.
Conflict of interest statement
Conflict of Interest None declared.
Figures


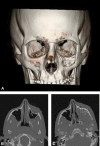



References
-
- Shui W, Zhou M, Chen S. The production of digital and printed resources from multiple modalities using visualization and three-dimensional printing techniques. Int J CARS. 2017;12(01):13–23. - PubMed
-
- Sharaf B, Kuruoglu D, Cantwell S R, Alexander A E, Dickens H J, Morris J M. EPPOCRATIS: expedited preoperative point-of-care reduction of fractures to normalized anatomy and three-dimensional printing to improve surgical outcomes. Plast Reconstr Surg. 2022;149(03):695–699. - PubMed
-
- Holmes S. Primary orbital fracture repair. Atlas Oral Maxillofac Surg Clin North Am. 2021;29(01):51–77. - PubMed
Publication types
LinkOut - more resources
Full Text Sources
Research Materials

