Lymphangioleiomyomatosis: a metastatic lung disease
- PMID: 36571446
- PMCID: PMC9886342
- DOI: 10.1152/ajpcell.00202.2022
Lymphangioleiomyomatosis: a metastatic lung disease
Abstract
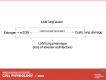
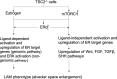
Lymphangioleiomyomatosis (LAM) is a rare disease affecting women, caused by somatic mutations in the TSC1 or TSC2 genes, and driven by estrogen. Similar to many cancers, it is metastatic, primarily to the lung. Despite its monogenetic nature, like many cancers, LAM is a heterogeneous disease. The cellular constituents of LAM are very diverse, including mesenchymal, epithelial, endothelial, and immune cells. LAM is characterized by dysregulation of many cell signaling pathways, distinct populations of LAM cells, and a rich microenvironment, in which the immune system appears to play an important role. This review delineates the heterogeneity of LAM and focuses on the metastatic features of LAM, the deregulated signaling mechanisms and the tumor microenvironment. Understanding the tumor-host interaction in LAM may provide insights into the development of new therapeutic strategies, which could be combinatorial or superlative to Sirolimus, the current U.S. Food and Drug Administration-approved treatment.
Keywords: TSC; lung; lymphangioleiomyomatosis; mTOR; rare disease.
Conflict of interest statement
No conflicts of interest, financial or otherwise, are declared by the authors.
Figures


Similar articles
-
Urokinase-type plasminogen activator (uPA) is critical for progression of tuberous sclerosis complex 2 (TSC2)-deficient tumors.J Biol Chem. 2017 Dec 15;292(50):20528-20543. doi: 10.1074/jbc.M117.799593. Epub 2017 Sep 27. J Biol Chem. 2017. PMID: 28972182 Free PMC article.
-
Rapamycin-insensitive up-regulation of adipocyte phospholipase A2 in tuberous sclerosis and lymphangioleiomyomatosis.PLoS One. 2014 Oct 27;9(10):e104809. doi: 10.1371/journal.pone.0104809. eCollection 2014. PLoS One. 2014. PMID: 25347447 Free PMC article.
-
Estrogen maintains myometrial tumors in a lymphangioleiomyomatosis model.Endocr Relat Cancer. 2016 Apr;23(4):265-80. doi: 10.1530/ERC-15-0505. Epub 2016 Feb 15. Endocr Relat Cancer. 2016. PMID: 26880751 Free PMC article.
-
Smooth muscle-like cells in pulmonary lymphangioleiomyomatosis.Proc Am Thorac Soc. 2008 Jan 1;5(1):119-26. doi: 10.1513/pats.200705-061VS. Proc Am Thorac Soc. 2008. PMID: 18094094 Free PMC article. Review.
-
Clinical and molecular insights into lymphangioleiomyomatosis.Sarcoidosis Vasc Diffuse Lung Dis. 2005 Dec;22 Suppl 1:S49-66. Sarcoidosis Vasc Diffuse Lung Dis. 2005. PMID: 16457017 Review.
Cited by
-
Identification of common genetic features and pathways involved in pulmonary lymphangioleiomyomatosis and ER-positive breast cancer.Medicine (Baltimore). 2023 Sep 29;102(39):e34810. doi: 10.1097/MD.0000000000034810. Medicine (Baltimore). 2023. PMID: 37773865 Free PMC article.
-
Beyond the Graft: Recurrence of Interstitial Lung Diseases Post Transplant.J Clin Med. 2025 Feb 8;14(4):1093. doi: 10.3390/jcm14041093. J Clin Med. 2025. PMID: 40004625 Free PMC article. Review.
-
[Incidental diagnosis of lymphangioleiomyomatosis in gynecological surgery-a case series].Pathologie (Heidelb). 2025 May;46(3):179-184. doi: 10.1007/s00292-025-01414-0. Epub 2025 Feb 7. Pathologie (Heidelb). 2025. PMID: 39918558 Free PMC article. German.
-
Lymphangioleiomyomatosis with Tuberous Sclerosis Complex-A Case Study.J Pers Med. 2023 Nov 12;13(11):1598. doi: 10.3390/jpm13111598. J Pers Med. 2023. PMID: 38003913 Free PMC article.
-
Inhibition of NAMPT as a therapeutic strategy to suppress tumor growth in lymphangioleiomyomatosis.Biochim Biophys Acta Mol Cell Res. 2025 Aug;1872(6):119986. doi: 10.1016/j.bbamcr.2025.119986. Epub 2025 May 8. Biochim Biophys Acta Mol Cell Res. 2025. PMID: 40348345
References
-
- McCormack FX, Gupta N, Finlay GR, Young LR, Taveira-DaSilva AM, Glasgow CG, Steagall WK, Johnson SR, Sahn SA, Ryu JH, Strange C, Seyama K, Sullivan EJ, Kotloff RM, Downey GP, Chapman JT, Han MK, D'Armiento JM, Inoue Y, Henske EP, Bissler JJ, Colby TV, Kinder BW, Wikenheiser-Brokamp KA, Brown KK, Cordier JF, Meyer C, Cottin V, Brozek JL, Smith K, Wilson KC, Moss J; ATS/JRS Committee on Lymphangioleiomyomatosis. Official American Thoracic Society/Japanese Respiratory Society Clinical Practice Guidelines: lymphangioleiomyomatosis diagnosis and management. Am J Respir Crit Care Med 194: 748–761, 2016. doi:10.1164/rccm.201607-1384ST. - DOI - PMC - PubMed
-
- Johnson SR, Cordier JF, Lazor R, Cottin V, Costabel U, Harari S, Reynaud-Gaubert M, Boehler A, Brauner M, Popper H, Bonetti F, Kingswood C; Review Panel of the ERS LAM Task Force. European Respiratory Society guidelines for the diagnosis and management of lymphangioleiomyomatosis. Eur Respir J 35: 14–26, 2010. doi:10.1183/09031936.00076209. - DOI - PubMed
-
- Harknett EC, Chang WY, Byrnes S, Johnson J, Lazor R, Cohen MM, Gray B, Geiling S, Telford H, Tattersfield AE, Hubbard RB, Johnson SR. Use of variability in national and regional data to estimate the prevalence of lymphangioleiomyomatosis. QJM 104: 971–979, 2011. doi:10.1093/qjmed/hcr116. - DOI - PubMed
Publication types
MeSH terms
Substances
Grants and funding
LinkOut - more resources
Full Text Sources
Medical
Miscellaneous

