Ivermectin Attenuates CCl4-Induced Liver Fibrosis in Mice by Suppressing Hepatic Stellate Cell Activation
- PMID: 36555680
- PMCID: PMC9782196
- DOI: 10.3390/ijms232416043
Ivermectin Attenuates CCl4-Induced Liver Fibrosis in Mice by Suppressing Hepatic Stellate Cell Activation
Abstract
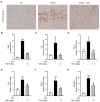
Liver fibrosis, a common liver dysfunction with high morbidity and mortality rates, is the leading cause of cirrhosis and hepatocellular carcinoma, for which there are no effective therapies. Ivermectin is an antiparasitic drug that also has been showing therapeutic actions in many other diseases, including antiviral and anticancer actions, as well as treating metabolic diseases. Herein, we evaluated the function of ivermectin in regulating liver fibrosis. Firstly, carbon tetrachloride (CCl4)-injected Balb/c mice were used to assess the antifibrosis effects of ivermectin in vivo. Further, CFSC, a rat hepatic stellate cell (HSC) line, was used to explore the function of ivermectin in HSC activation in vitro. The in vivo data showed that ivermectin administration alleviated histopathological changes, improved liver function, reduced collagen deposition, and downregulated the expression of profibrotic genes. Mechanistically, the ivermectin treatment inhibited intrahepatic macrophage accumulation and suppressed the production of proinflammatory factors. Importantly, the ivermectin administration significantly decreased the protein levels of α-smooth muscle actin (α-SMA) both in vivo and in vitro, suggesting that the antifibrotic effects of ivermectin are mainly due to the promotion of HSC deactivation. The present study demonstrates that ivermectin may be a potential therapeutic agent for the prevention of hepatic fibrosis.
Keywords: TGF-β1; hepatic stellate cells; inflammation; ivermectin; liver fibrosis.
Conflict of interest statement
The authors declare no conflict of interest.
Figures






Similar articles
-
Physalin D attenuates hepatic stellate cell activation and liver fibrosis by blocking TGF-β/Smad and YAP signaling.Phytomedicine. 2020 Nov;78:153294. doi: 10.1016/j.phymed.2020.153294. Epub 2020 Jul 28. Phytomedicine. 2020. PMID: 32771890
-
The common dietary flavonoid myricetin attenuates liver fibrosis in carbon tetrachloride treated mice.Mol Nutr Food Res. 2017 Apr;61(4). doi: 10.1002/mnfr.201600392. Epub 2017 Feb 6. Mol Nutr Food Res. 2017. PMID: 27983763
-
DCDC2 inhibits hepatic stellate cell activation and ameliorates CCl4-induced liver fibrosis by suppressing Wnt/β-catenin signaling.Sci Rep. 2024 Apr 24;14(1):9425. doi: 10.1038/s41598-024-59698-w. Sci Rep. 2024. PMID: 38658618 Free PMC article.
-
Ampelopsin attenuates carbon tetrachloride-induced mouse liver fibrosis and hepatic stellate cell activation associated with the SIRT1/TGF-β1/Smad3 and autophagy pathway.Int Immunopharmacol. 2019 Dec;77:105984. doi: 10.1016/j.intimp.2019.105984. Epub 2019 Oct 31. Int Immunopharmacol. 2019. PMID: 31677501
-
N-n-Butyl haloperidol iodide ameliorates liver fibrosis and hepatic stellate cell activation in mice.Acta Pharmacol Sin. 2022 Jan;43(1):133-145. doi: 10.1038/s41401-021-00630-7. Epub 2021 Mar 23. Acta Pharmacol Sin. 2022. PMID: 33758354 Free PMC article.
Cited by
-
Ivermectin Attenuates Methotrexate-Induced Liver Fibrosis by Reducing TGF-β and Syndecan-1 Expression.Medicina (Kaunas). 2025 Jun 4;61(6):1036. doi: 10.3390/medicina61061036. Medicina (Kaunas). 2025. PMID: 40572724 Free PMC article.
-
Research and application of medicines for treating liver fibrosis: current status and prospects.Front Pharmacol. 2025 Jul 9;16:1582258. doi: 10.3389/fphar.2025.1582258. eCollection 2025. Front Pharmacol. 2025. PMID: 40703362 Free PMC article. Review.
References
MeSH terms
Substances
Grants and funding
LinkOut - more resources
Full Text Sources

