Evaluation and Treatment of Vulvodynia: State of the Science
- PMID: 36533637
- PMCID: PMC10107324
- DOI: 10.1111/jmwh.13456
Evaluation and Treatment of Vulvodynia: State of the Science
Abstract
Vulvodynia affects 7% of American women, yet clinicians often lack awareness of its presentation. It is underdiagnosed and often misdiagnosed as vaginitis. The etiology of vulvodynia remains unknown, making it difficult to identify or develop effective treatment methods. The purpose of this article is to (1) review the presentation and evaluation of vulvodynia, (2) review the research on vulvodynia treatments, and (3) aid the clinician in the selection of vulvodynia treatment methods. The level of evidence to support vulvodynia treatment varies from case series to randomized controlled trials (RCTs). Oral desipramine with 5% lidocaine cream, intravaginal diazepam tablets with intravaginal transcutaneous electric nerve stimulation (TENS), botulinum toxin type A 50 units, enoxaparin sodium subcutaneous injections, intravaginal TENS (as a single therapy), multimodal physical therapy, overnight 5% lidocaine ointment, and acupuncture had the highest level of evidence with at least one RCT or comparative effectiveness trial. Pre to posttest reduction in vulvar pain and/or dyspareunia in non-RCT studies included studies of gabapentin cream, amitriptyline cream, amitriptyline with baclofen cream, up to 6 weeks' oral itraconazole therapy, multimodal physical therapy, vaginal dilators, electromyography biofeedback, hypnotherapy, cognitive behavioral therapy, cold knife vestibulectomy, and laser therapy. There is a lack of rigorous RCTs with large sample sizes for the treatment of vulvodynia, rendering it difficult to determine efficacy of most treatment methods. Clinicians will be guided in the selection of best treatments for vulvodynia that have the highest level of evidence and are least invasive.
Keywords: pain management; patient education; pharmacology.
© 2022 The Authors. Journal of Midwifery & Women's Health published by Wiley Periodicals LLC on behalf of American College of Nurse Midwives (ACNM).
Conflict of interest statement
The authors have no conflicts of interest to disclose.
Figures
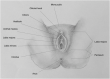

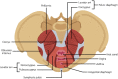

References
-
- Bornstein J, Goldstein AT, Stockdale CK, et al. 2015 ISSVD, ISSWSH and IPPS consensus terminology and classification of persistent vulvar pain and vulvodynia. Obstet Gynecol. 2016;127(4):745‐751. - PubMed
-
- Brotto LA, Yong P, Smith KB, Sadownik LA. Impact of a multidisciplinary vulvodynia program on sexual functioning and dyspareunia. J Sex Med. 2015;12(1):238‐247. - PubMed
-
- Basson R. The recurrent pain and sexual sequelae of provoked vestibulodynia: a perpetuating cycle. J Sex Med. 2012;9(8):2077‐2092. - PubMed
-
- Masheb RM, Brondolo E, Kerns RD. A multidimensional, case‐control study of women with self‐identified chronic vulvar pain. Pain Med. 2002;3(3):253‐259. - PubMed
Publication types
MeSH terms
Substances
Grants and funding
LinkOut - more resources
Full Text Sources

