Iatrogenic Ankle Charcot Neuropathic Arthropathy after Spinal Surgery: A Case Report and Literature Review
- PMID: 36556978
- PMCID: PMC9785748
- DOI: 10.3390/medicina58121776
Iatrogenic Ankle Charcot Neuropathic Arthropathy after Spinal Surgery: A Case Report and Literature Review
Abstract
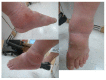
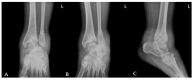
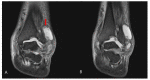
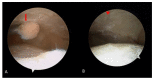
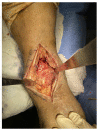
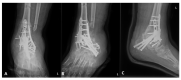
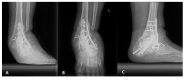
Charcot neuropathic arthropathy is a relatively rare, chronic disease that leads to joint destruction and reduced quality of life of patients. Early diagnosis of Charcot arthropathy is essential for a good outcome. However, the diagnosis is often based on the clinical course and longitudinal follow-up of patients is required. Charcot arthropathy is suspected in patients with suggestive symptoms and an underlying etiology. Failed spinal surgery is not a known cause of Charcot arthropathy. Herein we report a patient with ankle Charcot neuropathic arthropathy that developed after failed spinal surgery. A 58-year-old man presented to the emergency room due to painful swelling of the left ankle for 2 weeks that developed spontaneously. He underwent spinal surgery 8 years ago that was associated with nerve damage, which led to weakness of great toe extension and ankle dorsiflexion, and sensory loss below the knee. CT and T2-weighted sagittal MRI showed a fine erosive lesion, subluxation, sclerosis, fragmentation, and large bone defects. Based on the patient's history and radiological findings, Charcot arthropathy was diagnosed. However, the abnormal blood parameters, positive blood cultures, and severe pain despite the decreased sensation suggested a diagnosis of septic arthritis. Therefore, diagnostic arthroscopy was performed. The ankle joint exhibited continued destruction after the initial surgery. Consequently, several repeat surgeries were performed over the next 2 years. Despite the early diagnosis and treatment of Charcot arthropathy, the destruction of the ankle joint continued. Given the chronic disease course and poor prognosis of Charcot arthropathy, it is essential to consider this diagnosis in patients with neuropathy.
Keywords: ankle; charcot neuropathic arthropathy; iatrogenic charcot; spinal surgery.
Conflict of interest statement
The authors declare that they have no conflict of interest.
Figures

References
-
- Eichenholtz S.N. Charcot joints. J. Bone Jt. Surg. 1962;44:1485.
Publication types
MeSH terms
Grants and funding
LinkOut - more resources
Full Text Sources
Medical

