Penicillin allergy delabeling: Opportunities for implementation and dissemination
- PMID: 36563744
- PMCID: PMC11949300
- DOI: 10.1016/j.anai.2022.12.023
Penicillin allergy delabeling: Opportunities for implementation and dissemination
Abstract
Although existing as a safety measure to prevent iatrogenic harm, unconfirmed penicillin allergy labels have a negative impact on personal and public health. One downstream effect of unconfirmed penicillin allergy is the continued emergence and transmission of resistant bacteria and their associated health care costs. Recognizing the consequences of inaccurate penicillin allergy labels, professional and public health organizations have started promoting the adoption of proactive penicillin allergy evaluations, with the ultimate goal of removing the penicillin allergy label when the allergy is disproved, also known as penicillin allergy "delabeling." A penicillin allergy evaluation includes a comprehensive allergy history often followed by drug challenge, sometimes with preceding skin testing. Currently, penicillin allergy delabeling is largely carried out by allergy specialists in outpatient settings. Penicillin allergy delabeling is performed on inpatients, albeit rarely, often at the time of need, as a point-of-care procedure. Access to penicillin allergy evaluation services is limited. Recent studies demonstrate the feasibility of expanding penicillin allergy evaluations and delabeling to internists, pediatricians, emergency medicine physicians, infectious diseases specialists, and clinical pharmacists. However, reducing the impact of mislabeled penicillin allergy will require comprehensive efforts and new investments. In this review, we summarize the current practices of penicillin allergy delabeling and discuss expansion opportunities for penicillin allergy delabeling as quality improvement.
Copyright © 2022 American College of Allergy, Asthma & Immunology. Published by Elsevier Inc. All rights reserved.
Conflict of interest statement
Figures
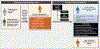
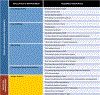


References
-
- Castells M, Khan DA, Phillips EJ. Penicillin allergy. N Engl J Med. 2019;381(24):2338–2351. - PubMed
-
- Macy E, Poon KYT. Self-reported antibiotic allergy incidence and prevalence: age and sex effects. Am J Med. 2009;122(8). 778.e1–778.e7. - PubMed
-
- Wurcel AG, Guardado R, Ortiz C, Bornmann CR, Gillis J, Huang K, et al. Low frequency of allergy referral for penicillin allergy evaluation in an urban Boston primary care setting. J Allergy Clin Immunol Glob. 2022. https://www.jaci-global.org/article/S2772-8293(22)00083-2/fulltext. Accessed January 6, 2023. - PMC - PubMed
-
- Hampton LL, DeBoy JT, Hornik CP, White MJ, Nazareth-Pidgeon KM. Association of sociodemographic factors with reported penicillin allergy in pediatric inpatients. Hosp Pediatr. 2022;12(7):625–631. - PubMed
Publication types
MeSH terms
Substances
Grants and funding
LinkOut - more resources
Full Text Sources
Medical

