The Benign Side of the Abdominal Wall: A Pictorial Review of Non-Neoplastic Diseases
- PMID: 36553218
- PMCID: PMC9778078
- DOI: 10.3390/diagnostics12123211
The Benign Side of the Abdominal Wall: A Pictorial Review of Non-Neoplastic Diseases
Abstract
The abdominal wall is the location of a wide spectrum of pathological conditions, from benign to malignant ones. Imaging is often recommended for the evaluation of known palpable abdominal masses. However, abdominal wall pathologies are often incidentally discovered and represent a clinical and diagnostic challenge. Knowledge of the possible etiologies and complications, combined with clinical history and laboratory findings, is crucial for the correct management of these conditions. Specific imaging clues can help the radiologist narrow the differential diagnosis and distinguish between malignant and benign processes. In this pictorial review, we will focus on the non-neoplastic benign masses and processes that can be encountered on the abdominal wall on cross-sectional imaging, with a particular focus on their management. Distinctive sonographic imaging clues, compared with computed tomography (CT) and magnetic resonance (MR) findings will be highlighted, together with clinical and practical tips for reaching the diagnosis and guiding patient management, to provide a complete diagnostic guide for the radiologist.
Keywords: abdominal wall; computed tomography; diagnosis; differential; incidentalomas; magnetic resonance imaging; ultrasonography.
Conflict of interest statement
Roberto Cannella: support for attending meetings from Bracco and Bayer; co-funding by the European Union—FESR or FSE, PON Research and Innovation 2014–2020—DM 1062/2021. Other authors declare no conflict of interest.
Figures





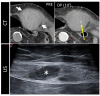
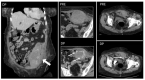

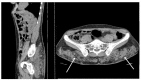
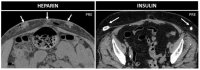


Similar articles
-
The Neoplastic Side of the Abdominal Wall: A Comprehensive Pictorial Essay of Benign and Malignant Neoplasms.Diagnostics (Basel). 2023 Jan 15;13(2):315. doi: 10.3390/diagnostics13020315. Diagnostics (Basel). 2023. PMID: 36673126 Free PMC article. Review.
-
The abdominal wall lumps and bumps: cross-sectional imaging spectrum.Can Assoc Radiol J. 2014 Feb;65(1):9-18. doi: 10.1016/j.carj.2012.02.001. Epub 2012 Aug 9. Can Assoc Radiol J. 2014. PMID: 22884230 Review.
-
Sonography of Abdominal Wall Masses and Masslike Lesions: Correlation With Computed Tomography and Magnetic Resonance Imaging.J Ultrasound Med. 2016 Jan;35(1):189-208. doi: 10.7863/ultra.15.03027. Epub 2015 Dec 11. J Ultrasound Med. 2016. PMID: 26657747
-
Benign and Suspicious Ovarian Masses-MR Imaging Criteria for Characterization: Pictorial Review.J Oncol. 2012;2012:481806. doi: 10.1155/2012/481806. Epub 2012 Mar 22. J Oncol. 2012. PMID: 22536238 Free PMC article.
-
ACR Appropriateness Criteria® Palpable Abdominal Mass-Suspected Neoplasm.J Am Coll Radiol. 2019 Nov;16(11S):S384-S391. doi: 10.1016/j.jacr.2019.05.014. J Am Coll Radiol. 2019. PMID: 31685106 Review.
Cited by
-
Role of computed tomography in imaging of endometriosis.Abdom Radiol (NY). 2025 Mar 27. doi: 10.1007/s00261-025-04907-x. Online ahead of print. Abdom Radiol (NY). 2025. PMID: 40146309 Review.
-
Gorgon sign in abdominal wall endometriosis.Abdom Radiol (NY). 2024 Jun;49(6):2158-2160. doi: 10.1007/s00261-024-04284-x. Epub 2024 Mar 16. Abdom Radiol (NY). 2024. PMID: 38492002 Review. No abstract available.
References
-
- Vanhoenacker, Filip M., Parizel P.M., Gielen J.L. Imaging of Soft Tissue Tumors. 3rd ed. Springer; Berlin/Heidelberg, Germany: 2017.
-
- van Rijswijk C.S., Geirnaerdt M.J., Hogendoorn P.C., Taminiau A.H., van Coevorden F., Zwinderman A.H., Pope T.L., Bloem J.L. Soft-tissue tumors: Value of static and dynamic gadopentetate dimeglumine-enhanced MR imaging in prediction of malignancy. Radiology. 2004;233:493–502. doi: 10.1148/radiol.2332031110. - DOI - PubMed
Publication types
LinkOut - more resources
Full Text Sources

