The Prognostic Role of True Radical Resection in Perihilar Cholangiocarcinoma after Improved Evaluation of Radial Margin Status
- PMID: 36551610
- PMCID: PMC9776927
- DOI: 10.3390/cancers14246126
The Prognostic Role of True Radical Resection in Perihilar Cholangiocarcinoma after Improved Evaluation of Radial Margin Status
Abstract
Background: The evaluation of surgical margins in resected perihilar cholangiocarcinoma (PHCC) remains a challenging issue. Both ductal (DM) and radial margin (RM) should be considered to define true radical resections (R0). Although DM status is routinely described in pathological reports, RM status is often overlooked. Therefore, the frequency of true R0 and its impact on survival might be biased.
Objective: To improve the evaluation of RM status and investigate the impact of true R0 on survival.
Methods: From 2014 to 2020, 90 patients underwent curative surgery for PHCC at Verona University Hospital, Verona, Italy. Both DM (proximal and distal biliary margin) and RM (hepatic, periductal, and vascular margin) status were evaluated by expert hepatobiliary pathologists. Patients with lymph-node metastases or positive surgical margins (R1) were candidates for adjuvant treatment. Clinicopathological and survival data were retrieved from an institutional database.
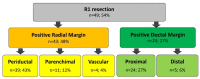
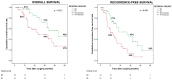
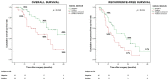
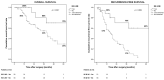
Results: True R0 were 46% (41) and overall R1 were 54% (49). RM positivity resulted in being higher than DM positivity (48% versus 27%). Overall survival was better in patients with true R0 than in patients with R1 (median survival time: 53 vs. 28 months; p = 0.016). Likewise, the best recurrence-free survival was observed in R0 compared with R1 (median survival time: 32 vs. 15 months; p = 0.006). Multivariable analysis identified residual disease status as an independent prognostic factor of both OS (p = 0.009, HR = 2.68, 95% CI = 1.27-5.63) and RFS (p = 0.009, HR = 2.14, 95% CI = 1.20-3.83).
Conclusion: Excellent survival was observed in true R0 patients. The improved evaluation of RM status is mandatory to properly stratify prognosis and select patients for adjuvant treatment.
Keywords: hilar cholangiocarcinoma; periductal margin; radial margin; residual disease; surgical margin.
Conflict of interest statement
The authors declare no conflict of interest.
Figures

Similar articles
-
Impact of Positive Radial Margin on Recurrence and Survival in Perihilar Cholangiocarcinoma.Cancers (Basel). 2022 Mar 25;14(7):1680. doi: 10.3390/cancers14071680. Cancers (Basel). 2022. PMID: 35406452 Free PMC article.
-
The impact of positive resection margin in perihilar cholangiocarcinoma, ductal margin vs radial margin.Langenbecks Arch Surg. 2024 Nov 26;409(1):359. doi: 10.1007/s00423-024-03547-x. Langenbecks Arch Surg. 2024. PMID: 39589565
-
A Study on Radial Margin Status in Resected Perihilar Cholangiocarcinoma.Ann Surg. 2021 Mar 1;273(3):572-578. doi: 10.1097/SLA.0000000000003305. Ann Surg. 2021. PMID: 30946074
-
The Relevance of Radial Margin Status in Perihilar Cholangiocarcinoma: A State-of-the-Art Narrative Review.Dig Surg. 2024;41(2):92-102. doi: 10.1159/000535995. Epub 2024 Mar 6. Dig Surg. 2024. PMID: 38447545 Review.
-
Does Intraoperative Frozen Section and Revision of Margins Lead to Improved Survival in Patients Undergoing Resection of Perihilar Cholangiocarcinoma? A Systematic Review and Meta-analysis.Ann Surg Oncol. 2022 Nov;29(12):7592-7602. doi: 10.1245/s10434-022-12041-x. Epub 2022 Jun 25. Ann Surg Oncol. 2022. PMID: 35752725
Cited by
-
Current Perspectives in Liver Transplantation for Perihilar Cholangiocarcinoma.Curr Oncol. 2023 Mar 1;30(3):2942-2953. doi: 10.3390/curroncol30030225. Curr Oncol. 2023. PMID: 36975438 Free PMC article. Review.
-
Development and validation of a machine learning-based nomogram for survival prediction of patients with hilar cholangiocarcinoma after curative-intent resection.Sci Rep. 2025 Jul 12;15(1):25220. doi: 10.1038/s41598-025-10329-y. Sci Rep. 2025. PMID: 40652016 Free PMC article.
-
Feasibility and safety of robotic radical resection for hilar cholangiocarcinoma in highly selected patients: A systematic review and meta-analysis with meta-regression.Ann Hepatobiliary Pancreat Surg. 2025 May 31;29(2):99-112. doi: 10.14701/ahbps.24-236. Epub 2025 Feb 26. Ann Hepatobiliary Pancreat Surg. 2025. PMID: 40007165 Free PMC article. Review.
References
-
- Groot Koerkamp B., Wiggers J.K., Gonen M., Doussot A., Allen P.J., Besselink M.G.H., Blumgart L.H., Busch O.R.C., D’Angelica M.I., DeMatteo R.P., et al. Survival after Resection of Perihilar Cholangiocarcinoma-Development and External Validation of a Prognostic Nomogram. Ann. Oncol. 2015;26:1930–1935. doi: 10.1093/annonc/mdv279. - DOI - PMC - PubMed
-
- Rassam F., Roos E., van Lienden K.P., van Hooft J.E., Klümpen H.J., van Tienhoven G., Bennink R.J., Engelbrecht M.R., Schoorlemmer A., Beuers U.H.W., et al. Modern Work-up and Extended Resection in Perihilar Cholangiocarcinoma: The AMC Experience. Langenbeck’s Arch. Surg. 2018;403:289–307. doi: 10.1007/s00423-018-1649-2. - DOI - PMC - PubMed
LinkOut - more resources
Full Text Sources

