Next-Generation Polymyxin Class of Antibiotics: A Ray of Hope Illuminating a Dark Road
- PMID: 36551367
- PMCID: PMC9774142
- DOI: 10.3390/antibiotics11121711
Next-Generation Polymyxin Class of Antibiotics: A Ray of Hope Illuminating a Dark Road
Abstract
Although new-generation antimicrobials, in particular β-lactam/β-lactamase inhibitors, have largely replaced polymyxins in carbapenem-resistant Gram-negative bacterial infections, polymyxins are still needed for carbapanem-resistant Acinetobacter baumannii infections and in settings where novel agents are not readily available. Despite their potent in vitro activity, the clinical utility of polymyxins is significantly limited by their pharmacokinetic properties and nephrotoxicity risk. There is significant interest, therefore, in developing next-generation polymyxins with activity against colistin-resistant strains and lower toxicity than existing polymyxins. In this review, we aim to present the antibacterial activity mechanisms, in vitro and in vivo efficacy data, and toxicity profiles of new-generation polymyxins, including SPR206, MRX-8, and QPX9003, as well as the general characteristics of old polymyxins. Considering the emergence of colistin-resistant strains particularly in endemic regions, the restoration of the antimicrobial activity of polymyxins via PBT2 is also described in this review.
Keywords: MRX-8; PBT2; QPX9003; SPR206; colistin; polymyxins.
Conflict of interest statement
M.A. has received honoraria for educational activities from Pfizer, MSD, Gilead and Genentech, and research support from Pfizer and Gilead. D.L.P. reports research grants from Merck, Pfizer, and Shionogi. D.L.P. has received honoraria for advisory board membership or consultancies from the AMR Action Fund, Merck, Pfizer, Shionogi, GSK, Qpex, Spero, Entasis, VenatoRx, BioMerieux, and Accelerate. All other authors declare that they have no conflicts of interest. The authors have no other relevant affiliations or financial involvement with any organization or entity with a financial interest in or financial conflict with the subject matter or materials discussed in the manuscript apart from those disclosed.
Figures

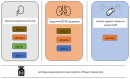
References
-
- World Health Organization . Global Antimicrobial Resistance Surveillance System (GLASS) Report: Early Implementation 2017–2018. WHO; Geneva, Switzerland: 2019. [(accessed on 13 January 2022)]. Available online: https://www.who.int/publications/i/item/9789241515061.
-
- Centers for Disease Control and Prevention . Antibiotic Resistance Threats in the United States. CDC; Atlanta, GA, USA: 2019. [(accessed on 13 January 2022)]. Available online: https://www.cdc.gov/drugresistance/pdf/threats-report/2019-ar-threats-re....
-
- Tacconelli E., Carrara E., Savoldi A., Harbarth S., Mendelson M., Monnet D.L., Pulcini C., Kahlmeter G., Kluytmans J., Carmeli Y., et al. Discovery, research, and development of new antibiotics: The WHO priority list of antibiotic-resistant bacteria and tuberculosis. Lancet Infect. Dis. 2018;18:318–327. doi: 10.1016/S1473-3099(17)30753-3. - DOI - PubMed
Publication types
LinkOut - more resources
Full Text Sources

