A 3-hour fast-track extubation protocol for early extubation after cardiac surgery
- PMID: 36590715
- PMCID: PMC9801240
- DOI: 10.1016/j.xjon.2022.07.006
A 3-hour fast-track extubation protocol for early extubation after cardiac surgery
Abstract
Objectives: Early extubation after cardiac surgery improves outcomes and reduces cost. We investigated the effect of a multidisciplinary 3-hour fast-track protocol on extubation, intensive care unit length of stay time, and reintubation rate after a wide range of cardiac surgical procedures.
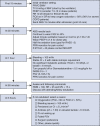
Methods: We performed an observational study of 472 adult patients undergoing cardiac surgery at a large academic institution. A multidisciplinary 3-hour fast-track protocol was applied to a wide range of cardiac procedures. Data were collected 4 months before and 6 months after protocol implementation. Cox regression model assessed factors associated with extubation time and intensive care unit length of stay.
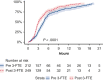
Results: A total of 217 patients preprotocol implementation and 255 patients postprotocol implementation were included. Baseline characteristics were similar except for the median procedure time and dexmedetomidine use. The median extubation time was reduced by 44% (4:43 hours vs 3:08 hours; P < .001) in the postprotocol group. Extubation within 3 hours was achieved in 49.4% of patients in the postprotocol group compared with 25.8% patients in the preprotocol group; P < .001. There was no statistically significant difference in the intensive care unit length of stay after controlling for other factors. Early extubation was associated with only 1 patient requiring reintubation in the postprotocol group.
Conclusions: The multidisciplinary 3-hour fast-track extubation protocol is a safe and effective tool to further reduce the duration of mechanical ventilation after a wide range of cardiac surgical procedures. The protocol implementation did not decrease the intensive care unit length of stay.
Keywords: 3-FTE, 3-hour fast-track extubation; AVR, aortic valve replacement; CABG, coronary artery bypass grafting; IABP, intra-aortic balloon pump; ICU, intensive care unit; LOS, length of stay; cardiac surgery; early extubation; multidisciplinary protocol.
© 2022 The Authors. Published by Elsevier Inc. on behalf of The American Association for Thoracic Surgery.
Figures




References
-
- Cheng D.C., Karski J., Peniston C., Asokumar B., Raveendran G., Carroll J., et al. Morbidity outcome in early versus conventional tracheal extubation after coronary artery bypass grafting: a prospective randomized controlled trial. J Thorac Cardiovasc Surg. 1996;112:755–764. - PubMed
-
- Bonten M.J., Kollef M.H., Hall J.B. Risk factors for ventilator-associated pneumonia: from epidemiology to patient management. Clin Infect Dis. 2004;38:1141–1149. - PubMed
-
- He S., Chen B., Li W., Yan J., Chen L., Wang X., et al. Ventilator-associated pneumonia after cardiac surgery: a meta-analysis and systematic review. J Thorac Cardiovasc Surg. 2014;148:3148–3155. - PubMed
-
- Hansen-Flaschen J.H., Brazinsky S., Basile C., Lanken P.N. Use of sedating drugs and neuromuscular blocking agents in patients requiring mechanical ventilation for respiratory failure: a national survey. JAMA. 1991;266:2870–2875. - PubMed
-
- van Mastrigt G.A., Maessen J.G., Heijmans J., Severens J.L., Prins M.H. Does fast-track treatment lead to a decrease of intensive care unit and hospital length of stay in coronary artery bypass patients? A meta-regression of randomized clinical trials. Crit Care Med. 2006;34:1624–1634. - PubMed
LinkOut - more resources
Full Text Sources

