General practitioners' everyday clinical decision-making on psychosocial problems of children and youth in the Netherlands
- PMID: 36576906
- PMCID: PMC9797081
- DOI: 10.1371/journal.pone.0278314
General practitioners' everyday clinical decision-making on psychosocial problems of children and youth in the Netherlands
Abstract
Background: Psychosocial problems in children and youth are common and may negatively impact their lives and the lives of their families. Since general practitioners (GPs) play a crucial role in detecting and intervening in such problems, it is clinically necessary to improve our insight into their clinical decision-making (CDM). The objective of this study was to explore which mechanisms underlie GPs' everyday CDM and their options for management or referral.
Material and methods: This was a mixed methods study in which qualitative (interview substudy) and quantitative (online survey substudy) data were collected from GPs. Using a question framework and vignettes representative of clinical practice, GPs' CDM was explored. GPs were selected by means of an academic research network and purposive sampling. Data collection continued in constant comparison between both substudies. Using grounded theory, data from both substudies were triangulated into a flowchart consisting of mechanisms and management/referral options.
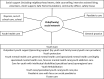
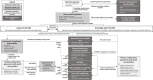
Results: CDM-mechanisms were divided into three groups. GP-related mechanisms were GPs' primary approach of the problem (somatically or psychosocially) and their self-assessed competence to solve the problem based on interest in and knowledge about youth mental health care. Mechanisms related to the child and its social context included GPs' assessment whether there was psychiatric (co)morbidity, their sense of self-limitedness of the problem and assessed complexity of the problem. Whether GPs' had existing collaboration agreements with youth care providers and how they experienced their collaboration were collaboration-related mechanisms.
Conclusion: The current study contributes to a relatively unexplored research area by revealing GP's in-depth thought processes regarding their CDM. However, existing research in this area supports the identified CDM mechanisms. Future initiatives should focus on validating CDM mechanisms in a larger population. If confirmed, mechanisms could be integrated into GP training and may offer guidelines for regulating proper access to mental health care services.
Copyright: © 2022 van Venrooij et al. This is an open access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.
Conflict of interest statement
The authors have declared that no competing interests exist.
Figures

References
MeSH terms
LinkOut - more resources
Full Text Sources
Miscellaneous

