Vascular contributions to Alzheimer's disease
- PMID: 36529160
- PMCID: PMC10481451
- DOI: 10.1016/j.trsl.2022.12.003
Vascular contributions to Alzheimer's disease
Abstract
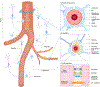
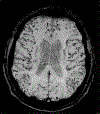
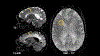
Alzheimer's disease (AD) is the most common cause of dementia and is characterized by progressive neurodegeneration and cognitive decline. Understanding the pathophysiology underlying AD is paramount for the management of individuals at risk of and suffering from AD. The vascular hypothesis stipulates a relationship between cardiovascular disease and AD-related changes although the nature of this relationship remains unknown. In this review, we discuss several potential pathological pathways of vascular involvement in AD that have been described including dysregulation of neurovascular coupling, disruption of the blood brain barrier, and reduced clearance of metabolite waste such as beta-amyloid, a toxic peptide considered the hallmark of AD. We will also discuss the two-hit hypothesis which proposes a 2-step positive feedback loop in which microvascular insults precede the accumulation of Aß and are thought to be at the origin of the disease development. At neuroimaging, signs of vascular dysfunction such as chronic cerebral hypoperfusion have been demonstrated, appearing early in AD, even before cognitive decline and alteration of traditional biomarkers. Cerebral small vessel disease such as cerebral amyloid angiopathy, characterized by the aggregation of Aß in the vessel wall, is highly prevalent in vascular dementia and AD patients. Current data is unclear whether cardiovascular disease causes, precipitates, amplifies, precedes, or simply coincides with AD. Targeted imaging tools to quantitatively evaluate the intracranial vasculature and longitudinal studies in individuals at risk for or in the early stages of the AD continuum could be critical in disentangling this complex relationship between vascular disease and AD.
Copyright © 2022. Published by Elsevier Inc.
Figures




References
-
- 2021 Alzheimer’s disease facts and figures. Alzheimers Dement. 2021;17:327–406. - PubMed
-
- Gauthier S, Rosa-Neto P, Morais J, Webster C. World Alzheimer Report 2021: Journey through the diagnosis of dementia. London, England: Alzheimer’s Disease International; 2021.
-
- Kozlov S, Afonin A, Evsyukov I, Bondarenko A. Alzheimer’s disease: as it was in the beginning. Rev Neurosci. 2017;28:825–43. - PubMed
-
- Makin S. The amyloid hypothesis on trial. Nature. 2018;559:S4–s7. - PubMed
Publication types
MeSH terms
Grants and funding
LinkOut - more resources
Full Text Sources
Medical
Miscellaneous

