Bacterial and fungal coinfections among patients with COVID-19 in Zanjan, Northwest of Iran; a single-center observational with meta-analysis of the literature
- PMID: 36531818
- PMCID: PMC9723436
- DOI: 10.18502/ijm.v14i5.10955
Bacterial and fungal coinfections among patients with COVID-19 in Zanjan, Northwest of Iran; a single-center observational with meta-analysis of the literature
Abstract
Background and objectives: There is a poor understanding about the prevalence and characteristics of secondary bacterial and fungal infections among Coronavirus diseases 2019 (COVID-19) superinfection in hospitalized patients.
Materials and methods: Four hundred COVID-19-proven patients were enrolled in this study. Nasal swabs for molecular assay (Real-time PCR) and sputum samples for further microbiological assays were collected. Following a broad-spectrum search, a meta-analysis was performed using StatsDirect software (version 2.7.9) according to the DerSimonian and Laird method applying the random-effects models.
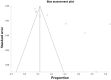
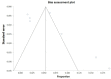
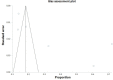
Results: Streptococcus spp. (21.5%) and Staphylococcus spp. (16.7%) had the highest prevalence of bacterial coinfection among the COVID-19 patients, while Acinetobacter spp. had the lowest prevalence (4.2%). Among fungal coinfections, Candida albicans was the most prevalent (6.7%), and Aspergillus spp. was the lowest (2%). Males, elderly patients, patients with a history of underlying diseases and drug use, patients who showed acute clinical symptoms, and patients with a prolonged hospital stay had a higher incidence of secondary infections (P-value <0.05). The pooled prevalence for bacterial and fungal coinfections was 33.52% (95% CI: 18.12 to 50.98; I2: 99.4%; P-value: <0.0001).
Conclusion: We suggest designing additional research with a larger target population and diagnostic molecular analyses to depict a more realistic view of the coinfection status.
Keywords: COVID-19; Nosocomial infection; Secondary infection.
Copyright © 2022 The Authors. Published by Tehran University of Medical Sciences.
Figures



Similar articles
-
The Prevalence of Bacterial and Fungal Coinfections among Critically Ill COVID-19 Patients in the ICU in Jordan.Int J Microbiol. 2022 Oct 31;2022:9992881. doi: 10.1155/2022/9992881. eCollection 2022. Int J Microbiol. 2022. PMID: 36353524 Free PMC article.
-
Worldwide prevalence of fungal coinfections among COVID-19 patients: a comprehensive systematic review and meta-analysis.Osong Public Health Res Perspect. 2022 Feb;13(1):15-23. doi: 10.24171/j.phrp.2021.0293. Epub 2022 Feb 8. Osong Public Health Res Perspect. 2022. PMID: 35255675 Free PMC article.
-
Fungal and bacterial coinfections increase mortality of severely ill COVID-19 patients.J Hosp Infect. 2021 Jul;113:145-154. doi: 10.1016/j.jhin.2021.04.001. Epub 2021 Apr 20. J Hosp Infect. 2021. PMID: 33852950 Free PMC article.
-
State-of-the-art review of secondary pulmonary infections in patients with COVID-19 pneumonia.Infection. 2021 Aug;49(4):591-605. doi: 10.1007/s15010-021-01602-z. Epub 2021 Mar 11. Infection. 2021. PMID: 33709380 Free PMC article. Review.
-
Bacterial Coinfections in Coronavirus Disease 2019.Trends Microbiol. 2021 Oct;29(10):930-941. doi: 10.1016/j.tim.2021.03.018. Epub 2021 Apr 8. Trends Microbiol. 2021. PMID: 33934980 Free PMC article. Review.
References
-
- Russell CD, Fairfield CJ, Drake TM, Turtle L, Seaton RA, Wootton DG, et al. . Co-infections, secondary infections, and antimicrobial use in patients hospitalised with COVID-19 during the first pandemic wave from the ISARIC WHO CCP-UK study: a multicentre, prospective cohort study. Lancet Microbe 2021; 2(8): e354–e365. - PMC - PubMed
LinkOut - more resources
Full Text Sources
Miscellaneous
