Duplex and Angiographic-Assisted Evaluation of Outcomes of Endovascular Embolization after Surgical Deep Vein Arterialization for the Treatment No-Option Critical Limb Ischemia Patients
- PMID: 36552992
- PMCID: PMC9777475
- DOI: 10.3390/diagnostics12122986
Duplex and Angiographic-Assisted Evaluation of Outcomes of Endovascular Embolization after Surgical Deep Vein Arterialization for the Treatment No-Option Critical Limb Ischemia Patients
Abstract
Objective: To report early and mid-term outcomes of the arterialization of the deep venous system in no-option critical limb-threatening ischemia (CLTI) using duplex ultrasound and angiographic evaluation to improve limb perfusion.
Methods: A single-center prospective study of patients with no-option CLTI treated with hybrid surgical arterialization of the deep venous circulation and staged endovascular embolization of the venous collateral. Embolization was performed using a controlled-release spiral, within two weeks after bypass surgery. Patients were assessed for clinical status, wound healing, median transcutaneous partial pressure of O2 (TcPO2), and post-operative duplex ultrasound evaluating peak systolic velocity (PSV), end diastolic velocity (EDV), and resistance index (RI) to assess foot perfusion and bypass features. Primary endpoint analysis was primary technical success, limb salvage, patency rates, and clinical improvement. Secondary endpoints were 30-day and long-term mortality, major cardiovascular events (MACE), including myocardial infarction or stroke, and serious adverse events (SAE).
Results: Five patients with no-option CLTI were treated at our center using the hybrid deep vein arterialization technique. Clinical stage was grade 3 in one patient and grade 4 in the remaining four. Mean age was 65.8 years (range 49-76 years), and two patients were affected by Buerger's disease. Primary technical success was achieved in all patients, and all the bypasses were patent at the angiographic examination. At 30-day and at average follow-up of 9.8 months (range 2-24 months), mortality, major cardiovascular events (MACE), and serious adverse events (SAE) were not reported, with a primary patency and limb salvage rates of 100%. Three patients required minor amputation. Clinical improvement was demonstrated in all patients with granulation, resolution of rest pain, or both. Median TcPO2 values rose from 10 mm Hg (range 4-25) before the procedure to 35 (range 31-57) after surgery, and to 59 mm Hg (range 50-76) after the staged endovascular procedure.
Conclusions: In our initial experience, the arterialization of the deep venous circulation, with subsequent selective embolization of the venous escape routes from the foot, seems a feasible and effective solution for limb salvage in patients with no-option CLTI and those in the advanced wound, ischemia, and foot infection (WIfI) clinical stage.
Keywords: chronic limb-threatening ischemia; critical limb ischemia; deep vein arterialization; no-option chronic limb-threatening ischemia.
Conflict of interest statement
The authors declare no conflict of interest.
Figures
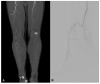



References
-
- Zhan L.X., Branco B.C., Armstrong D.G., Mills J.L., Sr. The Society for Vascular Surgery lower extremity threatened limb classification system based on Wound, Ischemia, and foot Infection (WIfI) correlates with risk of major amputation and time to wound healing. J. Vasc. Surg. 2015;61:939–944. doi: 10.1016/j.jvs.2014.11.045. - DOI - PubMed
-
- Reinecke H., Unrath M., Freisinger E., Bunzemeier H., Meyborg M., Lüders F., Gebauer K., Roeder N., Berger K., Malyar N.M. Peripheral arterial disease and critical limb ischaemia: Still poor outcomes and lack of guideline adherence. Eur. Heart J. 2015;36:932–938. doi: 10.1093/eurheartj/ehv006. - DOI - PubMed
LinkOut - more resources
Full Text Sources

